Roger Massengale, General Manager, Acute Pain, Halyard Health03.08.17
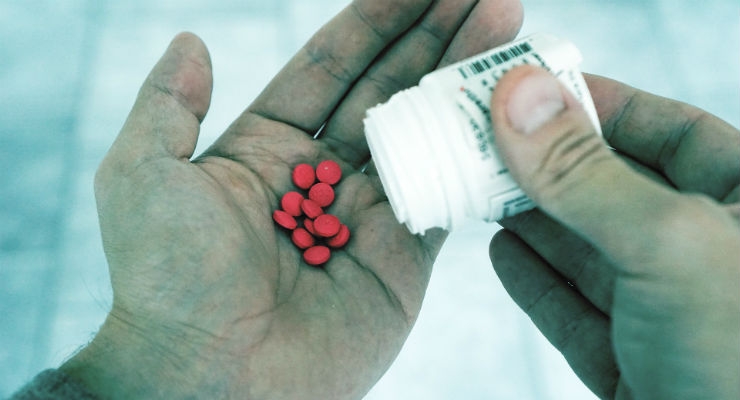
The country is witnessing a massive opioid epidemic, opioid-related accidental deaths, and overuse of prescription drugs for pain. Despite making up only 4.6 percent of the world population, the United States uses 80 percent of the global opioid supply,1 and 4.3 million Americans aged 12 or older reported current nonmedical use of prescription pain relievers in 2014.2 Opioids prescribed post-surgery play a major role here, with one study of 391,139 surgical patients finding that 10.3 percent of patients who were prescribed opioids within seven days of surgery were still using those medications one year later.3
Until recently, post-operative pain was primarily treated with opioids—and according to the CDC, the increase in opioid prescribing is a contributing factor to the increase of prescription overdoses.4 Opioid-based pain medications may produce significant adverse effects, with both clinical and financial consequences. These medications pose the risk of opioid addiction/physical dependence and may lead to complications like respiratory depression, constipation, sedation, nausea, vomiting, and dizziness.5

Roger Massengale, General Manager, Acute Pain, Halyard Health
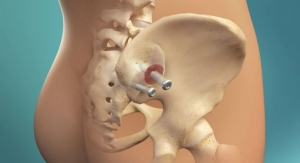
Fortunately, there are technologies and treatment approaches available that can effectively manage pain following surgery without relying on opioids. These treatments include regional nerve blocks, periarticular injections, neuraxial anesthesia, and non-opioid oral and intravenous medications.6
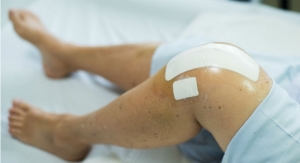
Research suggests that use of non-opioid treatments like regional nerve blocks may provide patients with superior acute postoperative pain relief, while decreasing the amount of opioid-related adverse effects. In fact, a 2014 study found that the use of a femoral nerve block resulted in less pain for patients during the first 72 hours after knee replacement surgery, in addition to lower opioid consumption, less nausea and vomiting, higher patient satisfaction, and greater knee flexion compared to use of opioids alone.7
Many patients may still be unaware that there are alternatives to opioids for post-surgical pain relief. By placing a stronger emphasis on patient education regarding opioids, and the alternatives available, healthcare professionals can contribute to curbing the opioid epidemic, while improving the overall patient experience.
References
1 Manchikanti L, Singh A. Therapeutic opioids: a ten-year perspective on the complexities and complications of escalating use, abuse, and nonmedical use of opioids. Pain Physician. 2008;11(2 Suppl):S63-S88
2 Hedden SL, Kennet J, Lipari R, et al. [Internet] Rockville, MD: SAMHSA; c2016 [updated 2015 Sept; cited 2016 Dec 6]. Behavioral Health Trends in the United States: Results from the 2014 National Survey on Drug Use and Health; [about 2 screens]. Available from: http://www.samhsa.gov/data/sites/default/files/NSDUH-FRR1-2014/NSDUH-FRR1-2014.pdf
3 Alam A, Gomes T, Zheng H, Mamdani MM, Juurlink DN, Bell CM. Long-term Analgesic Use After Low-Risk Surgery A Retrospective Cohort Study. Arch Intern Med. 2012;172(5):425-430.
4 CDC Vital Signs [Internet]. Atlanta: Centers for Disease Control and Prevention; c2016 [updated 2014 Jul; cited 2016 Dec 6]. Opioid Painkiller Prescribing: Where You Live Makes a Difference; [about 4 screens]. Available from: https://www.cdc.gov/vitalsigns/pdf/2014-07-vitalsigns.pdf
5 Benyamin R, Trescot AM, Datta S, et al. Opioid complications and side effects. Pain Physician. 2008;11:s105-s120.
6 Parvizi J, Bloomfield MR. Multimodal pain management in orthopedics: implications for joint arthroplasty surgery. Orthopedics. 2013;36(2 Suppl):7-14.
7 Chan EY, Fransen M, Parker DA, Assam PN, Chua N. Femoral nerve blocks for acute postoperative pain after knee replacement surgery. Cochrane Database Syst Rev. 2014 May 13;(5):CD009941.
Until recently, post-operative pain was primarily treated with opioids—and according to the CDC, the increase in opioid prescribing is a contributing factor to the increase of prescription overdoses.4 Opioid-based pain medications may produce significant adverse effects, with both clinical and financial consequences. These medications pose the risk of opioid addiction/physical dependence and may lead to complications like respiratory depression, constipation, sedation, nausea, vomiting, and dizziness.5

Roger Massengale, General Manager, Acute Pain, Halyard Health
Research suggests that use of non-opioid treatments like regional nerve blocks may provide patients with superior acute postoperative pain relief, while decreasing the amount of opioid-related adverse effects. In fact, a 2014 study found that the use of a femoral nerve block resulted in less pain for patients during the first 72 hours after knee replacement surgery, in addition to lower opioid consumption, less nausea and vomiting, higher patient satisfaction, and greater knee flexion compared to use of opioids alone.7
Many patients may still be unaware that there are alternatives to opioids for post-surgical pain relief. By placing a stronger emphasis on patient education regarding opioids, and the alternatives available, healthcare professionals can contribute to curbing the opioid epidemic, while improving the overall patient experience.
References
1 Manchikanti L, Singh A. Therapeutic opioids: a ten-year perspective on the complexities and complications of escalating use, abuse, and nonmedical use of opioids. Pain Physician. 2008;11(2 Suppl):S63-S88
2 Hedden SL, Kennet J, Lipari R, et al. [Internet] Rockville, MD: SAMHSA; c2016 [updated 2015 Sept; cited 2016 Dec 6]. Behavioral Health Trends in the United States: Results from the 2014 National Survey on Drug Use and Health; [about 2 screens]. Available from: http://www.samhsa.gov/data/sites/default/files/NSDUH-FRR1-2014/NSDUH-FRR1-2014.pdf
3 Alam A, Gomes T, Zheng H, Mamdani MM, Juurlink DN, Bell CM. Long-term Analgesic Use After Low-Risk Surgery A Retrospective Cohort Study. Arch Intern Med. 2012;172(5):425-430.
4 CDC Vital Signs [Internet]. Atlanta: Centers for Disease Control and Prevention; c2016 [updated 2014 Jul; cited 2016 Dec 6]. Opioid Painkiller Prescribing: Where You Live Makes a Difference; [about 4 screens]. Available from: https://www.cdc.gov/vitalsigns/pdf/2014-07-vitalsigns.pdf
5 Benyamin R, Trescot AM, Datta S, et al. Opioid complications and side effects. Pain Physician. 2008;11:s105-s120.
6 Parvizi J, Bloomfield MR. Multimodal pain management in orthopedics: implications for joint arthroplasty surgery. Orthopedics. 2013;36(2 Suppl):7-14.
7 Chan EY, Fransen M, Parker DA, Assam PN, Chua N. Femoral nerve blocks for acute postoperative pain after knee replacement surgery. Cochrane Database Syst Rev. 2014 May 13;(5):CD009941.