Ilsa Webeck, Managing Director & Founder, MedTech Strategies03.19.24
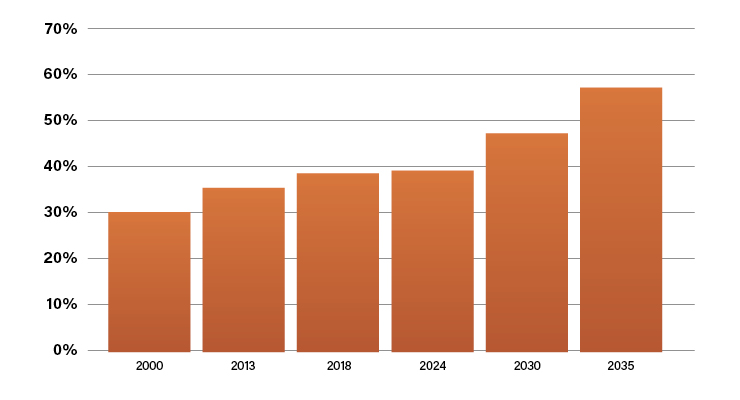
In the U.S., obesity continues to be a major issue for the healthcare industry and the well-being of a significant portion of the population. In 2022, self-reported surveys demonstrated three states (West Virginia, Louisiana, and Oklahoma) had over 40% of their total adult population classified as obese and half of U.S. states had over 40% of non-Hispanic black adult population self-reporting as obese.1
Not only was obesity a concern before the COVID pandemic, but research has demonstrated the rate of obesity among both children2 and adults3 has increased since. Relative to 2019, there was a significantly higher average body mass index (+0.6%) and rates of obesity (+0.3%) for adults through the pandemic (Table 1).
While these year-to-year percent changes may seem small, the connection between the increase in weight is correlated to an increase in annual medical costs. Obesity can add $1,861 to yearly healthcare costs while severe obesity can add up to $3,097, which adds additional strain to an already stretched U.S. healthcare system5—already at an estimated $100 billion annual cost of treating obesity.6
Arthroplasty surgery for obese patients with hip osteoarthritis can cause a variety of acute complications and worrisome side effects. A clinical team from the Hospital of Cook County in Chicago, Ill., and St. George's University in Granada, researched the differences in hip replacement morbidity and mortality following surgery. While the obese patients did not show a higher risk for in-hospital mortality, they needed a longer length of stay and were more likely to develop deep vein thrombosis, acute kidney failure, and pressure-related injuries compared to non-obese patients.8 However, the literature suggests while obesity has risks associated with the success of the surgical procedure itself, six months post-op, severely and morbidly obese patients reported pain relief and functional gain equivalent to other patients.9
For knee replacements, there has been mixed data on the impact of obesity and the likelihood of success and potential for future revision needs. A review article published in 2022 was unable to show significant differences between morbidity associated with knee arthroplasty, stating, “We consider the gained benefit for the morbidly obese in functional outcome to surpass the risk in TKA [total knee arthroplasty].”10
For both groups, the added surgical complications associated with obesity are present, but the benefits of knee or hip arthroplasty in obese populations outweigh the risks.
While the prevalence of obesity in the U.S. remains a significant concern, it will be interesting to watch the overall impact of the pandemic and new pharmacotherapies for obesity. The long-term impact of these factors on obesity rates and subsequent joint replacement remains uncertain, prompting questions about the future of hip and knee arthroplasty procedures, growth for device companies, and the overall health outcomes of the population.
References
Ilsa Webeck has over 25 years of work experience assessing commercial and market viability in the medtech space. After founding MedTech Strategies in 2014, she has worked with a wide range of organizations focused on assessing commercial fit and identifying product and service value propositions, as well as uncovering customer/user needs to understand a path to commercial success. Her past experiences include group product director at J&J’s DePuy Spine, leading the strategic marketing and upstream marketing team, and associate director for global commercial strategy in the MS Franchise at Biogen Idec. For more information, visit www.medtechstrategiesllc.com.
Not only was obesity a concern before the COVID pandemic, but research has demonstrated the rate of obesity among both children2 and adults3 has increased since. Relative to 2019, there was a significantly higher average body mass index (+0.6%) and rates of obesity (+0.3%) for adults through the pandemic (Table 1).
While these year-to-year percent changes may seem small, the connection between the increase in weight is correlated to an increase in annual medical costs. Obesity can add $1,861 to yearly healthcare costs while severe obesity can add up to $3,097, which adds additional strain to an already stretched U.S. healthcare system5—already at an estimated $100 billion annual cost of treating obesity.6
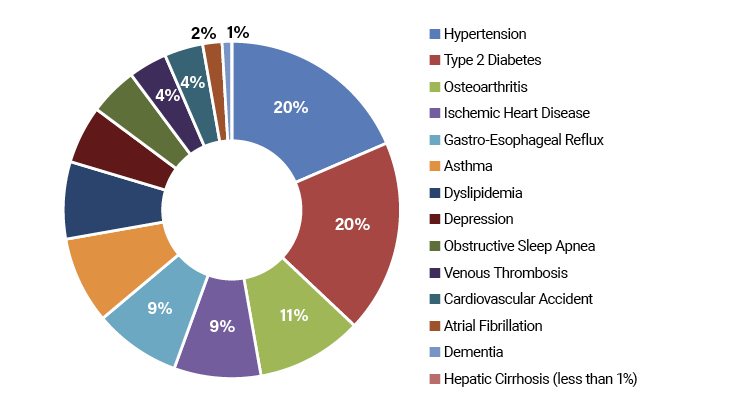
Obesity Comorbidities
One study completed by the Royal College in the U.K. provides a stark look at the comorbidities associated with obesity (Table 2) and the risks and impacts that are only growing.7 Osteoarthritis appears as the third most common comorbidity for patients with obesity at 11% after hypertension (20%) and Type 2 diabetes (20%), which often have concomitant conditions. As a top comorbidity associated with obesity, osteoarthritis is a concerning issue and will continue to be so as the population grows increasingly obese.Arthroplasty surgery for obese patients with hip osteoarthritis can cause a variety of acute complications and worrisome side effects. A clinical team from the Hospital of Cook County in Chicago, Ill., and St. George's University in Granada, researched the differences in hip replacement morbidity and mortality following surgery. While the obese patients did not show a higher risk for in-hospital mortality, they needed a longer length of stay and were more likely to develop deep vein thrombosis, acute kidney failure, and pressure-related injuries compared to non-obese patients.8 However, the literature suggests while obesity has risks associated with the success of the surgical procedure itself, six months post-op, severely and morbidly obese patients reported pain relief and functional gain equivalent to other patients.9
For knee replacements, there has been mixed data on the impact of obesity and the likelihood of success and potential for future revision needs. A review article published in 2022 was unable to show significant differences between morbidity associated with knee arthroplasty, stating, “We consider the gained benefit for the morbidly obese in functional outcome to surpass the risk in TKA [total knee arthroplasty].”10
For both groups, the added surgical complications associated with obesity are present, but the benefits of knee or hip arthroplasty in obese populations outweigh the risks.
Pharmacotherapies for Obesity
The recent launch of “obesity drugs” calls the future rate of obesity growth rates into question and, therefore, may have a significant impact on the rate of osteoarthritis and joint replacement. According to a recent publication, the seven drug options currently available are having an impact. Patients are experiencing benefits from using these drugs, with reported 5%-10% total body weight loss.11 It will be interesting to watch the dynamics to see if the prevalence of these new obesity treatments will have any impact on the prevalence of osteoarthritis or knee pain and, therefore, shift the number of surgeries.Future Impact
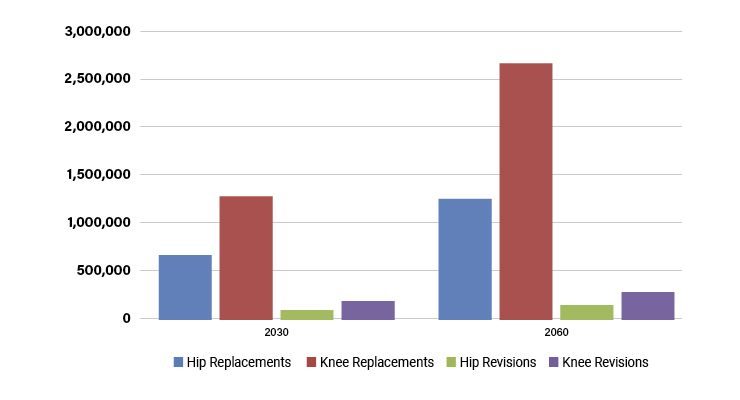
What does this mean for the hip and knee arthroplasty industry (Table 3)? An increase in obesity is leading to an increase of osteoarthritis, however, new obesity drugs will have an uncertain impact. Moreover, Stryker Chairman, CEO, and President Kevin Lobo stated, “We are, in fact, optimistic about the positive impacts of these drugs...In the short term, it will help to make ineligible people eligible for surgery sooner. And in the long term, it will likely lead to more surgery as people increase their activity levels. With that said, the rate and persistence of adoption of these medicines is still a large unknown...”13While the prevalence of obesity in the U.S. remains a significant concern, it will be interesting to watch the overall impact of the pandemic and new pharmacotherapies for obesity. The long-term impact of these factors on obesity rates and subsequent joint replacement remains uncertain, prompting questions about the future of hip and knee arthroplasty procedures, growth for device companies, and the overall health outcomes of the population.
The MedTech Strategies Perspective
The increase in obesity following COVID has had a significant impact on the health of the U.S. population, however, the introduction and more widespread use of pharmacologic treatments may have a significant impact on hip and knee arthroplasty needs in the next five to 10 years. Will these factors balance out, leading to continued growth in the need for total joint replacement or will the drug options lead to a healthier, pain-free population?References
- bit.ly/3uSGiia
- bit.ly/3uKNuNt
- bit.ly/3Tibl07
- bit.ly/3UZU90X
- bit.ly/3UYAYo0
- bit.ly/3UVA37W
- bit.ly/49RXqn2
- bit.ly/48EuBJV
- bit.ly/3ViE8n1
- bit.ly/49zZ4Kf
- bit.ly/49xvYLv
- bit.ly/49SuJpX
- Stryker earnings call (Q3 2023)
Ilsa Webeck has over 25 years of work experience assessing commercial and market viability in the medtech space. After founding MedTech Strategies in 2014, she has worked with a wide range of organizations focused on assessing commercial fit and identifying product and service value propositions, as well as uncovering customer/user needs to understand a path to commercial success. Her past experiences include group product director at J&J’s DePuy Spine, leading the strategic marketing and upstream marketing team, and associate director for global commercial strategy in the MS Franchise at Biogen Idec. For more information, visit www.medtechstrategiesllc.com.