Denis Pasero, Product Commercialization Manager, Ilika plc12.09.21
The smart trend that started with cell phones and watches is now spreading to every facet of our lives, including the healthcare field – but what does the term smart really mean?
Electronic components, such as sensors, communications ICs and microcontrollers have been developed that are ultra-small, accurate and use miniscule amounts of energy. Together, these components allow us to take measurements from almost anywhere and transmit the gathered information to datacenters for analysis, processing and storage.
The same principles are used in healthcare with telemedicine, where diagnostic measurements are taken from patients in their homes without the need for them to go to a healthcare facility for testing. Health metrics that can currently be monitored at home include temperature, blood sugar levels and blood pressure, and that list is growing all the time.
The main benefit of telemedicine is its ability to detect any abnormal readings early, allowing the patient to be treated with a better chance of a successful outcome. This early diagnosis also helps to keep costs lower. Another upside of telemedicine is that it allows doctors to be more productive by seeing more patients, a benefit that will only increase in importance as our population ages.
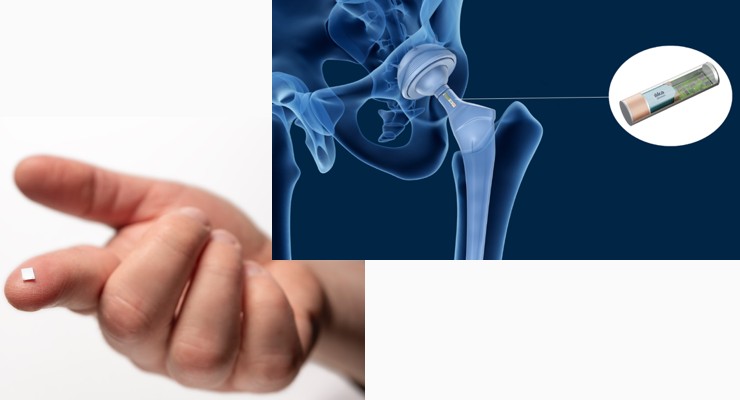
Those benefits can also be gained in orthopedic medicine, with smart sensors embedded in implants rather than in medical devices. There are numerous ways that these smart sensors can be used in orthopedics by measuring metrics such as force, pressure, displacement, and temperature from inside the implant. Knee arthroplasty, hip arthroplasty, spine fusion, and fracture fixation are all applications that will benefit from capturing real-time information on the status of both the implant and the patient, and using that information to reduce complications and quicken recovery times. Fractures can be monitored to ensure that any corrective action can be taken on time, and infections can be detected and treated in their earliest stages. Implants with smart sensors will also be important in helping to improve orthopedic medicine as a whole by providing the information needed to refine implant design, improve surgical techniques or speed up postoperative recovery.
The process of taking in-vivo orthopedic measurements is not new in itself, but the practice hasn’t been able to reach its full potential until now when electronic components have been miniaturized enough to be embedded without affecting the overall form factor of the implant. The basic components required for a smart sensor system include the sensor itself, a microcontroller, and a communications device, along with an antenna, and a power source. It is the power source that has been the last barrier to the widespread integration of smart implants.
To provide the full picture of the ongoing condition of both the implant and the patient requires a circuit that is internally powered. When sensors were first designed into implants, a wired connection was used to provide the power and collect the measured data. This technique used percutaneous leads, which raised the risk of infection and impaired the patient’s mobility. It provided the information required for research purposes, but wasn’t practical outside of the academic setting.
Battery power has also been attempted, but the large physical size of batteries can impact the form factor of the implants and restrict their use for many applications. Additionally, some popular types of battery can also be dangerous. For example, the lithium-ion batteries that power mobile phones can catch fire when stressed. In this case, the battery electrolyte can react with the oxygen found in the battery cathode to create a fire that is self-sustaining. That same electrolyte found in lithium-ion batteries is also toxic, so leakage is another hazard that needs to be overcome.
The ideal power source for smart implants would be small, with a footprint no larger than a few square millimeters and a height of less than a millimeter. It should be safe and long lasting, due to potential complications for the patient during replacement. Finally, it should be easy to recharge and have enough capacity to provide enough energy to power the circuit for a full measure and transmit cycle as often as required.
As they have a solid electrolyte, there is no danger of combustion or leakage, making them safer than other battery designs. Solid-state batteries can be recharged in-vivo by inductive charging or used together with energy harvesting technology to stay operational for almost as long as the implant is viable.
A good example of a modern solid-state battery design is the Ilika Stereax M300, which can be evaluated and designed into new products now and will be generally available from next year. The Stereax M300 is 0.9mm high and currently has a footprint of around 15 mm2. Ilika is currently working on shrinking that footprint to a target size of only 5 mm2. It has a capacity of 300µAh that can be increased by stacking cells together.
The battery can be charged and recharged over a thousand times. That number can be extended to provide an even longer lifetime by over-specifying the energy capacity. If the standard form-factor is not suitable, customizable options can also be arranged.
Together with today’s miniature and power efficient electronic components, solid-state batteries, like the Ilika Stereax M300, are the key to unlocking a new wave of innovation in smart implants that will revolutionize the field of orthopedic medicine.
Denis Pasero is product commercialization manager at Ilika plc, which has developed Stereax mm-scale solid state batteries designed for powering Active Implanted Medical Devices (AIMD).
Electronic components, such as sensors, communications ICs and microcontrollers have been developed that are ultra-small, accurate and use miniscule amounts of energy. Together, these components allow us to take measurements from almost anywhere and transmit the gathered information to datacenters for analysis, processing and storage.
The same principles are used in healthcare with telemedicine, where diagnostic measurements are taken from patients in their homes without the need for them to go to a healthcare facility for testing. Health metrics that can currently be monitored at home include temperature, blood sugar levels and blood pressure, and that list is growing all the time.
The main benefit of telemedicine is its ability to detect any abnormal readings early, allowing the patient to be treated with a better chance of a successful outcome. This early diagnosis also helps to keep costs lower. Another upside of telemedicine is that it allows doctors to be more productive by seeing more patients, a benefit that will only increase in importance as our population ages.
Those benefits can also be gained in orthopedic medicine, with smart sensors embedded in implants rather than in medical devices. There are numerous ways that these smart sensors can be used in orthopedics by measuring metrics such as force, pressure, displacement, and temperature from inside the implant. Knee arthroplasty, hip arthroplasty, spine fusion, and fracture fixation are all applications that will benefit from capturing real-time information on the status of both the implant and the patient, and using that information to reduce complications and quicken recovery times. Fractures can be monitored to ensure that any corrective action can be taken on time, and infections can be detected and treated in their earliest stages. Implants with smart sensors will also be important in helping to improve orthopedic medicine as a whole by providing the information needed to refine implant design, improve surgical techniques or speed up postoperative recovery.
The process of taking in-vivo orthopedic measurements is not new in itself, but the practice hasn’t been able to reach its full potential until now when electronic components have been miniaturized enough to be embedded without affecting the overall form factor of the implant. The basic components required for a smart sensor system include the sensor itself, a microcontroller, and a communications device, along with an antenna, and a power source. It is the power source that has been the last barrier to the widespread integration of smart implants.
Finding an Ideal Source of Power
Almost all electronic systems require their own power source. In some cases devices can be powered wirelessly from an external source. The source sends both the power and the control signals that wake the circuit and instruct it to take a measurement and send the data back. When the source is removed, the circuit powers down until it is activated again. The greatest advantage of this type of circuit is that it can be designed to be safe, small and unobtrusive. The major downside is that it is only useful for capturing important metrics at a single point in time, without providing any visibility of what is happening inside the implant while the circuit is unpowered.To provide the full picture of the ongoing condition of both the implant and the patient requires a circuit that is internally powered. When sensors were first designed into implants, a wired connection was used to provide the power and collect the measured data. This technique used percutaneous leads, which raised the risk of infection and impaired the patient’s mobility. It provided the information required for research purposes, but wasn’t practical outside of the academic setting.
Battery power has also been attempted, but the large physical size of batteries can impact the form factor of the implants and restrict their use for many applications. Additionally, some popular types of battery can also be dangerous. For example, the lithium-ion batteries that power mobile phones can catch fire when stressed. In this case, the battery electrolyte can react with the oxygen found in the battery cathode to create a fire that is self-sustaining. That same electrolyte found in lithium-ion batteries is also toxic, so leakage is another hazard that needs to be overcome.
The ideal power source for smart implants would be small, with a footprint no larger than a few square millimeters and a height of less than a millimeter. It should be safe and long lasting, due to potential complications for the patient during replacement. Finally, it should be easy to recharge and have enough capacity to provide enough energy to power the circuit for a full measure and transmit cycle as often as required.
Solid-State Batteries
A new battery design may be able to provide all of these features. Solid-state batteries are smaller than traditional batteries, while also providing greater power density, more charging cycles and the ability to charge faster.As they have a solid electrolyte, there is no danger of combustion or leakage, making them safer than other battery designs. Solid-state batteries can be recharged in-vivo by inductive charging or used together with energy harvesting technology to stay operational for almost as long as the implant is viable.
A good example of a modern solid-state battery design is the Ilika Stereax M300, which can be evaluated and designed into new products now and will be generally available from next year. The Stereax M300 is 0.9mm high and currently has a footprint of around 15 mm2. Ilika is currently working on shrinking that footprint to a target size of only 5 mm2. It has a capacity of 300µAh that can be increased by stacking cells together.
The battery can be charged and recharged over a thousand times. That number can be extended to provide an even longer lifetime by over-specifying the energy capacity. If the standard form-factor is not suitable, customizable options can also be arranged.
Together with today’s miniature and power efficient electronic components, solid-state batteries, like the Ilika Stereax M300, are the key to unlocking a new wave of innovation in smart implants that will revolutionize the field of orthopedic medicine.
Denis Pasero is product commercialization manager at Ilika plc, which has developed Stereax mm-scale solid state batteries designed for powering Active Implanted Medical Devices (AIMD).