Cleveland Clinic03.15.18
A team of researchers led by Cleveland Clinic has published first-of-its-kind findings in Science Translational Medicine on a new method of restoring natural movement sensation in patients with prosthetic arms.
Led by Paul Marasco, Ph.D., the research team has successfully engineered a sense of complex hand movement in patients with upper limb amputations. This breakthrough may enhance the ability to control their prostheses, independently manage activities of daily living and improve quality of life.
“By restoring the intuitive feeling of limb movement—the sensation of opening and closing your hand—we are able to blur the lines between what the patients’ brains perceived as ‘self’ versus ‘machine’,” said Marasco, head of the Laboratory for Bionic Integration in Cleveland Clinic’s Lerner Research Institute. “These findings have important implications for improving human-machine interactions and bring us closer than ever before to providing people with amputation with complete restoration of natural arm function.”
The team used small, but powerful, robots to vibrate specific muscles to “turn on” patients’ sensation of movement, allowing them to feel that their fingers and hands were moving and that they were an integrated part of their own body. By feeling their missing hands while controlling their bionic prostheses, patients in the study could make complex grip patterns to perform specific tasks as well or better than able-bodied people.
“Decades of research has shown that muscles need to sense movement to work properly. This system basically hacks the neural circuits behind that system,” said James W. Gnadt, Ph.D., program director at the National Institute of Neurological Disorders and Stroke, part of the National Institutes of Health which partially supported the study. “This approach takes the field of prosthetic medicine to a new level which we hope will improve the lives of many.”
To improve the relationship between the mind and the prosthesis, the researchers investigated whether they could use a movement illusion to help patients better control their bionic hands. They studied six patients who had previously undergone targeted nerve reinnervation, a procedure that establishes a neural-machine interface by redirecting amputated nerves to remaining muscles. When they vibrated the patients’ reinnervated muscles to provide illusory movement, they not only felt their missing limbs move, but could use these sensations to intentionally manipulate their prostheses to accurately guide complex grips.
This is important because when an able-bodied person moves, the brain constantly receives feedback regarding the movement’s progress. This unconscious sense prevents errors in movement, like overreaching, and allows the body to make necessary adjustments. People with amputation lose this essential feedback, however, and as a result, cannot control their prostheses without having to watch them carefully at all times.

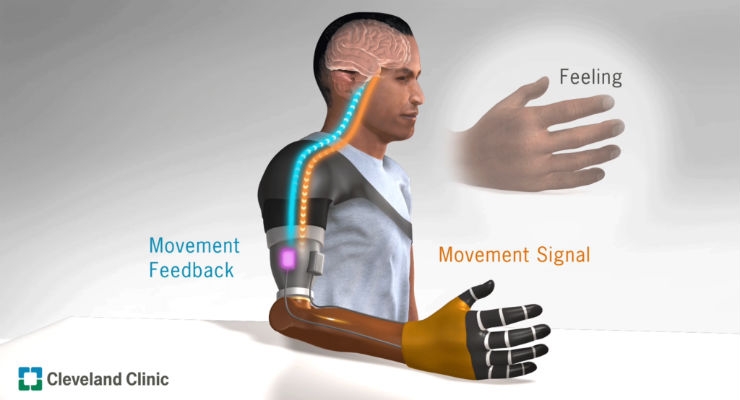
Illusory movement perception improves motor control for prosthetic hands. Image courtesy of Cleveland Clinic.
The new study shows that the sense of missing limb movement, caused by the strategic muscle vibration, provided patients with better spatial awareness and improved fine motor control without having to visually monitor the prostheses. Additionally, the movement sensation made the bionic arms feel more like “self.”
“When you make a movement and then you feel it occur, you intrinsically know that you are the author of that movement and that you have a sense of control or ‘agency’ over your actions,” said Marasco. “People who have had an amputation lose that feeling of control, which leaves them feeling frustrated and disconnected from their prosthetic limbs. The illusions we generate restore the sensation of movement and reestablish their sense of agency over their prosthetics. This helps people with amputation to feel more in control.”
Going forward, the research team is exploring ways to expand these techniques to patients who have lost a leg, as well as for those with conditions that inhibit movement sensation such as stroke. They are also working to package the system into a prosthesis for longer-term applications to enable patients to operate the system on a daily basis.
“The ultimate goal of our research is to use movement sensation to streamline the relationship between patients and their technology, to better integrate their prosthetics as a natural part of themselves,” said Marasco. Marasco is a principal investigator in the Advanced Platform Technology Research Center, Louis Stokes Cleveland Department of Veterans Affairs Medical Center and an associate staff scientist in the Department of Biomedical Engineering in Cleveland Clinic’s Lerner Research Institute. In 2016, he received a Presidential Early Career Award for Scientists and Engineers from former President Barack Obama.
Co-authors on the study included Jacqueline Hebert from the University of Alberta; Jon Sensinger from the University of New Brunswick; Ravi Nataraj from the Stevens Institute of Technology; and Brett Mensh from the Howard Hughes Medical Institute.
This study was funded through a National Institutes of Health, Office of the Director, Common Fund, Transformative R01 Research Award, # 1R01NS081710 – 01.
Led by Paul Marasco, Ph.D., the research team has successfully engineered a sense of complex hand movement in patients with upper limb amputations. This breakthrough may enhance the ability to control their prostheses, independently manage activities of daily living and improve quality of life.
“By restoring the intuitive feeling of limb movement—the sensation of opening and closing your hand—we are able to blur the lines between what the patients’ brains perceived as ‘self’ versus ‘machine’,” said Marasco, head of the Laboratory for Bionic Integration in Cleveland Clinic’s Lerner Research Institute. “These findings have important implications for improving human-machine interactions and bring us closer than ever before to providing people with amputation with complete restoration of natural arm function.”
The team used small, but powerful, robots to vibrate specific muscles to “turn on” patients’ sensation of movement, allowing them to feel that their fingers and hands were moving and that they were an integrated part of their own body. By feeling their missing hands while controlling their bionic prostheses, patients in the study could make complex grip patterns to perform specific tasks as well or better than able-bodied people.
“Decades of research has shown that muscles need to sense movement to work properly. This system basically hacks the neural circuits behind that system,” said James W. Gnadt, Ph.D., program director at the National Institute of Neurological Disorders and Stroke, part of the National Institutes of Health which partially supported the study. “This approach takes the field of prosthetic medicine to a new level which we hope will improve the lives of many.”
To improve the relationship between the mind and the prosthesis, the researchers investigated whether they could use a movement illusion to help patients better control their bionic hands. They studied six patients who had previously undergone targeted nerve reinnervation, a procedure that establishes a neural-machine interface by redirecting amputated nerves to remaining muscles. When they vibrated the patients’ reinnervated muscles to provide illusory movement, they not only felt their missing limbs move, but could use these sensations to intentionally manipulate their prostheses to accurately guide complex grips.
This is important because when an able-bodied person moves, the brain constantly receives feedback regarding the movement’s progress. This unconscious sense prevents errors in movement, like overreaching, and allows the body to make necessary adjustments. People with amputation lose this essential feedback, however, and as a result, cannot control their prostheses without having to watch them carefully at all times.

Illusory movement perception improves motor control for prosthetic hands. Image courtesy of Cleveland Clinic.
The new study shows that the sense of missing limb movement, caused by the strategic muscle vibration, provided patients with better spatial awareness and improved fine motor control without having to visually monitor the prostheses. Additionally, the movement sensation made the bionic arms feel more like “self.”
“When you make a movement and then you feel it occur, you intrinsically know that you are the author of that movement and that you have a sense of control or ‘agency’ over your actions,” said Marasco. “People who have had an amputation lose that feeling of control, which leaves them feeling frustrated and disconnected from their prosthetic limbs. The illusions we generate restore the sensation of movement and reestablish their sense of agency over their prosthetics. This helps people with amputation to feel more in control.”
Going forward, the research team is exploring ways to expand these techniques to patients who have lost a leg, as well as for those with conditions that inhibit movement sensation such as stroke. They are also working to package the system into a prosthesis for longer-term applications to enable patients to operate the system on a daily basis.
“The ultimate goal of our research is to use movement sensation to streamline the relationship between patients and their technology, to better integrate their prosthetics as a natural part of themselves,” said Marasco. Marasco is a principal investigator in the Advanced Platform Technology Research Center, Louis Stokes Cleveland Department of Veterans Affairs Medical Center and an associate staff scientist in the Department of Biomedical Engineering in Cleveland Clinic’s Lerner Research Institute. In 2016, he received a Presidential Early Career Award for Scientists and Engineers from former President Barack Obama.
Co-authors on the study included Jacqueline Hebert from the University of Alberta; Jon Sensinger from the University of New Brunswick; Ravi Nataraj from the Stevens Institute of Technology; and Brett Mensh from the Howard Hughes Medical Institute.
This study was funded through a National Institutes of Health, Office of the Director, Common Fund, Transformative R01 Research Award, # 1R01NS081710 – 01.