Personalized healthcare has garnered significant attention for years and it’s only continued to increase. While the benefits of serving each patient with the solutions to address their unique needs are numerous, costs and manufacturing challenges have limited implementation. One area, however, in which personalized healthcare has gained substantial ground is within the orthopedic space. A number of contributing factors have allowed for this healthcare sector to take a lead position in offering personalized healthcare.
One of the tools that help to enable personalized healthcare is additive manufacturing. With costs falling for the machines as well as the materials, more companies are able to offer the service. Further, healthcare facilities are even exploring additive manufacturing technologies to bring the benefits into the clinical space.
Offering his perspective on the drivers, benefits, and trends around personalized healthcare and additive manufacturing, Benjamin Johnson, vice president of Portfolio & Regulatory at 3D Systems, took time to respond to a number of questions around these topics. In the following Q&A, Johnson discusses why personalized healthcare is a critical step in delivering care and provides feedback how additive manufacturing is helping to make it a reality.
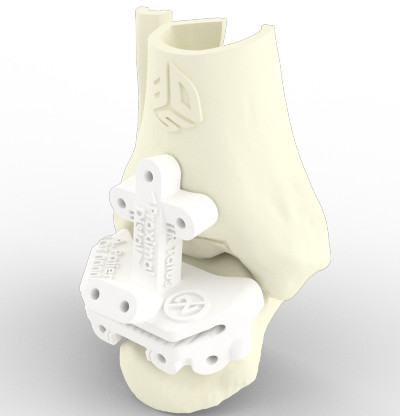
Vantage® Ankle PSI provides pre-operative planning, surgical guides, and anatomic models for TAA procedures.
Benjamin Johnson: Personalized patient care for improving surgical outcomes isn’t a new concept, but the adoption of patient-specific technologies is rapidly accelerating due to several factors. First, the availability and quality of patient diagnostic data has dramatically improved over the last few decades. The computing power needed to acquire, transfer, visualize, and manipulate large amounts of high-resolution data is accessible at reasonable cost. Second, the technologies needed to fabricate patient-specific instruments and implants are stabilizing, which allows for low-volume batch manufacturing at scale. Finally, regulatory pathways for personalized devices have been established with a significant number of patient-specific products currently on the market.
Fenske: Doesn’t the challenge of this level of personalization outweigh the potential benefits?
Johnson: The answer essentially boils down to a cost-benefit analysis per procedure type. It is certainly worthwhile to invest in pre-surgical planning patient-specific device design for complex surgical interventions with a high risk of reintervention or where patient aesthetics and quality of life are heavily impacted. As the costs and lead times associated with device personalization decrease through technological improvements, more procedures will become accessible.
Fenske: How are regulatory issues addressed when we are talking about one product for one patient?
Johnson: The regulatory frameworks for patient-specific devices continue to evolve, but there is a lot of work being put into creating robust guidelines. In terms of quality systems, the manufacturing workflow is still very labor intensive. Therefore, a lot of in-process checks typically need to be established to ensure reliability. This also includes having the clinical team involved in the process to direct and review the preferred treatment plan.
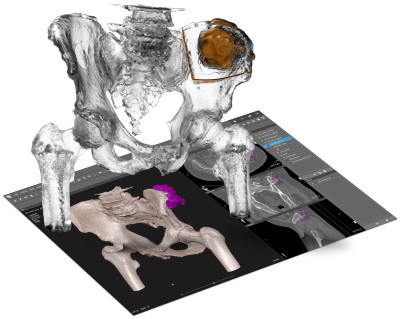
3D Systems’ D2P® software enables creation of patient-specific digital and physical 3D anatomic models for pre-surgical planning.
Johnson: The concept of additive manufacturing, or to build devices layer by layer, is perfectly suited for patient-specific instruments and implants versus traditional manufacturing techniques that require machine set up or tooling. It’s just as reasonable to fabricate a single device for a patient as it is to manufacture a batch of parts from a single build. Further, the materials available to additive manufacturing are well suited for a myriad of patient specific devices from conformable skin-contacting devices to single-use disposable instruments to permanent implants.
Fenske: Through additive manufacturing, will we see personalized healthcare solutions made available at the point of care (i.e., within the hospital environment)?
Johnson: We are already seeing deployment of additive manufacturing technologies for clinical care at most major medical centers. Today, the devices being produced are typically lower risk tools used for medical communication and treatment planning. However, the benefits to surgical outcome, total healthcare cost, and patient satisfaction will drive change to how and where patient-specific solutions are manufactured. The point-of-care medical device manufacturing center will become an essential part of every hospital in the not-too-distant future.
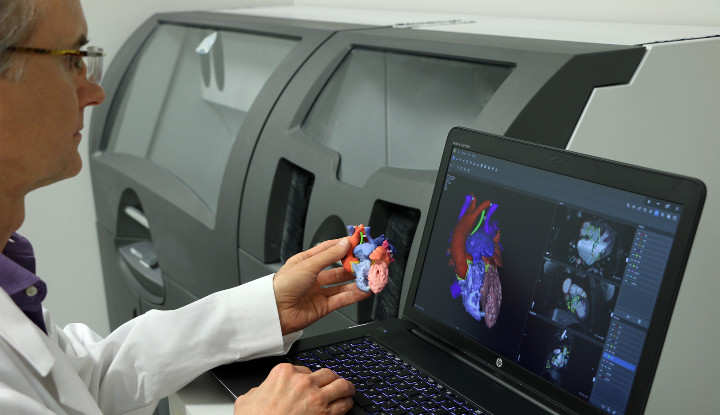
The point-of-care medical device manufacturing center will become an essential part of every hospital in the not-too-distant future.
Fenske: What about cost considerations with personalized healthcare? Do you anticipate a significant increase in the cost of these solutions versus how they are offered currently?
Johnson: The way to think about patient-specific solutions, in my opinion, is a tradeoff between the cost of the devices and the benefits realized in the form of decreased morbidities, readmissions, and revisions. In parallel, I suspect the cost of the devices will come down as new technologies addressing the workflow are deployed.
Fenske: Do you have any additional comments you’d like to share based on any of the topics we discussed or something you’d like to tell orthopedic device manufacturers?
Johnson: Bringing patient-specific medical devices to market is an arduous endeavor. Partnering with a team that has experience helping manufacturers navigate the process—from concept and design to clearance and manufacturing—can accelerate innovation. 3D Systems’ Application Innovation Group provides consulting services that range from medical device design and development to process qualification of printers for device manufacturing and continued production support.
Find out more about 3D Systems’ Application Innovation Group>>>>>