University of Missouri Health06.23.17
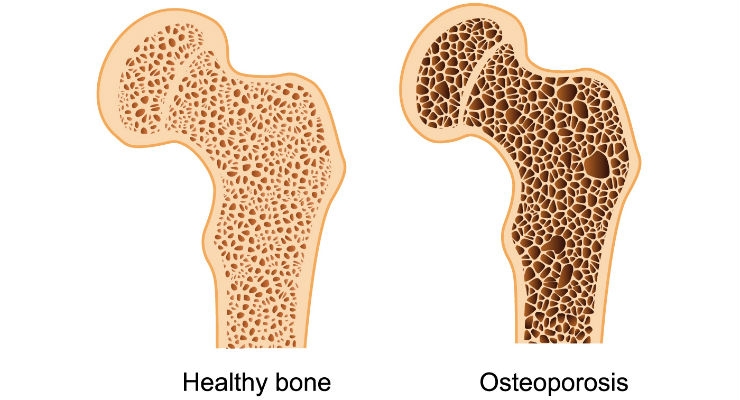
According to the National Center for Biotechnology Information, approximately 1.5 million Americans suffer osteoporosis-related fractures each year. Although comprehensive care for fragility fractures is available to patients, their understanding of risk factors, treatment adherence and the use of preventive screening remains low. Researchers at the University of Missouri School of Medicine reviewed recent osteoporosis treatment and management options with the goal of preventing complications from the disease.
“A fracture is the only true symptom of osteoporosis, and typically, that’s how the disease is diagnosed,” said Brett Crist, M.D., associate professor of orthopaedic surgery at the MU School of Medicine and senior author of the review. “Knowing risk factors―age, gender and family history―allows us to screen for osteoporosis and prevent complications. However, in our review, we found that preventable complications, such as secondary fractures, are more common than they should be. The reality is that death and disability associated with osteoporosis affect more people than most cancers. Previous research shows that the mortality rate for the elderly is 30 percent up to one year following a hip fracture.”
Crist, who also serves as an orthopaedic trauma surgeon at MU Health Care, said that several factors can lead to preventable secondary fractures.
“The use of preventive screening for osteoporosis is low,” Crist said. “The risk of decreased bone density starts at age 50, so it’s appropriate to start screening patients then to maximize the benefit and cost-effectiveness of fracture prevention. However, less than 27 percent of patients ages 65 to 79 are screened for the disease. Screening rates are even lower for both younger and older patient populations. Screening methods should include questionnaires and available tests for measuring bone density, such as a DEXA scan.”
Medication cost is another factor that can inhibit osteoporosis care. Although newer medications that require fewer doses and have fewer side effects are available, their use is relatively low because of their cost.
“Getting patients to follow their care plan sometimes can be a challenge, especially when it comes to prescribed medications,” Crist said. “Cost is definitely a factor. For example, a newer medication called Teriparatide increases bone density in patients with osteoporosis. However, a month’s supply of this medication without insurance costs about $3,000. The more cost-effective drugs often carry greater side effects and a more difficult dosing regimen.”
Calcium and Vitamin D are commonly prescribed for the treatment and management of osteoporosis. However, recent studies have called into question their effectiveness.
“These supplements are relatively inexpensive, over-the-counter treatment options,” Crist said. “For those reasons, patients tend to take them as suggested by their physician. However, some studies question the benefits of calcium supplements and suggest they may have unwanted side effects in some patients. More research is definitely needed in the area of calcium supplementation as a treatment option.”
Ultimately, Crist said that physicians need to have conversations with their patients about recent advances in osteoporosis treatment and management.
“Patients sometimes view osteoporosis as part of the normal aging process,” Crist said. “However, they take a significant risk if they don’t fully understand the consequences of their diagnosis. The development of an interdisciplinary care plan that meets the expectations and needs of the patient is the goal.”
The review, “Osteoporosis: A Discussion on the Past 5 Years,” recently was published in Current Reviews in Musculoskeletal Medicine. The review in this publication was supported by the Department of Orthopaedic Surgery at the MU School of Medicine.
“A fracture is the only true symptom of osteoporosis, and typically, that’s how the disease is diagnosed,” said Brett Crist, M.D., associate professor of orthopaedic surgery at the MU School of Medicine and senior author of the review. “Knowing risk factors―age, gender and family history―allows us to screen for osteoporosis and prevent complications. However, in our review, we found that preventable complications, such as secondary fractures, are more common than they should be. The reality is that death and disability associated with osteoporosis affect more people than most cancers. Previous research shows that the mortality rate for the elderly is 30 percent up to one year following a hip fracture.”
Crist, who also serves as an orthopaedic trauma surgeon at MU Health Care, said that several factors can lead to preventable secondary fractures.
“The use of preventive screening for osteoporosis is low,” Crist said. “The risk of decreased bone density starts at age 50, so it’s appropriate to start screening patients then to maximize the benefit and cost-effectiveness of fracture prevention. However, less than 27 percent of patients ages 65 to 79 are screened for the disease. Screening rates are even lower for both younger and older patient populations. Screening methods should include questionnaires and available tests for measuring bone density, such as a DEXA scan.”
Medication cost is another factor that can inhibit osteoporosis care. Although newer medications that require fewer doses and have fewer side effects are available, their use is relatively low because of their cost.
“Getting patients to follow their care plan sometimes can be a challenge, especially when it comes to prescribed medications,” Crist said. “Cost is definitely a factor. For example, a newer medication called Teriparatide increases bone density in patients with osteoporosis. However, a month’s supply of this medication without insurance costs about $3,000. The more cost-effective drugs often carry greater side effects and a more difficult dosing regimen.”
Calcium and Vitamin D are commonly prescribed for the treatment and management of osteoporosis. However, recent studies have called into question their effectiveness.
“These supplements are relatively inexpensive, over-the-counter treatment options,” Crist said. “For those reasons, patients tend to take them as suggested by their physician. However, some studies question the benefits of calcium supplements and suggest they may have unwanted side effects in some patients. More research is definitely needed in the area of calcium supplementation as a treatment option.”
Ultimately, Crist said that physicians need to have conversations with their patients about recent advances in osteoporosis treatment and management.
“Patients sometimes view osteoporosis as part of the normal aging process,” Crist said. “However, they take a significant risk if they don’t fully understand the consequences of their diagnosis. The development of an interdisciplinary care plan that meets the expectations and needs of the patient is the goal.”
The review, “Osteoporosis: A Discussion on the Past 5 Years,” recently was published in Current Reviews in Musculoskeletal Medicine. The review in this publication was supported by the Department of Orthopaedic Surgery at the MU School of Medicine.