Bill Medford, MSK Ultrasonographer, SonoSite Fujifilm04.12.16
With its diagnostic accuracy and absence of radiation exposure, ultrasound is now poised to make a larger and more positive impact on musculoskeletal (MSK) medicine, the latest of the fields to recognize the clinical and economic benefits of ultrasound. Recognizing the gains to be made in both cost reduction and patient safety, the Centers for Medicare and Medicaid Services (CMS) is currently designing the implementation of Appropriate Use Criteria (AUC) for medical imaging that favors ultrasound as the initial procedure of choice for several applications. These criteria go into effect January 1, 2017.
The lag between solid evidence of ultrasound’s advantages for MSK and its widespread adoption is largely born of inertia, which has allowed the companies that develop the technology to address remaining technical barriers to use.
Ultrasound in MSK: Why and When?
The literature is very clear that for many musculoskeletal applications, ultrasound should be the preferred technique for initial evaluations. For example, since as far back as 1984, numerous studies have shown ultrasound’s accuracy in recognizing the presence or absence of a rotator cuff tear is equal to that of MRI, while costing up to 5 times less and taking a fraction of the time. Why then are rotator cuffs still screened nearly exclusively with MRI? Because in the United States, MRI is ubiquitous—the availability of MRI and the practice pattern of specialists is to order the MRI. And when physicians are fluent with a specific technology, it is difficult to change that practice.
That’s where AUC comes in. Led by professional organizations and physician groups, the development of these criteria will be grounded in evidence rather than tradition or preference. These guidelines are not rigid—they won’t rule out MRI when looking inside the joint, of course, as ultrasound cannot penetrate bone—but they do codify when ultrasound is the more appropriate initial procedure of choice.
Following are three specific MSK applications where ultrasound technology might best be considered the initial procedure of choice, but should certainly be used more frequently:
SonoSite understands that because the evidence is ahead of current practice in MSK, there’s a higher bar for the technology to be user friendly. Thus, while there are artifacts in all forms of imaging, the artifacts typically found in MRIs—visual artifacts off of surgical hardware—make ultrasound the obvious option for assessing any postoperative rotator cuff for re-tear.
Artifacts in ultrasound make it more difficult to determine whether a structure that’s echo-free should be echo-free and, therefore, fluid, or whether any visible echoes are real or artifactual. The ability to differentiate solid from fluid is much easier with a low-artifact image.
With the company’s release of X-porte and XDI, the engineers developing the system have found a way to reduce and nearly eliminate what’s called side-lobe artifact, which has always been a challenge for ultrasound. (Side-lobe artifacts are a scatter of echoes that a user gets in that portion of the sound beam where the beam does not focus.) Extreme definition imaging has resulted in a significantly more artifact-free image than what had been commercially available at any time in the past. Any time the resolution on any imaging modality is improved, it allows for increased confidence in what’s being visualized. That leap in the technology, and its ease of use even for physicians better versed in MRI, will lead to more definitive recognition of musculoskeletal pathologies.
Conclusion
When physicians experience success with an approach or technique they’ve practiced for years, changing midstream to something new entails a learning curve that few want to follow. SonoSite has removed one of the objections to switching systems by clarifying the image so that there is no loss of diagnostic confidence for MSK evaluations (and, in the cases discussed above, there are significant diagnostic advantages). Obstetricians once resisted using ultrasound to place a needle into the pregnant uterus; they had to be convinced that ultrasound would offer them more precision, higher accuracy, and ultimately, greater confidence.
While it’s been a long process to see ultrasound embraced in musculoskeletal use, the combination of superior quality technology and external pressure are propelling it in the right direction.
Bill Medford was a clinically-based sonographer for 32 years, handling all aspects of ultrasound except echocardiography. He has more recently been with SonoSite for the past 5 years.
The lag between solid evidence of ultrasound’s advantages for MSK and its widespread adoption is largely born of inertia, which has allowed the companies that develop the technology to address remaining technical barriers to use.
Ultrasound in MSK: Why and When?
The literature is very clear that for many musculoskeletal applications, ultrasound should be the preferred technique for initial evaluations. For example, since as far back as 1984, numerous studies have shown ultrasound’s accuracy in recognizing the presence or absence of a rotator cuff tear is equal to that of MRI, while costing up to 5 times less and taking a fraction of the time. Why then are rotator cuffs still screened nearly exclusively with MRI? Because in the United States, MRI is ubiquitous—the availability of MRI and the practice pattern of specialists is to order the MRI. And when physicians are fluent with a specific technology, it is difficult to change that practice.
That’s where AUC comes in. Led by professional organizations and physician groups, the development of these criteria will be grounded in evidence rather than tradition or preference. These guidelines are not rigid—they won’t rule out MRI when looking inside the joint, of course, as ultrasound cannot penetrate bone—but they do codify when ultrasound is the more appropriate initial procedure of choice.
Following are three specific MSK applications where ultrasound technology might best be considered the initial procedure of choice, but should certainly be used more frequently:
-
Rotator cuff tears and follow-up evaluation
Ultrasound is optimal for applications involving soft tissue, and one of the most common MSK issues is injury to the rotator cuff. Given the image clarity ultrasound systems can offer, this option can be both quicker and equally definitive on diagnosing whether there is a tear or not? -
Achilles tendinopathy
With MRI, in some cases, it can be difficult to differentiate complete from partial Achilles tendon tears. Are there still a few tendon fibers intact? With ultrasound, dynamic assessment during flexion/extension of the foot will demonstrate the sliding motion of an intact or partially intact tendon. Assessing Achilles tendon injuries is, like rotator cuff tears, where ultrasound holds a distinct advantage over a static imaging technique like MRI. -
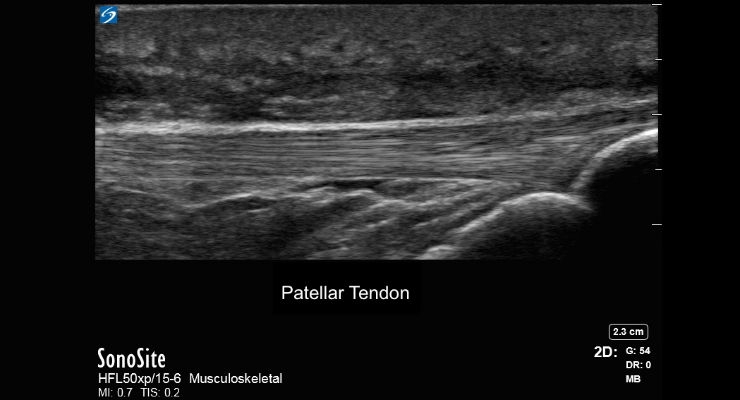
Repetitive stress injuries related to tendon issues
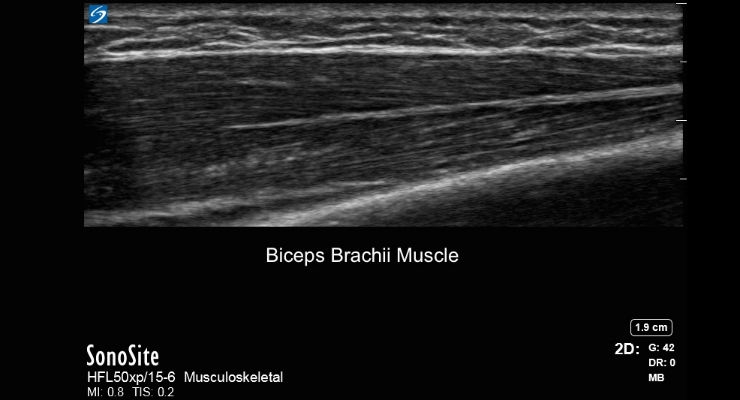
Some of the most common issues for the athlete—the high performance athlete in particular—are repetitive stress injuries to tendons. Ultrasound is very good at recognizing what is called tendonopathy, which can range widely in acuity. Ultrasound allows physicians to warn athletes when a tendon is inflamed or suffering degeneration, because all tendons have a distinctly crisp, fibrillar pattern when normal on ultrasound. As well, ultrasound is very sensitive in distinguishing between a muscle tear or strain, thus furnishing better (and more easily obtained) information about when the athlete can return to play.
SonoSite understands that because the evidence is ahead of current practice in MSK, there’s a higher bar for the technology to be user friendly. Thus, while there are artifacts in all forms of imaging, the artifacts typically found in MRIs—visual artifacts off of surgical hardware—make ultrasound the obvious option for assessing any postoperative rotator cuff for re-tear.
Artifacts in ultrasound make it more difficult to determine whether a structure that’s echo-free should be echo-free and, therefore, fluid, or whether any visible echoes are real or artifactual. The ability to differentiate solid from fluid is much easier with a low-artifact image.
With the company’s release of X-porte and XDI, the engineers developing the system have found a way to reduce and nearly eliminate what’s called side-lobe artifact, which has always been a challenge for ultrasound. (Side-lobe artifacts are a scatter of echoes that a user gets in that portion of the sound beam where the beam does not focus.) Extreme definition imaging has resulted in a significantly more artifact-free image than what had been commercially available at any time in the past. Any time the resolution on any imaging modality is improved, it allows for increased confidence in what’s being visualized. That leap in the technology, and its ease of use even for physicians better versed in MRI, will lead to more definitive recognition of musculoskeletal pathologies.
Conclusion
When physicians experience success with an approach or technique they’ve practiced for years, changing midstream to something new entails a learning curve that few want to follow. SonoSite has removed one of the objections to switching systems by clarifying the image so that there is no loss of diagnostic confidence for MSK evaluations (and, in the cases discussed above, there are significant diagnostic advantages). Obstetricians once resisted using ultrasound to place a needle into the pregnant uterus; they had to be convinced that ultrasound would offer them more precision, higher accuracy, and ultimately, greater confidence.
While it’s been a long process to see ultrasound embraced in musculoskeletal use, the combination of superior quality technology and external pressure are propelling it in the right direction.
Bill Medford was a clinically-based sonographer for 32 years, handling all aspects of ultrasound except echocardiography. He has more recently been with SonoSite for the past 5 years.