Sean Fenske, Editor03.22.17
We are in a fantastic age of materials innovation, with so many new options emerging rapidly. Graphene is creating great excitement and could one day prove to be a fantastic material with virtually unlimited applications, both in and out of healthcare. Hybrid materials such as drug-infused options can help promote healing or prevent potential infection. Ceramics are finding their way into the body due to the biocompatibility, favorable wear characteristics, and strength these materials offer. Even still, biomaterials are emerging that promote a more natural solution, helping to restore more normal form, fit, and function.
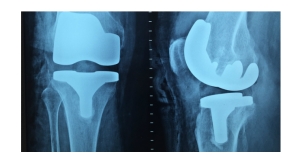
That said, in the orthopedic industry today, there is still an unsettled debate that essentially boils down to two material options: metal or plastic. When I attended the North American Spine Society annual meeting last year, this was quite apparent. Those manufacturers working with metal touted the benefits of the material, stating how orthopedic device makers were getting back to using the option in significant numbers. They explained how many of the limitations or concerns with metal were improving or had been resolved. Meanwhile, those delivering technologies made from plastic were quick to point to how much of the industry had shifted to the plastic alternative. Especially in spinal implants, PEEK had gained significant ground when compared to metal and it resolved some of the concerns with using it.
Truth is, the debate is far from being resolved. I even encountered one person on the metal side of the debate who jokingly asked, “Does anyone even make plastic implants anymore?” Had he taken a moment to walk the exhibit floor at the event, he would have quickly had an answer.
Another truth of this discussion, both sides—plastic and metal—have their shortcomings and neither is still the perfect solution for orthopedics. They are, however, the best options we have for mass-produced orthopedic instruments and implants. Still another truth, albeit a somewhat unfortunate one, is this will likely be the case for many years to come. A substantial change in material options is not going to emerge anytime soon.
When I wrote my Editor’s Letter about the transformation of the spinal industry in the November/December 2016 issue, I cited a possible 10-year timeframe in which the current industry would see the widespread adoption of biomaterials. These would end the debate over metal or plastic for spinal implants. Given time to ponder this claim, I think 10 years is likely a bit too optimistic, but considering what’s happening today, I think it’s probably the low-end of the spectrum. I don’t think 20 years is unrealistic at all, and it may be more likely somewhere in the middle when we see the shift in materials for spinal implants.
As for other orthopedic specialties, the timetable is less clear and dependent upon the application. I will say that I think the ultimate winner in the materials debate will be neither metal or plastic, but rather biomaterials in all areas of orthopedics. Again, the timing will be dependent upon the advancement of these material options and the application, what properties are required, and how quickly they can enhance healing of a damaged bone, muscle, or tissue. Metal or plastic may play a supporting role in the use of biomaterials, but the primary material “champion” will be these options that help restore more of the body’s natural anatomy or accelerate healing.
In addition to revolutionary materials, the orthopedic sector will be aided significantly by a rapidly emerging manufacturing process. Termed additive manufacturing and more commonly known as 3D printing, this fabrication process will help orthopedic device manufacturers get more from the materials with which they are working—metal, plastic, or otherwise. Better designs that can only be achieved using this layered process will reduce material waste and enable patient-specific implants, guides, and instrumentation. Further, because of the custom capabilities 3D printing offers, replacement bone will be fit exactly to the remaining natural bone that’s left following trauma or removal due to disease.
Unfortunately, even 3D printing has its drawbacks. For now, the main concerns are manufacture times and material costs. Timing can be addressed with more preparation prior to surgery, which is actually already taking place when companies like ConforMIS are supplying the implant for a knee replacement. But beyond that, no company that I’m aware of is capable of providing custom implants for any other area of the body. Material costs, on the other hand, will be an ongoing struggle between the raw materials supplier and the manufacturer processing it to be used in the body.
There are more insights into this discussion and the impact of materials in orthopedics in this month’s cover story.
That said, in the orthopedic industry today, there is still an unsettled debate that essentially boils down to two material options: metal or plastic. When I attended the North American Spine Society annual meeting last year, this was quite apparent. Those manufacturers working with metal touted the benefits of the material, stating how orthopedic device makers were getting back to using the option in significant numbers. They explained how many of the limitations or concerns with metal were improving or had been resolved. Meanwhile, those delivering technologies made from plastic were quick to point to how much of the industry had shifted to the plastic alternative. Especially in spinal implants, PEEK had gained significant ground when compared to metal and it resolved some of the concerns with using it.
Truth is, the debate is far from being resolved. I even encountered one person on the metal side of the debate who jokingly asked, “Does anyone even make plastic implants anymore?” Had he taken a moment to walk the exhibit floor at the event, he would have quickly had an answer.
Another truth of this discussion, both sides—plastic and metal—have their shortcomings and neither is still the perfect solution for orthopedics. They are, however, the best options we have for mass-produced orthopedic instruments and implants. Still another truth, albeit a somewhat unfortunate one, is this will likely be the case for many years to come. A substantial change in material options is not going to emerge anytime soon.
When I wrote my Editor’s Letter about the transformation of the spinal industry in the November/December 2016 issue, I cited a possible 10-year timeframe in which the current industry would see the widespread adoption of biomaterials. These would end the debate over metal or plastic for spinal implants. Given time to ponder this claim, I think 10 years is likely a bit too optimistic, but considering what’s happening today, I think it’s probably the low-end of the spectrum. I don’t think 20 years is unrealistic at all, and it may be more likely somewhere in the middle when we see the shift in materials for spinal implants.
As for other orthopedic specialties, the timetable is less clear and dependent upon the application. I will say that I think the ultimate winner in the materials debate will be neither metal or plastic, but rather biomaterials in all areas of orthopedics. Again, the timing will be dependent upon the advancement of these material options and the application, what properties are required, and how quickly they can enhance healing of a damaged bone, muscle, or tissue. Metal or plastic may play a supporting role in the use of biomaterials, but the primary material “champion” will be these options that help restore more of the body’s natural anatomy or accelerate healing.
In addition to revolutionary materials, the orthopedic sector will be aided significantly by a rapidly emerging manufacturing process. Termed additive manufacturing and more commonly known as 3D printing, this fabrication process will help orthopedic device manufacturers get more from the materials with which they are working—metal, plastic, or otherwise. Better designs that can only be achieved using this layered process will reduce material waste and enable patient-specific implants, guides, and instrumentation. Further, because of the custom capabilities 3D printing offers, replacement bone will be fit exactly to the remaining natural bone that’s left following trauma or removal due to disease.
Unfortunately, even 3D printing has its drawbacks. For now, the main concerns are manufacture times and material costs. Timing can be addressed with more preparation prior to surgery, which is actually already taking place when companies like ConforMIS are supplying the implant for a knee replacement. But beyond that, no company that I’m aware of is capable of providing custom implants for any other area of the body. Material costs, on the other hand, will be an ongoing struggle between the raw materials supplier and the manufacturer processing it to be used in the body.
There are more insights into this discussion and the impact of materials in orthopedics in this month’s cover story.