Sam Brusco, Associate Editor02.17.23
In late January, the Advanced Medical Technology Association (AdvaMed) presented industry concerns regarding new ethylene oxide (EtO) regulations with President Joe Biden. The association expressed that sterilization facility closures could cause critical medical device shortages.
In a letter to the President,¹ AdvaMed president and CEO Scott Whitaker stated that the medtech industry welcomes the updated regulations for EtO sterilization facilities but asks that even though the Environmental Protection Agency (EPA) hasn’t threatened to ban EtO sterilization, the agency should “carefully reconsider language that might unreasonably alarm residents near sterilization facilities.”
Whitaker outlines his and the industry’s concern further in the letter: “We would ask that you consider the potential threat to patient care if any sterilization facilities shut down. With 20 billion medical devices sterilized using EtO each year in the U.S. at about only 100 facilities, the closure of even a small percentage of facilities could harm patient access to health care. EtO sterilization is at capacity. With 80 percent of surgical kits alone sterilized using EtO, any shutdown-induced disruption could reverberate from screening to the operating room to post-operative care.”
Whitaker said this concern came to fruition when a prior facility closure brought about the temporary shortage of pediatric breathing tubes, according to the U.S. Food and Drug Administration (FDA), and that the federal agency also expressed concerns about medical device availability should more facilities close.
He called on the EPA to “embrace technology-neutral solutions to meet new emissions targets” as well as “consider background EtO levels in ambient air and the tiny proportion of that represented by medical device sterilization EtO use.” Whitaker concluded by reiterating that the medtech industry and FDA are working to explore alternative sterilization methods.
In order to gain more insight on the EtO discourse and other prevalent trends, market forces, and challenges affecting medical/orthopedic device packaging and sterilization, ODT spoke to several experts in the space:
Marco Bianchi: As a manufacturer of sterilizers, we see from the perspective of long-time and well-known technologies, such as gamma ray and EtO sterilization. From the other side, there is a great push from authorities and producers for a greener, more sustainable technology, and we are deeply involved in making the world aware of our new HyPerPure technology, a solution for these topics.
Don Kennedy: First, rising costs associated with terminal sterilization of devices and transportation of surgery sets; and second, price reduction practices enacted in good conscience by payors that end up preventing adoption of more efficient products or services that can be proven and demonstrated to lower operating costs. Another way to express this is cutting costs but not actually reducing them due to inefficient practices.
An example of the latter is the cost of hot water at healthcare facilities. It’s a lesson I learned from an ASC owner who asked what I thought the most expensive cost was at his facility. I answered “people,” but he told me it was the energy bill he paid to run the steam autoclaves, and if he could have all his implants provided terminally sterile (pre-packaged) it would save significant energy costs and allow him to redirect his staff to running the OR and surgery schedule for the day.
Roy Morgan: There are three key trends we see in the marketplace for packaging and sterilization services in the last year. First are concerns about the long-term viability of EtO sterilization suppliers and the risks associated with potential plant closures due to health and safety concerns and the concomitant supply chain constraints that creates. There is also continued interest in standardized packaging configurations that can save time in development for startups looking to reduce time-to-market. Finally, there is desire for improved packaging materials to combat sterility barrier failures due to distribution system challenges (moisture, vibration, impact, drop, aging). On the sterilization side, we have recently noticed an uptick of interest in our vertically integrated capacity for Hydrogen Peroxide Gas Plasma sterilization, which we attribute to the EtO concerns.
John Nino: The orthopedic industry is facing an evolution anticipated to increase the need for sterilization, validation, and sterile packaged devices dedicated to an aging population and conversely, an expanding demand for sports-related injury devices. The critical component when considering packaging and sterilization is the risk of infection. To successfully meet evolving industry demand and minimize infection risks, orthopedic device makers will need increased support via sterile packaging availability and device sterilization from a strategic partner that bolsters their growth and innovation in a timely manner.
Thor Rollins: The most dominant market forces we see revolve around sterilization choices, their availability, and inherent suitability for a device. There are many sterilization choices, but manufacturers often tend to stick with what they know versus exploring other sterilization methods that may be better suited for their needs. We currently see a reexamination of orthopedic materials: manufacturers are re-evaluating their materials for multiple of reasons at this moment in time. One might be to have options for their sterilization, or to have a backup in case of delays or unforeseen issues. Other factors could be to reduce carbon footprint, improve the patient experience, or increase the device’s longevity and then reduce the surgery frequency. Our recommendation is to partner early with their sterilization provider to optimize outcomes and increase efficiencies.
Don Tumminelli: Now that the smoke has cleared (for the most part) with COVID, many of the elective surgeries either cancelled or postponed during the pandemic are now being scheduled, which creates a backlog as we all play catch up. In addition, the drive for orthopedic surgeries such as hip/knee/shoulder replacements is increasing as the technology continues to evolve and the time between a second replacement widens. More patients are making the decision to move forward. This drive is allowing for new innovation and spurs research for better, less invasive ways for the procedure.
Benjamin White: We saw how orthopedics manufacturers addressed the realities of EU MDR enforcement, from package conversion to serialization of components. We also see the overall pandemic-driven shift to a greater proportion of procedures performed in same-day surgery and ambulatory surgery centers (ASCs), which has pushed the market toward more single-use instrument sets and led to changes in packaging. Such an increase is pushing us toward addressing sustainability, with strides made in advancing circular packaging and other means of reducing our single-use plastic waste. We also see changes concerning sterilization, as OEMs consider whether to move away from EtO or revalidate toward more environmentally friendly parameters. As availability of X-ray sterilization continues to grow, we are likely to see increasing adoption of this method as well. Finally, there is supply chain pressure and fragility, especially the Tyvek shortage affecting packaging materials, but supply chain isn’t the headline news it was in 2020 and 2021, as many OEMs have worked through what they can control and plan.
Brusco: Please explain your packaging and related services and how they benefit medical/orthopedic device makers.
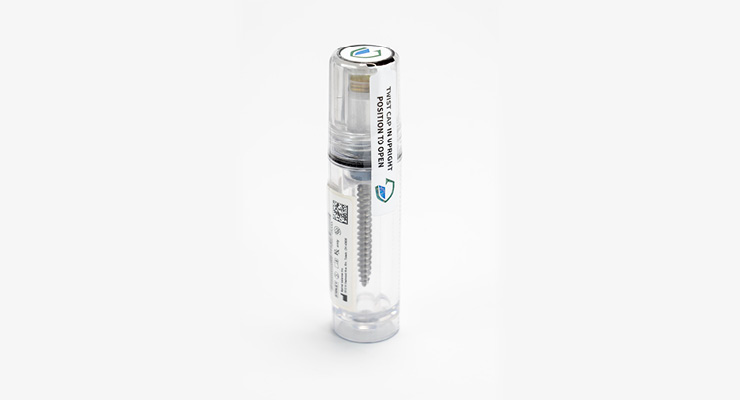
Kennedy: Our CapSure packaging system is a series of injection-molded tube bodies and mating lids in various lengths and diameters. The junction between the lid and body forms a seal unique to our industry. The material we use is Tritan, a USP class IV co-polyester. We have various solutions for holding and securing implants/devices within the tubes. A few of those are our own, but we also use TPUs, backer cards, clam shells, and films.
The main advantages to a device maker are a significant reduction in package size, toughness, and durability of the injection-molded packaging, dependability of the seal, visibility of the implant, and a reduction in the number of package components. The method of opening the package and presenting the implant to the sterile field is simple and quick to do in an aseptic manner.
Morgan: Our range of packaging services is expanding as we roll out our highly anticipated True-Validated packaging solution. We’ve taken “pre-validated packaging” to its logical conclusion by pre-validating every step of the packing and sterilization process. We provide a submission-ready document set, so if an orthopedic device fits into our pouch and is irradiated, the only remaining step is to write the adoption rationale. That means a company can possibly complete an FDA submission in under three weeks, which will be transformative for cash-starved startups.
Nino: We can meet packaging validation needs of orthopedic device makers while offering confidence they will meet ISO 11607 standards. These include heat seal validations (OQ/PQ), distributed simulation (D4169, ISTA), accelerated aging at most temperatures and RH requirements, and real-time aging.
Device manufacturers can work with one vendor who can meet all their sterile packaging needs—there is no need to qualify multiple vendors and deal with different resources. To accelerate the process and offer enhanced flexibility, we keep a variety of pre-validated packaging solutions in stock, such as Tyvek pouches and thermoformed trays with Tyvek lids, to ensure supply chain and get product to market even faster. Our class 7 cleanroom includes qualified tray and pouch sealers, a dedicated washroom fed by our own DI water system, and ultrasonic tanks and standard cleaning agents available for any cleaning requirements prior to packaging. Our facilities also house an ISTA certified package testing facility. Meanwhile, our robust quality system allows for documentation control of hundreds of SKUs for any given company. We have the ability to design and print labels for all of them, including UDI implantation.
Tumminelli: We work with the final package design to validate the ability to maintain sterility. Through real-time and accelerated aging of samples along the ISO 11607 series, the sterile barrier can be assessed for breaches through a series of different analyses such as dye migration, bubble, burst, and seal peel testing. Another lesser known analysis, which FDA has been asking for more and more, is the microbial aerosol challenge, where samples are placed in a chamber with ambient or dynamic pressure to expose them to an aerosol of spores. If the packaging system has a breach, this method is designed to detect it.
White: When orthopedic manufacturers launch new products, getting to market can be costly and time-consuming. The reasons include the need to run the gauntlet on package validations, which are intended to safeguard quality and sterility to enable aseptic transfer of devices into patients. Without the right expertise and resources, OEMs can encounter delays when it comes to package integrity testing, and these can ultimately push back product launches and threaten the ability to generate return on investment.
Pre-validated packaging solutions can accelerate time to market for orthopedic OEMs by as much as 50% in some cases. Several years ago, we developed a universal packaging platform that fits up to 80% of spinal and extremity implants. We offer it in tray and pouch configurations. The tray is a double sterile barrier thermoform tray with two polyurethane liners for protection, inner and outer lids, and a shelf carton. Products in the tray packaging can be sterilized by gamma irradiation, EtO, or e-beam. We also offer FastLane pouches, which can be sterilized by most methods. These tray and pouch configurations conform to all industry-recognized standards. In addition, OEMs benefit from elimination of tooling and design costs, and a smaller footprint that reduces material needs.
Brusco: Please explain your range of sterilization and related services and how they benefit orthopedic device makers.
Bianchi: We offer traditional sterilization solutions like saturated steam and EtO used for heat-sensitive products, for which a thermal treatment is not possible. In the last few years, we also introduced low-temperature HyPerPure sterilization technology, which works with hydrogen peroxide under deep vacuum conditions and zero air and is an adequate replacement of old technologies like EtO and gamma rays. The process is very fast, saving time and money for the manufacturer, can be internalized inside the production plant, and from a green point of view, is carbon free and doesn't release pollution into the environment.
Morgan: Sterilization services continue to be impacted by issues with EtO processors: more plants have been shut down resulting in capacity constraints and longer lead times. The response among the chemical sterilant community has been to move toward new “minimum-dose” cycles that can reduce the amount of potentially hazardous sterilant used in the industrial settings of contract manufacturing/sterilization. This can help avert the potential human casualties of cancer-clusters by greatly reducing potential exposure to sterilant fluids that are highly toxic in the concentrated form. The industry is also hard at work developing alternatives to EtO and the FDA will likely fast-track promising new sterilization modalities, but widespread adoption will still take many years. We offer in-house HPGP sterilization, which is an FDA “established” sterilization modality, and have capacity to take on new projects. HPGP effectively sterilizes bioburden, is the preferred sterilization method for many small orthopedic devices, and is environmentally safe—the byproducts are simple and non-toxic water and oxygen.
Nino: We serve the orthopedic device industry with specialized sterilization services dedicated to meeting stringent requirements and the fast turnaround times needed to avoid backorder situations. Our in-house capabilities include steam and EtO sterilization, while our contracted capacity for external resources include gamma processing. Our staff such as validation engineers and a microbiologist are equipped with the latest training to execute validation procedures accurately and quickly. We also offer management of quarterly dose audit procedures to further enhance efficiency, reliability, and expediency.
Rollins: There are several different methods of sterilization that can be used, including: EtO sterilization, gamma irradiation, electron beam irradiation, X-ray irradiation, steam sterilization (autoclaving), and other novel methods e.g., Nitrogen Dioxide sterilization and Vaporized Hydrogen Peroxide sterilization (VHP). The choice and benefits of each method come down to many variables, some of the most common are: compatibility of the medical device with the methods, availability of sterilizers, cost, timelines, and design of the device. Several methods may be appropriate for orthopedic devices—to determine the best method, orthopedic device manufacturers should seek input from their sterilization partner.
To expand, a medical device manufacturer might want to choose one sterilization methodology over another for a variety of reasons:
Tumminelli: Many orthopedic companies market a specific set of instruments used to perform the procedure. Many of these devices are reusable and come in the form of instrument sets often loaned to the healthcare facility. The instruments must be cleaned and sterilized between patients per the manufacturer's IFU. We offer these cleaning validations for manual and automated, as well as for those within the U.S. and EU. Capabilities for sterilization validations include steam, EtO, VHP and dry heat—all within FDA cleared healthcare sterilizers per ISO 14937 and/or 17665.
Brusco: What other value-added services do you offer, and why is it important to have them?
Bianchi: We offer an experience of more than 70 years in the field, especially for new technologies such as HyPerPure. We also offer a service of preliminary tests in our laboratories to verify the compatibility of materials, the effectiveness of sterilization, and support customers towards the use of the new technology from a regulation standpoint.
Kennedy: Our value-added services come from the CapSure system itself. Our customers have told us having the ability to consider single-barrier packaging options is highly important, especially as they seek ways to improve and simplify the accuracy, speed and delivery of implants to the surgeon. Another key and somewhat unexpected value-add is when our client learns Tritan is a recyclable material and Eastman (the supplier) has a system for repolymerizing the material and repurposing it for a non-medical use. This is a gain share for everyone: the device maker, healthcare facility, and environment.
An economic service we offer is a quantitative cost review looking at the lifecycle of the package. We go beyond the normal process of tabulating tooling, testing, component cost, and processing. We identify actual cost savings in terminal sterilization and transportation associated with the space efficiency of using tube packaging.
White: We offer clean room packaging, medical device specific warehousing, finished goods distribution, loaner kit management, advanced inspection and reverse logistics services—all with a focus on quality.
We’re also excited to announce we’ve launched Millstone Testing Services, our new division offering a comprehensive range of product, packaging, and environmental testing for the medical device and pharmaceutical industries. In November 2022, we acquired two contract testing companies, pooling their 90 years of experience in regulatory testing services, and bringing them in-house. With an expanded range of testing services, we can offer better controls around product testing, reduced lead times for in-process testing within production, and accelerated time to market.
Reference
In a letter to the President,¹ AdvaMed president and CEO Scott Whitaker stated that the medtech industry welcomes the updated regulations for EtO sterilization facilities but asks that even though the Environmental Protection Agency (EPA) hasn’t threatened to ban EtO sterilization, the agency should “carefully reconsider language that might unreasonably alarm residents near sterilization facilities.”
Whitaker outlines his and the industry’s concern further in the letter: “We would ask that you consider the potential threat to patient care if any sterilization facilities shut down. With 20 billion medical devices sterilized using EtO each year in the U.S. at about only 100 facilities, the closure of even a small percentage of facilities could harm patient access to health care. EtO sterilization is at capacity. With 80 percent of surgical kits alone sterilized using EtO, any shutdown-induced disruption could reverberate from screening to the operating room to post-operative care.”
Whitaker said this concern came to fruition when a prior facility closure brought about the temporary shortage of pediatric breathing tubes, according to the U.S. Food and Drug Administration (FDA), and that the federal agency also expressed concerns about medical device availability should more facilities close.
He called on the EPA to “embrace technology-neutral solutions to meet new emissions targets” as well as “consider background EtO levels in ambient air and the tiny proportion of that represented by medical device sterilization EtO use.” Whitaker concluded by reiterating that the medtech industry and FDA are working to explore alternative sterilization methods.
In order to gain more insight on the EtO discourse and other prevalent trends, market forces, and challenges affecting medical/orthopedic device packaging and sterilization, ODT spoke to several experts in the space:
- Marco Bianchi, marketing, sales, and communication at De Lama S.p.A.
- Don Kennedy, VP sales and marketing, Guardian Medical USA.
- Roy Morgan, CEO, Eagle Medical Packaging, Sterilization Inc.
- John Nino, CEO, Life Science Outsourcing.
- Thor Rollins, B.S. RM(NRCM), senior director, expert advisory services, Sterigenics and Nelson Labs.
- Don Tumminelli, senior technical manager, client services at HIGHPOWER Validation Testing & Lab Services.
- Benjamin White, director of technical services, Millstone Medical Outsourcing.
Marco Bianchi: As a manufacturer of sterilizers, we see from the perspective of long-time and well-known technologies, such as gamma ray and EtO sterilization. From the other side, there is a great push from authorities and producers for a greener, more sustainable technology, and we are deeply involved in making the world aware of our new HyPerPure technology, a solution for these topics.
Don Kennedy: First, rising costs associated with terminal sterilization of devices and transportation of surgery sets; and second, price reduction practices enacted in good conscience by payors that end up preventing adoption of more efficient products or services that can be proven and demonstrated to lower operating costs. Another way to express this is cutting costs but not actually reducing them due to inefficient practices.
An example of the latter is the cost of hot water at healthcare facilities. It’s a lesson I learned from an ASC owner who asked what I thought the most expensive cost was at his facility. I answered “people,” but he told me it was the energy bill he paid to run the steam autoclaves, and if he could have all his implants provided terminally sterile (pre-packaged) it would save significant energy costs and allow him to redirect his staff to running the OR and surgery schedule for the day.
Roy Morgan: There are three key trends we see in the marketplace for packaging and sterilization services in the last year. First are concerns about the long-term viability of EtO sterilization suppliers and the risks associated with potential plant closures due to health and safety concerns and the concomitant supply chain constraints that creates. There is also continued interest in standardized packaging configurations that can save time in development for startups looking to reduce time-to-market. Finally, there is desire for improved packaging materials to combat sterility barrier failures due to distribution system challenges (moisture, vibration, impact, drop, aging). On the sterilization side, we have recently noticed an uptick of interest in our vertically integrated capacity for Hydrogen Peroxide Gas Plasma sterilization, which we attribute to the EtO concerns.
John Nino: The orthopedic industry is facing an evolution anticipated to increase the need for sterilization, validation, and sterile packaged devices dedicated to an aging population and conversely, an expanding demand for sports-related injury devices. The critical component when considering packaging and sterilization is the risk of infection. To successfully meet evolving industry demand and minimize infection risks, orthopedic device makers will need increased support via sterile packaging availability and device sterilization from a strategic partner that bolsters their growth and innovation in a timely manner.
Thor Rollins: The most dominant market forces we see revolve around sterilization choices, their availability, and inherent suitability for a device. There are many sterilization choices, but manufacturers often tend to stick with what they know versus exploring other sterilization methods that may be better suited for their needs. We currently see a reexamination of orthopedic materials: manufacturers are re-evaluating their materials for multiple of reasons at this moment in time. One might be to have options for their sterilization, or to have a backup in case of delays or unforeseen issues. Other factors could be to reduce carbon footprint, improve the patient experience, or increase the device’s longevity and then reduce the surgery frequency. Our recommendation is to partner early with their sterilization provider to optimize outcomes and increase efficiencies.
Don Tumminelli: Now that the smoke has cleared (for the most part) with COVID, many of the elective surgeries either cancelled or postponed during the pandemic are now being scheduled, which creates a backlog as we all play catch up. In addition, the drive for orthopedic surgeries such as hip/knee/shoulder replacements is increasing as the technology continues to evolve and the time between a second replacement widens. More patients are making the decision to move forward. This drive is allowing for new innovation and spurs research for better, less invasive ways for the procedure.
Benjamin White: We saw how orthopedics manufacturers addressed the realities of EU MDR enforcement, from package conversion to serialization of components. We also see the overall pandemic-driven shift to a greater proportion of procedures performed in same-day surgery and ambulatory surgery centers (ASCs), which has pushed the market toward more single-use instrument sets and led to changes in packaging. Such an increase is pushing us toward addressing sustainability, with strides made in advancing circular packaging and other means of reducing our single-use plastic waste. We also see changes concerning sterilization, as OEMs consider whether to move away from EtO or revalidate toward more environmentally friendly parameters. As availability of X-ray sterilization continues to grow, we are likely to see increasing adoption of this method as well. Finally, there is supply chain pressure and fragility, especially the Tyvek shortage affecting packaging materials, but supply chain isn’t the headline news it was in 2020 and 2021, as many OEMs have worked through what they can control and plan.
Brusco: Please explain your packaging and related services and how they benefit medical/orthopedic device makers.
Kennedy: Our CapSure packaging system is a series of injection-molded tube bodies and mating lids in various lengths and diameters. The junction between the lid and body forms a seal unique to our industry. The material we use is Tritan, a USP class IV co-polyester. We have various solutions for holding and securing implants/devices within the tubes. A few of those are our own, but we also use TPUs, backer cards, clam shells, and films.
The main advantages to a device maker are a significant reduction in package size, toughness, and durability of the injection-molded packaging, dependability of the seal, visibility of the implant, and a reduction in the number of package components. The method of opening the package and presenting the implant to the sterile field is simple and quick to do in an aseptic manner.
Morgan: Our range of packaging services is expanding as we roll out our highly anticipated True-Validated packaging solution. We’ve taken “pre-validated packaging” to its logical conclusion by pre-validating every step of the packing and sterilization process. We provide a submission-ready document set, so if an orthopedic device fits into our pouch and is irradiated, the only remaining step is to write the adoption rationale. That means a company can possibly complete an FDA submission in under three weeks, which will be transformative for cash-starved startups.
Nino: We can meet packaging validation needs of orthopedic device makers while offering confidence they will meet ISO 11607 standards. These include heat seal validations (OQ/PQ), distributed simulation (D4169, ISTA), accelerated aging at most temperatures and RH requirements, and real-time aging.
Device manufacturers can work with one vendor who can meet all their sterile packaging needs—there is no need to qualify multiple vendors and deal with different resources. To accelerate the process and offer enhanced flexibility, we keep a variety of pre-validated packaging solutions in stock, such as Tyvek pouches and thermoformed trays with Tyvek lids, to ensure supply chain and get product to market even faster. Our class 7 cleanroom includes qualified tray and pouch sealers, a dedicated washroom fed by our own DI water system, and ultrasonic tanks and standard cleaning agents available for any cleaning requirements prior to packaging. Our facilities also house an ISTA certified package testing facility. Meanwhile, our robust quality system allows for documentation control of hundreds of SKUs for any given company. We have the ability to design and print labels for all of them, including UDI implantation.
Tumminelli: We work with the final package design to validate the ability to maintain sterility. Through real-time and accelerated aging of samples along the ISO 11607 series, the sterile barrier can be assessed for breaches through a series of different analyses such as dye migration, bubble, burst, and seal peel testing. Another lesser known analysis, which FDA has been asking for more and more, is the microbial aerosol challenge, where samples are placed in a chamber with ambient or dynamic pressure to expose them to an aerosol of spores. If the packaging system has a breach, this method is designed to detect it.
White: When orthopedic manufacturers launch new products, getting to market can be costly and time-consuming. The reasons include the need to run the gauntlet on package validations, which are intended to safeguard quality and sterility to enable aseptic transfer of devices into patients. Without the right expertise and resources, OEMs can encounter delays when it comes to package integrity testing, and these can ultimately push back product launches and threaten the ability to generate return on investment.
Pre-validated packaging solutions can accelerate time to market for orthopedic OEMs by as much as 50% in some cases. Several years ago, we developed a universal packaging platform that fits up to 80% of spinal and extremity implants. We offer it in tray and pouch configurations. The tray is a double sterile barrier thermoform tray with two polyurethane liners for protection, inner and outer lids, and a shelf carton. Products in the tray packaging can be sterilized by gamma irradiation, EtO, or e-beam. We also offer FastLane pouches, which can be sterilized by most methods. These tray and pouch configurations conform to all industry-recognized standards. In addition, OEMs benefit from elimination of tooling and design costs, and a smaller footprint that reduces material needs.
Brusco: Please explain your range of sterilization and related services and how they benefit orthopedic device makers.
Bianchi: We offer traditional sterilization solutions like saturated steam and EtO used for heat-sensitive products, for which a thermal treatment is not possible. In the last few years, we also introduced low-temperature HyPerPure sterilization technology, which works with hydrogen peroxide under deep vacuum conditions and zero air and is an adequate replacement of old technologies like EtO and gamma rays. The process is very fast, saving time and money for the manufacturer, can be internalized inside the production plant, and from a green point of view, is carbon free and doesn't release pollution into the environment.
Morgan: Sterilization services continue to be impacted by issues with EtO processors: more plants have been shut down resulting in capacity constraints and longer lead times. The response among the chemical sterilant community has been to move toward new “minimum-dose” cycles that can reduce the amount of potentially hazardous sterilant used in the industrial settings of contract manufacturing/sterilization. This can help avert the potential human casualties of cancer-clusters by greatly reducing potential exposure to sterilant fluids that are highly toxic in the concentrated form. The industry is also hard at work developing alternatives to EtO and the FDA will likely fast-track promising new sterilization modalities, but widespread adoption will still take many years. We offer in-house HPGP sterilization, which is an FDA “established” sterilization modality, and have capacity to take on new projects. HPGP effectively sterilizes bioburden, is the preferred sterilization method for many small orthopedic devices, and is environmentally safe—the byproducts are simple and non-toxic water and oxygen.
Nino: We serve the orthopedic device industry with specialized sterilization services dedicated to meeting stringent requirements and the fast turnaround times needed to avoid backorder situations. Our in-house capabilities include steam and EtO sterilization, while our contracted capacity for external resources include gamma processing. Our staff such as validation engineers and a microbiologist are equipped with the latest training to execute validation procedures accurately and quickly. We also offer management of quarterly dose audit procedures to further enhance efficiency, reliability, and expediency.
Rollins: There are several different methods of sterilization that can be used, including: EtO sterilization, gamma irradiation, electron beam irradiation, X-ray irradiation, steam sterilization (autoclaving), and other novel methods e.g., Nitrogen Dioxide sterilization and Vaporized Hydrogen Peroxide sterilization (VHP). The choice and benefits of each method come down to many variables, some of the most common are: compatibility of the medical device with the methods, availability of sterilizers, cost, timelines, and design of the device. Several methods may be appropriate for orthopedic devices—to determine the best method, orthopedic device manufacturers should seek input from their sterilization partner.
To expand, a medical device manufacturer might want to choose one sterilization methodology over another for a variety of reasons:
- Different orthopedic devices may require different sterilization methods. Certain materials may not be able to withstand certain sterilization methods, such as high temperatures, radiation energy, or certain chemicals.
- Some sterilization methods are more effective against certain types of microorganisms than others. Steam sterilization is effective against most microorganisms, but may not be as effective against bacterial spores.
- The device's intended use may also influence the sterilization method chosen. For example, devices that will be used in a sterile field, such as surgical instruments or orthopedic implants, may require a higher level of sterilization than devices that will be used in a non-sterile field, such as diagnostic equipment.
- Product and business objectives also influence the sterilization method chosen—e.g., production volume, supply chain needs. For example, a product manufactured in volumes of many truckloads per week is more likely to require a high volume industrial sterilization process, whereas a custom designed implant manufactured the night before a procedure may require a fast sterilization method that can be executed the day of product manufacture.
- Regulatory agencies may have specific requirements or recommendations for sterilization methods, so a manufacturer may need to choose a method that follows those regulations.
Tumminelli: Many orthopedic companies market a specific set of instruments used to perform the procedure. Many of these devices are reusable and come in the form of instrument sets often loaned to the healthcare facility. The instruments must be cleaned and sterilized between patients per the manufacturer's IFU. We offer these cleaning validations for manual and automated, as well as for those within the U.S. and EU. Capabilities for sterilization validations include steam, EtO, VHP and dry heat—all within FDA cleared healthcare sterilizers per ISO 14937 and/or 17665.
Brusco: What other value-added services do you offer, and why is it important to have them?
Bianchi: We offer an experience of more than 70 years in the field, especially for new technologies such as HyPerPure. We also offer a service of preliminary tests in our laboratories to verify the compatibility of materials, the effectiveness of sterilization, and support customers towards the use of the new technology from a regulation standpoint.
Kennedy: Our value-added services come from the CapSure system itself. Our customers have told us having the ability to consider single-barrier packaging options is highly important, especially as they seek ways to improve and simplify the accuracy, speed and delivery of implants to the surgeon. Another key and somewhat unexpected value-add is when our client learns Tritan is a recyclable material and Eastman (the supplier) has a system for repolymerizing the material and repurposing it for a non-medical use. This is a gain share for everyone: the device maker, healthcare facility, and environment.
An economic service we offer is a quantitative cost review looking at the lifecycle of the package. We go beyond the normal process of tabulating tooling, testing, component cost, and processing. We identify actual cost savings in terminal sterilization and transportation associated with the space efficiency of using tube packaging.
White: We offer clean room packaging, medical device specific warehousing, finished goods distribution, loaner kit management, advanced inspection and reverse logistics services—all with a focus on quality.
We’re also excited to announce we’ve launched Millstone Testing Services, our new division offering a comprehensive range of product, packaging, and environmental testing for the medical device and pharmaceutical industries. In November 2022, we acquired two contract testing companies, pooling their 90 years of experience in regulatory testing services, and bringing them in-house. With an expanded range of testing services, we can offer better controls around product testing, reduced lead times for in-process testing within production, and accelerated time to market.
Reference