Maria Shepherd, President and Founder, Medi-Vantage03.21.18
What a difference eight years makes. The massive changes in economic, regulatory, and consumer mandates have altered healthcare delivery across the United States. Compare 2018 to 2010. While we still haven’t seen an aggregate reduction in healthcare costs, increased efficiency and demonstrated value are evident in many successful hospital systems.
Why This Is Important
In 2017, there were 5,564 registered hospitals in the United States, according to the American Hospital Association.1 More than 85 percent (4,892) of these hospitals were community institutions and 2,845 of those were nonprofit, 1,034 were for-profit, and 983 were owned by state or local government systems (Table 1). In 2017, almost 400 U.S. hospitals2 were linked with 151 accredited medical schools in the country, according to data from the Association of American Medical Colleges.
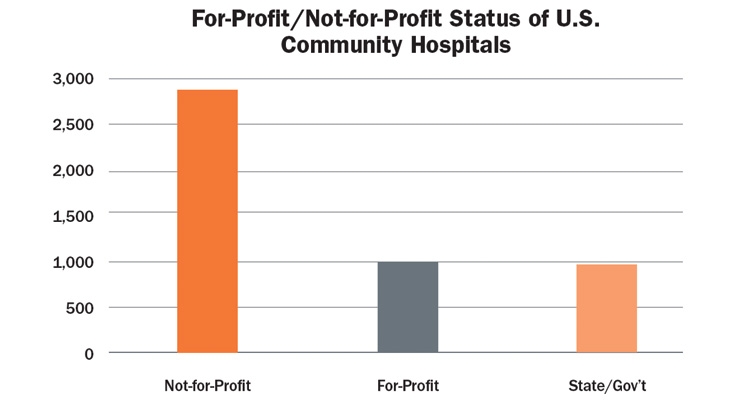
Table 1
For-profit vs. not-for-profit status is important because, while the overall cost of U.S. healthcare is increasing, services are decreasing. Total inpatient hospital beds fell to 17.3 beds per 1,000 people in 2014 from 32.8 beds in 1990, a reduction of 47 percent.3 Hospital length of stay decreased from an average nine days in 1990 to five days in 2014, a decrease of 44 percent. The 2014 average cost per inpatient day was $2,346 for nonprofit hospitals and $1,798 for for-profit hospitals, a significant difference of $548 per day (Table 2).
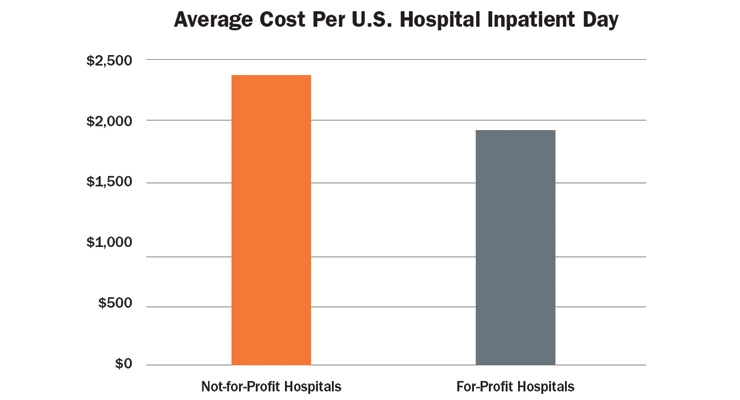
Table 2
According to a survey conducted by the American Academy of Orthopaedic Surgeons (AAOS), one way that for-profit hospitals can reduce cost is by employing orthopedic surgeons.4 Employing the orthopedic surgeon generates an average annual revenue of approximately $3 million per surgeon through the inpatient and outpatient care of patients, facilities fees, and ancillary services.
A 2015 AAOS survey4 states that 20 percent of the 28,047 orthopedic surgeon members of the AAOS are full-time employees of a hospital, academic center, or HMO. More than 60 percent participate in private practice, either in single or multi-specialty groups, or in small one to two physician practices. The remaining 20 percent work mostly in a mix of the two or for industry, insurance, or hospital administration.
Employment status makes a huge difference in the orthopedic surgeon’s income (Table 3), and those making the highest salaries in private practice will have different incentives than those employed by hospitals.
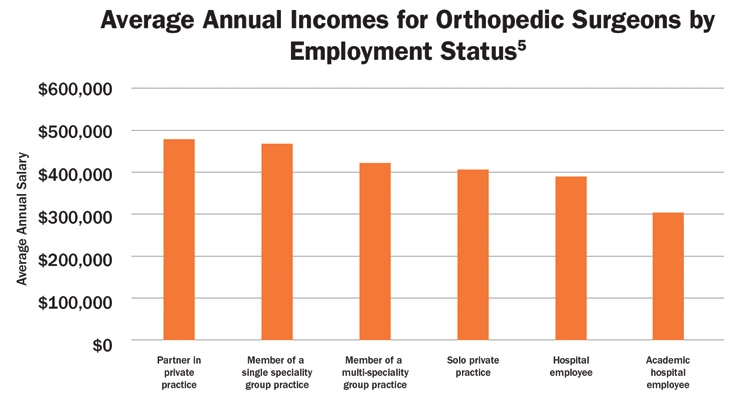
Table 3
The Medi-Vantage Perspective
While we will never leave the surgeon out of our research, as they are highly valuable decision makers, more than 50 percent of any given strategy research we perform investigates hospital administration opinions on the cost of doing business with medical device companies.
Our findings? For surgeons, understand the different and ever-changing incentives that are driven by employment status. For hospital administrators, develop medical devices that help reduce the length of stay. In our research, we learned that there is high value to a hospital CEO in getting a bed back one day early.
What Should Your Company Be Doing?
If your device helps reduce length of stay, develop a value proposition that proves the reduction in cost that feature/benefit provides. It moves your company away from negotiating on price, which can spiral out of control quickly.
References
Maria Shepherd has more than 20 years of leadership experience in medical device/life-science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing and business strategy as well as innovation research for the medical device industry. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.msbiv.com). She can be reached at 855-343-3100, ext. 102, or at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.
Why This Is Important
In 2017, there were 5,564 registered hospitals in the United States, according to the American Hospital Association.1 More than 85 percent (4,892) of these hospitals were community institutions and 2,845 of those were nonprofit, 1,034 were for-profit, and 983 were owned by state or local government systems (Table 1). In 2017, almost 400 U.S. hospitals2 were linked with 151 accredited medical schools in the country, according to data from the Association of American Medical Colleges.

Table 1
For-profit vs. not-for-profit status is important because, while the overall cost of U.S. healthcare is increasing, services are decreasing. Total inpatient hospital beds fell to 17.3 beds per 1,000 people in 2014 from 32.8 beds in 1990, a reduction of 47 percent.3 Hospital length of stay decreased from an average nine days in 1990 to five days in 2014, a decrease of 44 percent. The 2014 average cost per inpatient day was $2,346 for nonprofit hospitals and $1,798 for for-profit hospitals, a significant difference of $548 per day (Table 2).

Table 2
According to a survey conducted by the American Academy of Orthopaedic Surgeons (AAOS), one way that for-profit hospitals can reduce cost is by employing orthopedic surgeons.4 Employing the orthopedic surgeon generates an average annual revenue of approximately $3 million per surgeon through the inpatient and outpatient care of patients, facilities fees, and ancillary services.
A 2015 AAOS survey4 states that 20 percent of the 28,047 orthopedic surgeon members of the AAOS are full-time employees of a hospital, academic center, or HMO. More than 60 percent participate in private practice, either in single or multi-specialty groups, or in small one to two physician practices. The remaining 20 percent work mostly in a mix of the two or for industry, insurance, or hospital administration.
Employment status makes a huge difference in the orthopedic surgeon’s income (Table 3), and those making the highest salaries in private practice will have different incentives than those employed by hospitals.

Table 3
The Medi-Vantage Perspective
While we will never leave the surgeon out of our research, as they are highly valuable decision makers, more than 50 percent of any given strategy research we perform investigates hospital administration opinions on the cost of doing business with medical device companies.
Our findings? For surgeons, understand the different and ever-changing incentives that are driven by employment status. For hospital administrators, develop medical devices that help reduce the length of stay. In our research, we learned that there is high value to a hospital CEO in getting a bed back one day early.
What Should Your Company Be Doing?
If your device helps reduce length of stay, develop a value proposition that proves the reduction in cost that feature/benefit provides. It moves your company away from negotiating on price, which can spiral out of control quickly.
References
- http://bit.ly/odt180401
- http://bit.ly/odt180402
- http://bit.ly/odt180403 [PDF]
- Orthopaedic Practice in the U.S. 2014, American Academy of Orthopaedic Surgeons.
- http://bit.ly/odt180404
Maria Shepherd has more than 20 years of leadership experience in medical device/life-science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing and business strategy as well as innovation research for the medical device industry. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.msbiv.com). She can be reached at 855-343-3100, ext. 102, or at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.