PR Newswire05.01.17
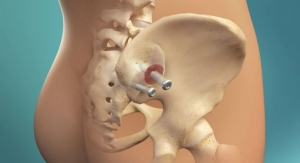
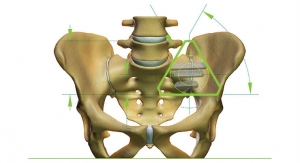
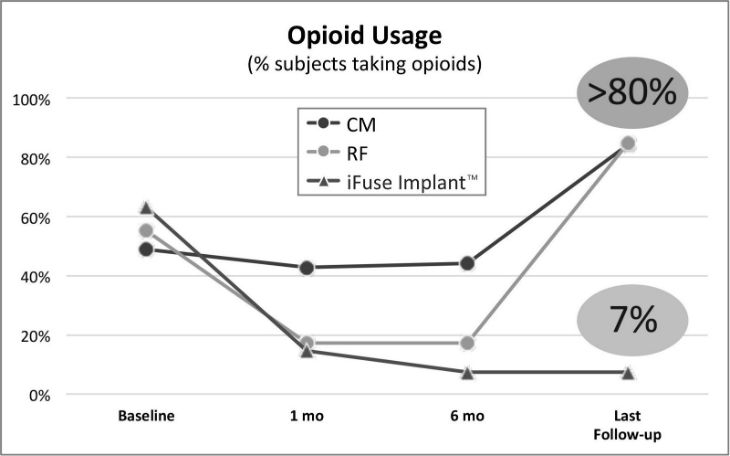
SI-BONE Inc., a medical device company that pioneered the use of the iFuse Implant System ("iFuse"), a triangular shaped minimally invasive surgical (MIS) device indicated for fusion for certain disorders of the sacroiliac (SI) joint, announced results from two recently published comparative studies showed patients treated with the iFuse Implant were significantly less likely to be taking opioid medications than patients treated with non-surgical care. The most recently published paper titled Minimally Invasive Sacroiliac Joint Fusion, Radiofrequency Denervation and Conservative Management for Sacroiliac Joint Pain: Six Year Comparative Study,1 published in the journal Neurosurgery, showed that patients treated with iFuse were 11X less likely to be taking opioids at last follow-up than those who were denied coverage for iFuse and treated with either conservative care or radiofrequency ablation (>80% vs, 7%) (Figure 1, below).
"Given the catastrophic opioid addiction epidemic we are currently dealing with in this country today, any procedure, device or technology that demonstrates the ability to significantly reduce opioid use should be made available to anyone who can benefit," said Frank Guinta, former New Hampshire congressman and co-founder of the Congressional Bipartisan Committee on opioid and heroin addiction. "Given the overwhelming amount of high quality level 1 clinical evidence associated with the iFuse Implant, it seems prudent and obvious to me that anyone properly diagnosed as an appropriate surgical candidate should have access to the procedure."
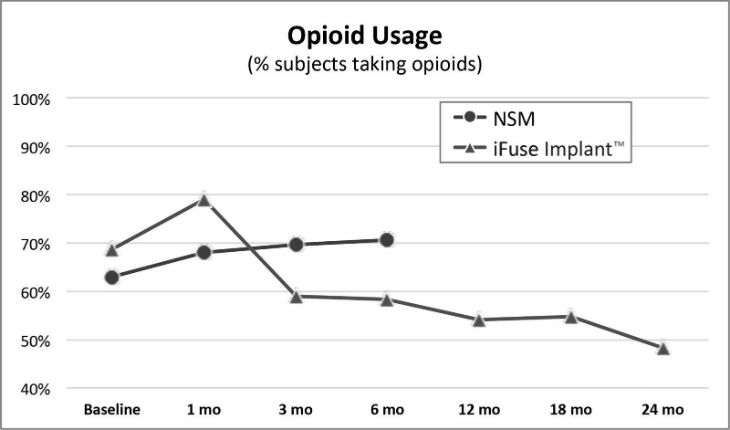
A second publication of two-year results from INSITE,2 a randomized controlled trial of MIS SI joint fusion with the iFuse Implant compared to non-surgical management, showed a 30% decrease from baseline in the number of subjects taking opioids at two years compared to patients treated non-surgically (Figure 2, below).
"It's rather remarkable that in both studies the number of patients taking opioids in the iFuse Implant group was significantly lower than the number of patients taking opioids in the non-surgical care group in spite of a lack of a structured program focused on opioid use dependence," said Daniel Cher, MD, vice president of clinical affairs at SI-BONE. "It's clear from the evidence in these two studies that treatment with the iFuse Implant was associated with a reduction in opioid use in patients with chronic SI joint pain who were taking opioids and who no longer responded to non-surgical care."
References
1Vanaclocha V, Herrera JM, Sáiz-Sapena N, Rivera-Paz M, Verdú-López F. Minimally Invasive Sacroiliac Joint Fusion, Radiofrequency Denervation and Conservative Management for Sacroiliac Joint Pain: Six Year Comparative Study. Neurosurgery. 2017 April 20. [Epub ahead of print]. doi: 10.1093/neuros/nyx185.
2Polly DW, Swofford J, Whang PG, Frank CJ, Glaser JA, Limoni RP, Cher DJ, Wine KD, Sembrano JN, and the INSITE Study Group. Two-Year Outcomes from a Randomized Controlled Trial of Minimally Invasive Sacroiliac Joint Fusion vs. Non-Surgical Management for Sacroiliac Joint Dysfunction. Int J Spine Surg. 2016;10.Article 28. doi:10.14444/3028.

"Given the catastrophic opioid addiction epidemic we are currently dealing with in this country today, any procedure, device or technology that demonstrates the ability to significantly reduce opioid use should be made available to anyone who can benefit," said Frank Guinta, former New Hampshire congressman and co-founder of the Congressional Bipartisan Committee on opioid and heroin addiction. "Given the overwhelming amount of high quality level 1 clinical evidence associated with the iFuse Implant, it seems prudent and obvious to me that anyone properly diagnosed as an appropriate surgical candidate should have access to the procedure."
A second publication of two-year results from INSITE,2 a randomized controlled trial of MIS SI joint fusion with the iFuse Implant compared to non-surgical management, showed a 30% decrease from baseline in the number of subjects taking opioids at two years compared to patients treated non-surgically (Figure 2, below).

"It's rather remarkable that in both studies the number of patients taking opioids in the iFuse Implant group was significantly lower than the number of patients taking opioids in the non-surgical care group in spite of a lack of a structured program focused on opioid use dependence," said Daniel Cher, MD, vice president of clinical affairs at SI-BONE. "It's clear from the evidence in these two studies that treatment with the iFuse Implant was associated with a reduction in opioid use in patients with chronic SI joint pain who were taking opioids and who no longer responded to non-surgical care."
References
1Vanaclocha V, Herrera JM, Sáiz-Sapena N, Rivera-Paz M, Verdú-López F. Minimally Invasive Sacroiliac Joint Fusion, Radiofrequency Denervation and Conservative Management for Sacroiliac Joint Pain: Six Year Comparative Study. Neurosurgery. 2017 April 20. [Epub ahead of print]. doi: 10.1093/neuros/nyx185.
2Polly DW, Swofford J, Whang PG, Frank CJ, Glaser JA, Limoni RP, Cher DJ, Wine KD, Sembrano JN, and the INSITE Study Group. Two-Year Outcomes from a Randomized Controlled Trial of Minimally Invasive Sacroiliac Joint Fusion vs. Non-Surgical Management for Sacroiliac Joint Dysfunction. Int J Spine Surg. 2016;10.Article 28. doi:10.14444/3028.