Michael Barbella, Managing Editor03.21.18
Ira Kirschenbaum, M.D., never really gave much thought to his professional habitat.
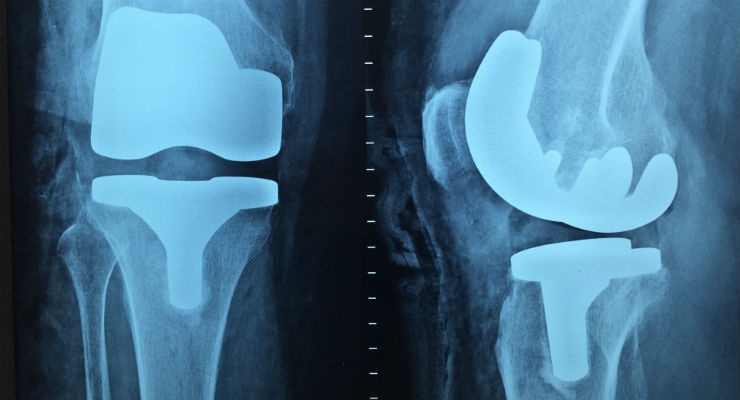
He’s spent more than two decades fixing broken or damaged knees, carefully drilling into bone, reattaching ligaments, and cementing new joints in place. Each case was different, thanks to the nature of human anatomy, but the surgical theater was always the same.
Kirschenbaum’s workplace was such a constant, in fact, that he never considered performing knee surgery outside the hospital setting. His outlook changed, though, once he became a patient.
“On Aug. 22, 2016, I had my left knee replaced as an outpatient, going home just two hours after the surgery ended,” Kirschenbaum, Orthopedics chairman at Bronx-Lebanon Hospital Center in New York, said. “As a surgeon, and now a patient, I can confirm this is the optimal way to perform total joint replacement for the correctly selected patient. The results are clinically equal, pain is less, patient satisfaction is higher, and the episode of care is more efficient and cost effective.”
For the right candidate, outpatient knee surgery can indeed be beneficial to both provider and recipient. But these cases historically have been rare due to patient safety and care quality concerns as well as reimbursement constraints.
Last fall, however, the Centers for Medicare and Medicaid Services (CMS) eliminated the latter obstacle by removing total knee arthroplasty (TKA) from its inpatient-only (IPO) list, thus allowing eligible Medicare recipients to undergo surgery on an outpatient basis beginning in January 2018. The decision capped a long, tempestuous debate in the orthopedic community that focused as much on money as it did on medicine.
Outpatient TKA opponents built their case mainly around patient safety, claiming non-hospital settings potentially could result in more emergency room visits for uncontrolled pain, blood clots, or other complications. Hospital executives, not surprisingly, focused on finances, complaining mostly about revenue losses from fewer multiple-day stays at their institutions.
Foes also voiced concerns over hospitals’ ability to reduce knee replacement surgery costs under the Comprehensive Care for Joint Replacement model and Bundled Payment for Care Initiative. Authorizing outpatient TKAs could hurt providers involved in these programs because their performance is compared to historical costs associated with joint replacements, Bruce Siegel, M.D., president and CEO of America’s Essential Hospitals, argued in a CMS comment letter.
“...the historical episode spending data might no longer be an accurate predictor of episode spending for beneficiaries receiving inpatient TKA procedures,” Siegel said in his letter. “Modifications to current Medicare payment models would be required if the TKA procedure is removed from the IPO list. This would lead to confusion among hospitals and CMS, as well as issues of accuracy and fairness in setting target prices.”
Outpatient TKA proponents claim the IPO removal will save Medicare hundreds of millions of dollars annually. They also note that technological advances are fueling a shift in care to non-hospital settings. More than 200 ambulatory surgery centers (ASCs) in the United States currently perform outpatient joint replacements, an eight-fold increase from 2014, according to Ambulatory Surgery Center Association (ASCA) data.
“There’s more comfort among surgeons who are coming out of residencies where they are trained to do surgeries on an outpatient basis,” ASCA chief operating officer Steve Miller said in published reports. “The volumes are doubling year over year.”
Maybe so, but CMS is not yet ready to reimburse outpatient TKAs performed at ASCs, as the agency’s IPO removal decision applies only to hospital outpatient departments. Mark I. Froimson, M.D., immediate past president of the American Association of Hip and Knee Surgeons (AAHKS), believes the CMS decision to limit outpatient TKAs to hospital-associated facilities shows the federal agency’s “desire to move slowly” in transitioning care.
In recent guidance to AAHKS members, Froimson alleges the policy change has sparked confusion among stakeholders, noting the inconsistency in interpretation among hospitals and surgeons is triggering doubts about their respective “freedom” to determine the most clinically appropriate location for knee surgery.
“Unfortunately, the unintended consequence of this [IPO rule] change has been an unprecedented amount of confusion on the part of a variety of stakeholders regarding how to interpret this new rule,” Froimson wrote in his Feb. 21 guidance. “Of additional concern is the fact that many are reporting that Medicare Advantage plans are directing their networks to drive the majority of TKAs to outpatient status, despite clear evidence that that was not CMS’s intent. This may be creating unsafe conditions for patients.”
To avoid any self-made safety hazards, Froimson outlined several recommendations to AAHKS members in his guidance. Chief among them was a suggestion to treat the vast majority of TKA cases as inpatient designations, since CMS itself acknowledged that it did not expect a “significant shift” in inpatient to outpatient procedures.
The guidance also advises physicians to clearly communicate reasons for not performing knee surgery in a hospital setting. In addition, the directive recommends doctors choose an outpatient designation for TKA only when it does not increase the risk of an adverse event. “It is expected at the present time, having little experience with treating TKA patients in outpatient departments, most of our members would continue to utilize the inpatient designation for the vast majority of their Medicare beneficiaries,” Froimson wrote.
He’s spent more than two decades fixing broken or damaged knees, carefully drilling into bone, reattaching ligaments, and cementing new joints in place. Each case was different, thanks to the nature of human anatomy, but the surgical theater was always the same.
Kirschenbaum’s workplace was such a constant, in fact, that he never considered performing knee surgery outside the hospital setting. His outlook changed, though, once he became a patient.
“On Aug. 22, 2016, I had my left knee replaced as an outpatient, going home just two hours after the surgery ended,” Kirschenbaum, Orthopedics chairman at Bronx-Lebanon Hospital Center in New York, said. “As a surgeon, and now a patient, I can confirm this is the optimal way to perform total joint replacement for the correctly selected patient. The results are clinically equal, pain is less, patient satisfaction is higher, and the episode of care is more efficient and cost effective.”
For the right candidate, outpatient knee surgery can indeed be beneficial to both provider and recipient. But these cases historically have been rare due to patient safety and care quality concerns as well as reimbursement constraints.
Last fall, however, the Centers for Medicare and Medicaid Services (CMS) eliminated the latter obstacle by removing total knee arthroplasty (TKA) from its inpatient-only (IPO) list, thus allowing eligible Medicare recipients to undergo surgery on an outpatient basis beginning in January 2018. The decision capped a long, tempestuous debate in the orthopedic community that focused as much on money as it did on medicine.
Outpatient TKA opponents built their case mainly around patient safety, claiming non-hospital settings potentially could result in more emergency room visits for uncontrolled pain, blood clots, or other complications. Hospital executives, not surprisingly, focused on finances, complaining mostly about revenue losses from fewer multiple-day stays at their institutions.
Foes also voiced concerns over hospitals’ ability to reduce knee replacement surgery costs under the Comprehensive Care for Joint Replacement model and Bundled Payment for Care Initiative. Authorizing outpatient TKAs could hurt providers involved in these programs because their performance is compared to historical costs associated with joint replacements, Bruce Siegel, M.D., president and CEO of America’s Essential Hospitals, argued in a CMS comment letter.
“...the historical episode spending data might no longer be an accurate predictor of episode spending for beneficiaries receiving inpatient TKA procedures,” Siegel said in his letter. “Modifications to current Medicare payment models would be required if the TKA procedure is removed from the IPO list. This would lead to confusion among hospitals and CMS, as well as issues of accuracy and fairness in setting target prices.”
Outpatient TKA proponents claim the IPO removal will save Medicare hundreds of millions of dollars annually. They also note that technological advances are fueling a shift in care to non-hospital settings. More than 200 ambulatory surgery centers (ASCs) in the United States currently perform outpatient joint replacements, an eight-fold increase from 2014, according to Ambulatory Surgery Center Association (ASCA) data.
“There’s more comfort among surgeons who are coming out of residencies where they are trained to do surgeries on an outpatient basis,” ASCA chief operating officer Steve Miller said in published reports. “The volumes are doubling year over year.”
Maybe so, but CMS is not yet ready to reimburse outpatient TKAs performed at ASCs, as the agency’s IPO removal decision applies only to hospital outpatient departments. Mark I. Froimson, M.D., immediate past president of the American Association of Hip and Knee Surgeons (AAHKS), believes the CMS decision to limit outpatient TKAs to hospital-associated facilities shows the federal agency’s “desire to move slowly” in transitioning care.
In recent guidance to AAHKS members, Froimson alleges the policy change has sparked confusion among stakeholders, noting the inconsistency in interpretation among hospitals and surgeons is triggering doubts about their respective “freedom” to determine the most clinically appropriate location for knee surgery.
“Unfortunately, the unintended consequence of this [IPO rule] change has been an unprecedented amount of confusion on the part of a variety of stakeholders regarding how to interpret this new rule,” Froimson wrote in his Feb. 21 guidance. “Of additional concern is the fact that many are reporting that Medicare Advantage plans are directing their networks to drive the majority of TKAs to outpatient status, despite clear evidence that that was not CMS’s intent. This may be creating unsafe conditions for patients.”
To avoid any self-made safety hazards, Froimson outlined several recommendations to AAHKS members in his guidance. Chief among them was a suggestion to treat the vast majority of TKA cases as inpatient designations, since CMS itself acknowledged that it did not expect a “significant shift” in inpatient to outpatient procedures.
The guidance also advises physicians to clearly communicate reasons for not performing knee surgery in a hospital setting. In addition, the directive recommends doctors choose an outpatient designation for TKA only when it does not increase the risk of an adverse event. “It is expected at the present time, having little experience with treating TKA patients in outpatient departments, most of our members would continue to utilize the inpatient designation for the vast majority of their Medicare beneficiaries,” Froimson wrote.