Business Wire10.09.17
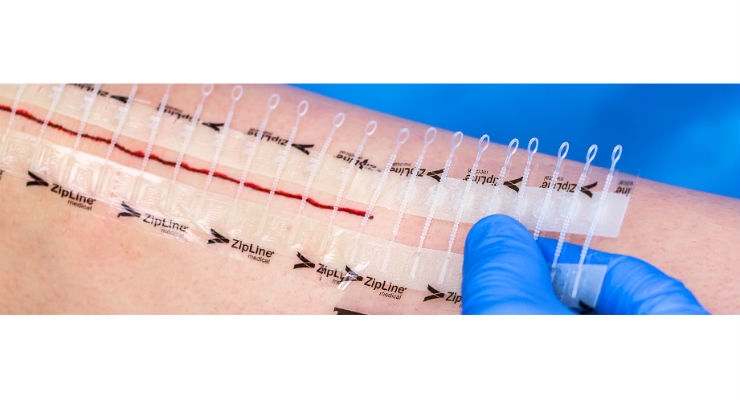
ZipLine Medical Inc. has announced results from an economic study that showed that Zip Surgical Skin Closure reduced post-discharge costs for total knee arthroplasty (TKA) when compared to staples. Results were presented at a Knee Society Members Meeting by Roger Emerson, M.D., of the Texas Center for Joint Replacement in Plano, Texas.
“In the study, we saw that staples and the Zip are both fast to apply in the operating room, but in the post-discharge environment, staple-related issues, such as patient phone calls, emergency department visits, infection concerns and removal create extra work and extra cost in the long run,” said Emerson. “In addition, patients were apprehensive about staple removal and concerned when they saw redness around their staples, which in some cases triggered antibiotic prescriptions to avoid possible infection.”
The study encompassed 130 consecutive TKA patients, with half of subjects closed with staples and half closed with Zip Surgical Skin Closure. All surgeries were performed at the Texas Center for Joint Replacement by the same surgeon using the same approach and implant, and were closed by the same surgical physician’s assistant. Patients were followed from surgery to first clinic post-operative visit (day 21-28) for assessment.
The study findings showed that the Zip reduced all of the following measures when compared to staples:
”In addition to actual emergency room, clinic and wound-related care costs, which can be considered ‘bundle-busters’ in a bundled care setting, there are opportunity costs to consider, where unreimbursed time responding to patient calls, concerns and staple removal results in less time spent on billable activities,” said Omar Alnachoukati, director of clinical research at the Texas Center for Joint Replacement. “In the study, we found a five times higher opportunity cost in the staple group. Total joint arthroplasty is the largest expense for a single condition among Medicare beneficiaries, totaling $7 billion annually. With staples currently one of the primary methods currently used for TKA closure, this study suggests that replacing staples with the non-invasive Zip device has the potential to offer significant savings to the healthcare system.”
The Zip is a non-invasive skin closure device that replaces sutures, staples, and glue for surgical incisions and lacerations. Clinical studies have demonstrated significant time savings, fewer wound complications and the ability to reduce post discharge healthcare costs. A patented force distribution design results in secure wound closure, excellent scar quality and high patient satisfaction. Unlike staples or sutures, there are no skin punctures with the Zip that can create pathways for bacteria. Benefits of the Zip have been demonstrated in clinical studies in orthopedic total joint arthroplasty, foot and ankle, pediatric cardiothoracic, electrophysiology, dermatology, and plastic and reconstructive surgery. Zip Surgical Skin Closure devices are classified by the U.S. Food and Drug Administration as Class I, 510(k) Exempt, and have received the CE Mark and China Food and Drug Administration approval.
ZipLine Medical develops cost-effective, non-invasive surgical skin closure devices that deliver high patient satisfaction and surgeon efficiency. Zip Surgical Skin Closure devices have been used in more than 100,000 cases and in over 30 countries worldwide. ZipLine Medical was founded by Amir Belson, M.D. and is headquartered in Campbell, Calif.
“In the study, we saw that staples and the Zip are both fast to apply in the operating room, but in the post-discharge environment, staple-related issues, such as patient phone calls, emergency department visits, infection concerns and removal create extra work and extra cost in the long run,” said Emerson. “In addition, patients were apprehensive about staple removal and concerned when they saw redness around their staples, which in some cases triggered antibiotic prescriptions to avoid possible infection.”
The study encompassed 130 consecutive TKA patients, with half of subjects closed with staples and half closed with Zip Surgical Skin Closure. All surgeries were performed at the Texas Center for Joint Replacement by the same surgeon using the same approach and implant, and were closed by the same surgical physician’s assistant. Patients were followed from surgery to first clinic post-operative visit (day 21-28) for assessment.
The study findings showed that the Zip reduced all of the following measures when compared to staples:
- A 46 percent reduction in incision-related actual clinic costs
- A 60 percent reduction in incision-related phone calls
- A 60 percent reduction in incision-related clinic visits
- A 75 percent reduction in incision-related antibiotics prescribed
”In addition to actual emergency room, clinic and wound-related care costs, which can be considered ‘bundle-busters’ in a bundled care setting, there are opportunity costs to consider, where unreimbursed time responding to patient calls, concerns and staple removal results in less time spent on billable activities,” said Omar Alnachoukati, director of clinical research at the Texas Center for Joint Replacement. “In the study, we found a five times higher opportunity cost in the staple group. Total joint arthroplasty is the largest expense for a single condition among Medicare beneficiaries, totaling $7 billion annually. With staples currently one of the primary methods currently used for TKA closure, this study suggests that replacing staples with the non-invasive Zip device has the potential to offer significant savings to the healthcare system.”
The Zip is a non-invasive skin closure device that replaces sutures, staples, and glue for surgical incisions and lacerations. Clinical studies have demonstrated significant time savings, fewer wound complications and the ability to reduce post discharge healthcare costs. A patented force distribution design results in secure wound closure, excellent scar quality and high patient satisfaction. Unlike staples or sutures, there are no skin punctures with the Zip that can create pathways for bacteria. Benefits of the Zip have been demonstrated in clinical studies in orthopedic total joint arthroplasty, foot and ankle, pediatric cardiothoracic, electrophysiology, dermatology, and plastic and reconstructive surgery. Zip Surgical Skin Closure devices are classified by the U.S. Food and Drug Administration as Class I, 510(k) Exempt, and have received the CE Mark and China Food and Drug Administration approval.
ZipLine Medical develops cost-effective, non-invasive surgical skin closure devices that deliver high patient satisfaction and surgeon efficiency. Zip Surgical Skin Closure devices have been used in more than 100,000 cases and in over 30 countries worldwide. ZipLine Medical was founded by Amir Belson, M.D. and is headquartered in Campbell, Calif.