Maria Shepherd, President and Founder, Medi-Vantage05.29.18
The practice of orthopedic surgery is still going through a significant transformation. Practice shifts from private to hospital employees and back to private again. This level of turbulence creates ambiguity, questions, threats, and opportunities.
Why This Is Important
Hospital employment of orthopedic surgeons has surged and decreased over the past 10 years. The trend of increasing hospital employment of orthopedic physicians has been driven by the U.S. healthcare environment and reimbursement shifts. Practice dynamics are changing (and disconcerting) for orthopedic surgeons. According to the AAOS,1 in 2016, an estimated 35 percent of orthopedists worked in private practice groups. Following that, 17 percent are salaried employees in hospitals, while 15 percent are employees of an academic institution. Rounding out the total, 11 percent work in solo private practice, and 9 percent work in multi-specialty groups (Table 1).

Table 1: 2016 Employment Statistics for Orthopedic Surgeons1
In 2010, of the approximately 5,000 or more accredited hospitals providing a full spectrum of surgical services, almost 500 had initiated true orthopedic hospital employment programs.2 It is difficult to assess that number now, in 2018, but our research here at Medi-Vantage indicates a significant percentage of orthopedic surgeons have gone back to private practice after working as a hospital employee.
This is supported by advice given in a Healio article.3 In that article, Nicholas A. Sgaglione, M.D., stated that strong leadership and good incentives drive long-term hospital employee tenure for orthopedic surgeons. He said, “Three keys to departmental retention in a hospital setting are regular communication with physicians, consensus, and coordination. Probably the largest area of dissatisfaction we find for those who have joined hospital systems from the private practice world, where you can manage whether you want to…hire another secretary or have another assistant, is that you are told, well, you cannot have a PA [physician assistant] or you cannot have that extra assistant that you need.”
Higher incomes are one reason hospital-employed surgeons return to private practice (Table 2). Yet, according to a Medscape survey, despite their high incomes relative to other medical specialties, only 48 percent of all orthopedic surgeons feel they are fairly compensated.4
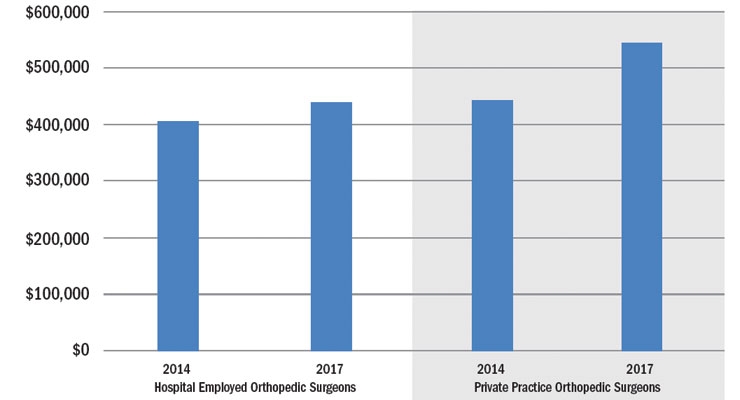
Table 2: Private Practice Orthopedic Surgeons Still the Highest Paid4
This is probably one important factor leading to the finding that the 2017 number of orthopedic surgeons working in ACOs4 has remained constant with those numbers reported in 2014 in the Market Snapshot column titled, “Big Changes in Orthopedic Practices” (Table 3).
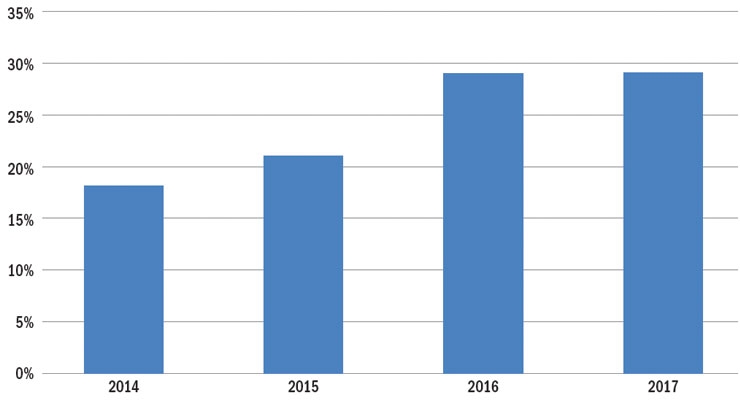
Table 3: Estimated Percentage of Orthopedic Surgeons Working in ACOs4
The Medscape survey4 validates our research interviews with orthopedic surgeons. Many tell us they are proud of the work that they do, but are frustrated with the constraints of employment in hospitals. Orthopedic surgeons find their relationships with their patients a highly rewarding aspect of their practices and their professional expertise in orthopedic surgery balances the many challenges they face (long hours, policies and regulations, low reimbursement from CMS, and the often-unfathomable complexities of the electronic medical record system).
What Can You Do as a Supplier of Orthopedic Products?
Clearly, our physician customers are stressed out. However, good medical device product design can reduce their stress, if designed and tested to do so. In a study5 designed to non-invasively measure perceived and biologically expressed stress levels of surgeons using two different types of hernia repairs performed in an animal model, conclusive evidence of reduced perceived stress levels was a finding for one of the designs.
Perceived stress was measured using a questionnaire that scored perceived stress levels in terms of mental, physical, and temporal demands; situational stress; task complexity; and distractions. To achieve an objective measurement, salivary hormone levels using the biomarkers amylase and cortisol were taken at multiple times before, during, and after the procedure. Objective assessments of decreased surgical stress have been linked to reduced surgical errors and improved outcomes.6 Is your product designed to reduce surgeon stress? It all starts with the marketing specification—does your message call out the need to reduce surgeon stress in an effort to improve outcomes?
References
Maria Shepherd has more than 20 years of leadership experience in medical device/life-science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing and business strategy as well as innovation research for the medical device industry. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.msbiv.com). She can be reached at 855-343-3100, ext. 102, or at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.
Why This Is Important
Hospital employment of orthopedic surgeons has surged and decreased over the past 10 years. The trend of increasing hospital employment of orthopedic physicians has been driven by the U.S. healthcare environment and reimbursement shifts. Practice dynamics are changing (and disconcerting) for orthopedic surgeons. According to the AAOS,1 in 2016, an estimated 35 percent of orthopedists worked in private practice groups. Following that, 17 percent are salaried employees in hospitals, while 15 percent are employees of an academic institution. Rounding out the total, 11 percent work in solo private practice, and 9 percent work in multi-specialty groups (Table 1).

Table 1: 2016 Employment Statistics for Orthopedic Surgeons1
In 2010, of the approximately 5,000 or more accredited hospitals providing a full spectrum of surgical services, almost 500 had initiated true orthopedic hospital employment programs.2 It is difficult to assess that number now, in 2018, but our research here at Medi-Vantage indicates a significant percentage of orthopedic surgeons have gone back to private practice after working as a hospital employee.
This is supported by advice given in a Healio article.3 In that article, Nicholas A. Sgaglione, M.D., stated that strong leadership and good incentives drive long-term hospital employee tenure for orthopedic surgeons. He said, “Three keys to departmental retention in a hospital setting are regular communication with physicians, consensus, and coordination. Probably the largest area of dissatisfaction we find for those who have joined hospital systems from the private practice world, where you can manage whether you want to…hire another secretary or have another assistant, is that you are told, well, you cannot have a PA [physician assistant] or you cannot have that extra assistant that you need.”
Higher incomes are one reason hospital-employed surgeons return to private practice (Table 2). Yet, according to a Medscape survey, despite their high incomes relative to other medical specialties, only 48 percent of all orthopedic surgeons feel they are fairly compensated.4

Table 2: Private Practice Orthopedic Surgeons Still the Highest Paid4
This is probably one important factor leading to the finding that the 2017 number of orthopedic surgeons working in ACOs4 has remained constant with those numbers reported in 2014 in the Market Snapshot column titled, “Big Changes in Orthopedic Practices” (Table 3).

Table 3: Estimated Percentage of Orthopedic Surgeons Working in ACOs4
The Medscape survey4 validates our research interviews with orthopedic surgeons. Many tell us they are proud of the work that they do, but are frustrated with the constraints of employment in hospitals. Orthopedic surgeons find their relationships with their patients a highly rewarding aspect of their practices and their professional expertise in orthopedic surgery balances the many challenges they face (long hours, policies and regulations, low reimbursement from CMS, and the often-unfathomable complexities of the electronic medical record system).
What Can You Do as a Supplier of Orthopedic Products?
Clearly, our physician customers are stressed out. However, good medical device product design can reduce their stress, if designed and tested to do so. In a study5 designed to non-invasively measure perceived and biologically expressed stress levels of surgeons using two different types of hernia repairs performed in an animal model, conclusive evidence of reduced perceived stress levels was a finding for one of the designs.
Perceived stress was measured using a questionnaire that scored perceived stress levels in terms of mental, physical, and temporal demands; situational stress; task complexity; and distractions. To achieve an objective measurement, salivary hormone levels using the biomarkers amylase and cortisol were taken at multiple times before, during, and after the procedure. Objective assessments of decreased surgical stress have been linked to reduced surgical errors and improved outcomes.6 Is your product designed to reduce surgeon stress? It all starts with the marketing specification—does your message call out the need to reduce surgeon stress in an effort to improve outcomes?
References
- Orthopaedic Practice in the U.S. 2016, AAOS
- http://bit.ly/odt180603 [PDF]
- http://bit.ly/odt180601
- http://bit.ly/odt180602
- http://bit.ly/odt180604
- C.M. Wetzel, et al. The American Journal of Surgery 191 (2006) 5–10
Maria Shepherd has more than 20 years of leadership experience in medical device/life-science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing and business strategy as well as innovation research for the medical device industry. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.msbiv.com). She can be reached at 855-343-3100, ext. 102, or at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.