ImmersiveTouch Inc.09.14.18
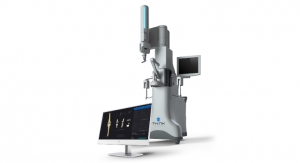
ImmersiveTouch Inc. announces the launch of ImmersiveView, the only suite of integrated virtual reality (VR) real-time solutions for personalized surgical planning, patient engagement and surgical training using patented haptic technology. ImmersiveView is designed to optimize outcomes and save costs, decreasing time in the operating room and improving pre-operative planning and patient satisfaction.
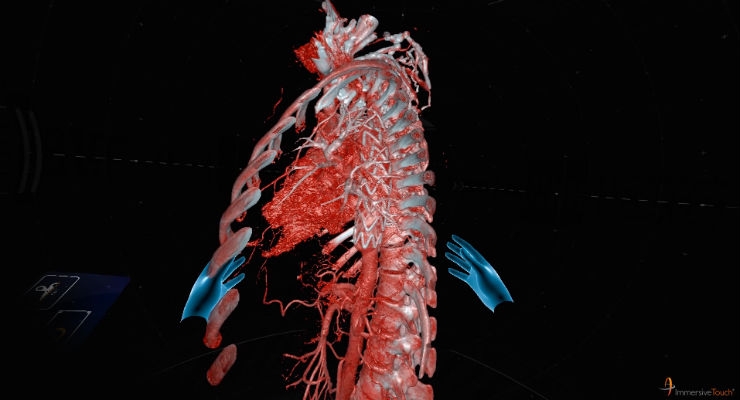
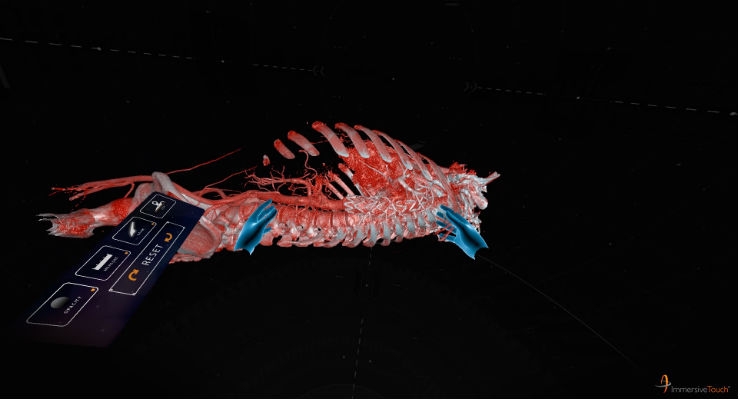
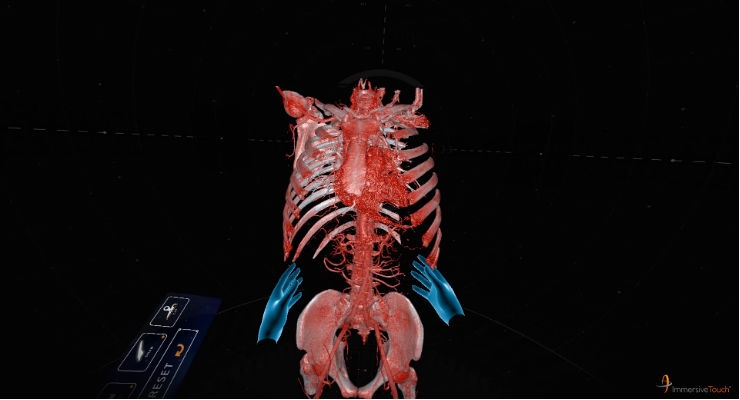
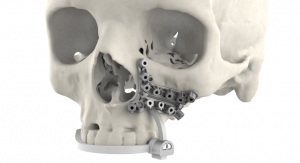
The ImmersiveView suite revolutionizes surgical planning by rapidly transforming existing patient computed tomography (CT) and magnetic resonance (MR) images into accurate, fully realized, high-resolution VR models that the physician can manipulate and explore from any angle, enabling a level of interaction not previously possible.
Advances in imaging in the last 15 years have led to three-dimensional (3D) recreations of anatomy, but they could only be viewed on a two-dimensional (2D) display, limiting the ability to fully interact with the model and assess the patient’s anatomy with full accuracy. ImmersiveView provides 3D visualization of medical imaging in a VR 3D display.
“Even though we could see patient anatomy in 3D, we could never interact with it because it was trapped in a 2D surface. ImmersiveView allows us to cross that glass barrier to the other side, into a different universe where we can immerse ourselves and interact with the anatomy from all angles using depth perception and even haptics to understand how it feels,” said Pravin K. Patel, M.D., chief of pediatric plastic and craniofacial surgery at the University of Illinois Heath & Medical Science Center and Chicago Shriners Hospitals for Children. “It helps our patients and family better understand what the surgeon sees and makes it real for them.”
ImmersiveView is highly intuitive, allowing the physician to grab, turn, expand and explore the VR model of the patient to evaluate procedural options and plan the surgery. With the touch of one button (which can be adjusted for right- and left-handedness), the user can:
Physicians also can use ImmersiveView to help patients experience, better understand and feel more comfortable with the procedure. Patients can ask more informed questions and participate in decision making, easing anxiety and supporting improved patient satisfaction and surgical conversion rates.
Another suite offering provides realistic VR surgical simulation using patented tactile (haptic) feedback. Surgical residents can familiarize themselves with the exact size, feel and internal workings of typical patients for specific surgeries and train as many times as needed to feel comfortable. The training system is fully customizable to all devices and scientifically proven to improve outcomes.1-5
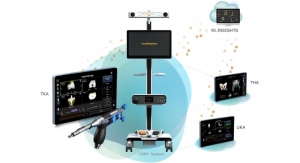
ImmersiveView is HIPAA-compliant, portable and fully compatible with all Patient Archiving and Communication (PAC) and Digital Imaging and Communications in Medicine (DICOM) systems. It can be used with any VR headset and system. Teams can participate in surgical planning by viewing the image the user is experiencing in VR on a display screen in person or via video conference. The ImmersiveView suite is more cost-effective and efficient than 3D printing and has replaced the service at some institutions.
“ImmersiveView helps physicians fully explore and understand their patients in 3D pixel by pixel, enabling them to do what they do even better,” said Pat Banerjee, Ph.D., CEO of ImmersiveTouch. “We have heard from users that ImmersiveView is a game changer, and we’re confident it will continue to revolutionize surgical practice, helping lead to fewer surgical errors and complications.”
ImmersiveTouch Inc. provides a suite of solutions for surgical planning, patient engagement and surgery skills training using groundbreaking virtual reality technology. Combining patient-specific 2D and 3D visual data, ImmersiveView provides a unique VR experience that aids surgeons and medical imaging specialists in optimal planning of surgical cases, enables patients to better understand their treatment and helps surgeons in training improve their skills using patented haptics.
References
1. Luciano C, et al. Learning retention of thoracic pedicle screw placement using a high-resolution augmented reality simulator with haptic feedback. Neurosurgery.. 2011 September; 69(Suppl OPERATIVE): 14-19.
2. Yudkowski R. Practice on an augmented reality/haptic simulator and library of virtual brains improves residents' ability to perform a ventriculostomy. Simul Healthc. 2013 Feb;8(1):25-31.
3. Schirmer CM. Virtual reality-based simulation training for ventriculostomy: an evidence-based approach.Neurosurgery. 2013 Oct;73 Suppl 1:66-73.
4. Gasco J. A novel virtual reality simulation for hemostasis in a brain surgical cavity: perceived utility for visuomotor skills in current and aspiring neurosurgery residents. World Neurosurg. 2013 Dec;80(6):732-7.
5. Sikder S. The use of a virtual reality surgical simulator for cataract surgical skill assessment with 6 months of intervening operating room experience. Clin Ophthalmol. 2015 Jan 20;9:141-9.
The ImmersiveView suite revolutionizes surgical planning by rapidly transforming existing patient computed tomography (CT) and magnetic resonance (MR) images into accurate, fully realized, high-resolution VR models that the physician can manipulate and explore from any angle, enabling a level of interaction not previously possible.
Advances in imaging in the last 15 years have led to three-dimensional (3D) recreations of anatomy, but they could only be viewed on a two-dimensional (2D) display, limiting the ability to fully interact with the model and assess the patient’s anatomy with full accuracy. ImmersiveView provides 3D visualization of medical imaging in a VR 3D display.
“Even though we could see patient anatomy in 3D, we could never interact with it because it was trapped in a 2D surface. ImmersiveView allows us to cross that glass barrier to the other side, into a different universe where we can immerse ourselves and interact with the anatomy from all angles using depth perception and even haptics to understand how it feels,” said Pravin K. Patel, M.D., chief of pediatric plastic and craniofacial surgery at the University of Illinois Heath & Medical Science Center and Chicago Shriners Hospitals for Children. “It helps our patients and family better understand what the surgeon sees and makes it real for them.”
ImmersiveView is highly intuitive, allowing the physician to grab, turn, expand and explore the VR model of the patient to evaluate procedural options and plan the surgery. With the touch of one button (which can be adjusted for right- and left-handedness), the user can:
- Measure
- Draw
- Cut
- Overlay and move a 2D scan of the patient anywhere in the image
- Better visualize specific parts of the anatomy by enabling transparency of tissues, such as bones, organs or blood vessels
- Take a picture and save it to the computer for later reference
Physicians also can use ImmersiveView to help patients experience, better understand and feel more comfortable with the procedure. Patients can ask more informed questions and participate in decision making, easing anxiety and supporting improved patient satisfaction and surgical conversion rates.
Another suite offering provides realistic VR surgical simulation using patented tactile (haptic) feedback. Surgical residents can familiarize themselves with the exact size, feel and internal workings of typical patients for specific surgeries and train as many times as needed to feel comfortable. The training system is fully customizable to all devices and scientifically proven to improve outcomes.1-5
ImmersiveView is HIPAA-compliant, portable and fully compatible with all Patient Archiving and Communication (PAC) and Digital Imaging and Communications in Medicine (DICOM) systems. It can be used with any VR headset and system. Teams can participate in surgical planning by viewing the image the user is experiencing in VR on a display screen in person or via video conference. The ImmersiveView suite is more cost-effective and efficient than 3D printing and has replaced the service at some institutions.
“ImmersiveView helps physicians fully explore and understand their patients in 3D pixel by pixel, enabling them to do what they do even better,” said Pat Banerjee, Ph.D., CEO of ImmersiveTouch. “We have heard from users that ImmersiveView is a game changer, and we’re confident it will continue to revolutionize surgical practice, helping lead to fewer surgical errors and complications.”
ImmersiveTouch Inc. provides a suite of solutions for surgical planning, patient engagement and surgery skills training using groundbreaking virtual reality technology. Combining patient-specific 2D and 3D visual data, ImmersiveView provides a unique VR experience that aids surgeons and medical imaging specialists in optimal planning of surgical cases, enables patients to better understand their treatment and helps surgeons in training improve their skills using patented haptics.
References
1. Luciano C, et al. Learning retention of thoracic pedicle screw placement using a high-resolution augmented reality simulator with haptic feedback. Neurosurgery.. 2011 September; 69(Suppl OPERATIVE): 14-19.
2. Yudkowski R. Practice on an augmented reality/haptic simulator and library of virtual brains improves residents' ability to perform a ventriculostomy. Simul Healthc. 2013 Feb;8(1):25-31.
3. Schirmer CM. Virtual reality-based simulation training for ventriculostomy: an evidence-based approach.Neurosurgery. 2013 Oct;73 Suppl 1:66-73.
4. Gasco J. A novel virtual reality simulation for hemostasis in a brain surgical cavity: perceived utility for visuomotor skills in current and aspiring neurosurgery residents. World Neurosurg. 2013 Dec;80(6):732-7.
5. Sikder S. The use of a virtual reality surgical simulator for cataract surgical skill assessment with 6 months of intervening operating room experience. Clin Ophthalmol. 2015 Jan 20;9:141-9.