Michael Barbella, Managing Editor05.04.21
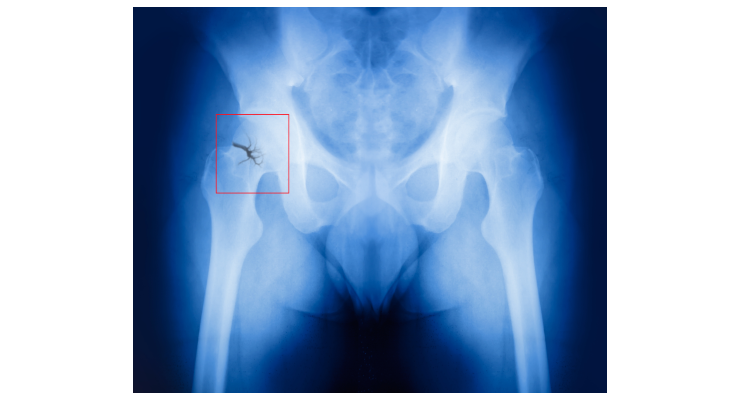
A new study assessing postoperative complications from hip fracture repair concludes that two problems in particular are associated with high mortality rates.
The study, “The Relative Impact of Specific Postoperative Complications on Older Patients Undergoing Hip Fracture Repair," details the ways in which researchers used data for patients aged 65 years and older from the 2016-2017 Hip Fracture Targeted American College of Surgeons National Surgical Quality Improvement program (ACS NSQIP) to reach their conclusions. Hip fracture in older patients is common, debilitating and costly.1,2,3
Population attributable fractions (PAFs) were used to quantify the anticipated reduction in the primary outcomes (30-day mortality and readmission) that would result from complete prevention of 10 postoperative complications. In 17,755 patients who underwent hip fracture repair in 117 hospitals, postoperative delirium and pneumonia were the highest-impact complications.
Postoperative delirium affected 29.8 percent of patients and was associated with:
The impact of the other eight complications – bleeding, Clostridium difficile colitis, decubitus ulcer, myocardial infarction, stroke, surgical site infection, urinary tract infection and venous thromboembolism—was comparatively small.
“Using an interprofessional team-based approach to identify and mitigate perioperative risks, for delirium and pneumonia in particular, hospitals may be able to improve key patient outcome measures such as mortality, length of stay and readmissions,” noted an accompanying editorial by Lindee Strizich, M.D., MSc and Christopher S. Kim, M.D.
References
1 Brauer CA, et al. Incidence and mortality of hip fractures in the United States. JAMA. 2009 Oct 14;302:1573–1579.
2 Bhandari M, Swiontkowski M. Management of acute hip fracture. N Engl J Med. 2017 Nov 23;377:2053–2062.
3 Kim SH, et al. Hip fractures in the United States: 2008 nationwide emergency department sample. Arthritis Care Res (Hoboken). 2012;64:751–757.
The study, “The Relative Impact of Specific Postoperative Complications on Older Patients Undergoing Hip Fracture Repair," details the ways in which researchers used data for patients aged 65 years and older from the 2016-2017 Hip Fracture Targeted American College of Surgeons National Surgical Quality Improvement program (ACS NSQIP) to reach their conclusions. Hip fracture in older patients is common, debilitating and costly.1,2,3
Population attributable fractions (PAFs) were used to quantify the anticipated reduction in the primary outcomes (30-day mortality and readmission) that would result from complete prevention of 10 postoperative complications. In 17,755 patients who underwent hip fracture repair in 117 hospitals, postoperative delirium and pneumonia were the highest-impact complications.
Postoperative delirium affected 29.8 percent of patients and was associated with:
- 30-day mortality (11.5 percent)
- Prolonged hospitalization (43 percent)
- 30-day hospital readmission (11.9 percent)
- Pneumonia affected 4.1% of patients and was associated with:
- 30-day mortality (27.3 percent)
- Prolonged hospitalization (66 percent)
- 30-day hospital readmission (28.1 percent)
The impact of the other eight complications – bleeding, Clostridium difficile colitis, decubitus ulcer, myocardial infarction, stroke, surgical site infection, urinary tract infection and venous thromboembolism—was comparatively small.
“Using an interprofessional team-based approach to identify and mitigate perioperative risks, for delirium and pneumonia in particular, hospitals may be able to improve key patient outcome measures such as mortality, length of stay and readmissions,” noted an accompanying editorial by Lindee Strizich, M.D., MSc and Christopher S. Kim, M.D.
References
1 Brauer CA, et al. Incidence and mortality of hip fractures in the United States. JAMA. 2009 Oct 14;302:1573–1579.
2 Bhandari M, Swiontkowski M. Management of acute hip fracture. N Engl J Med. 2017 Nov 23;377:2053–2062.
3 Kim SH, et al. Hip fractures in the United States: 2008 nationwide emergency department sample. Arthritis Care Res (Hoboken). 2012;64:751–757.