Mark Crawford, Contributing Editor08.12.22
Bringing additive manufacturing and procedural planning technologies to the point of care is an innovative way for healthcare systems to improve outcomes, increase efficiency, and reduce total costs. This approach is gaining popularity as more healthcare executives realize the benefits of point of care (POC). “Additive manufacturing adoption in hospitals is growing rapidly, spurred by the pandemic, increased demand for precision healthcare, and the affordability and availability of 3D printing solutions,” said Gaurav Manchanda, medical market development director for Formlabs, a Somerville, Mass.-based 3D printing technology developer and manufacturer.
3D printing (3DP) is used in surgical settings to help improve patient care across the spectrum of investigation, planning, procedural, and post-operative processes.
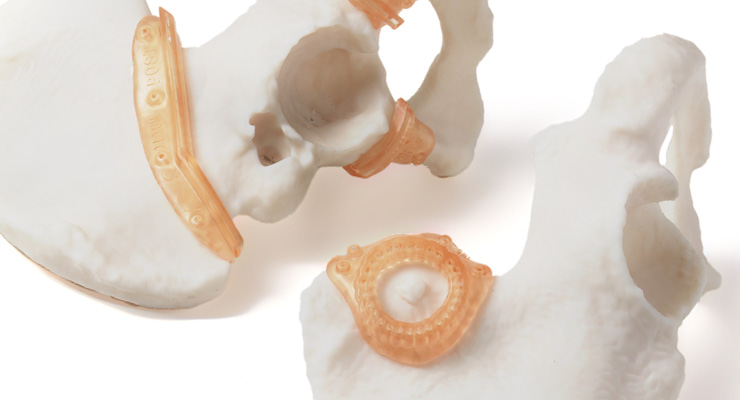
“For prosthetics, the ability to create custom fittings allows for maximum comfort, while geometrical freedom allowed by 3D printing means new design structures can be created for lighter, stronger prostheses,” said Jessica Coughlin, director of market access for healthcare for Stratasys, an Eden Prairie, Minn.- and Rehovot, Israel-based manufacturer of 3D printers, polymer materials, software, and 3D-printed parts on demand. “For medical devices, the reduction in production lead time and availability of biocompatible materials means more personalized solutions are getting to patients more quickly.”
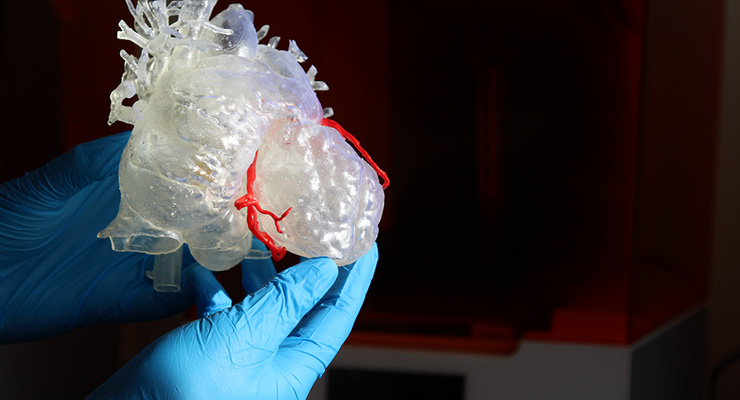
3D printing is also emerging as a new diagnostic tool for pre-surgical planning. 3D-printed models are extremely advantageous to surgeons—"for example, handling accurate physical replicas engages active spatial perception skills, enabling a more comprehensive understanding of the presented information in an inherently intuitive manner that cannot be achieved with conventional methods of imaging review that use screen-based 2D or volume-rendered representations,” Coughlin added.
The primary use case for POC AM/3DP (point of care additive manufacturing/3D printing) today is creating physical anatomical patient models, especially for patients with complex or rare conditions. Physicians analyze these models to determine the best treatment options, prepare for surgery, or explain procedures to patients—allowing them to make better-informed decisions that lead to improved patient outcomes.
Even with these advantages, “point-of-care manufacturing of implants is very rare and usually happens in close collaboration with a company or with a company as the legal manufacturer using AM equipment located at the hospital,” said Sebastian De Boodt, market manager of research and engineering for Materialise, a Belgium-based provider of certified medical software solutions for image-based planning and medical 3D printing, including personalized implants and surgical guides. “In these cases, AM is most often used for complex orthopedic revisions or for craniomaxillofacial [CMF] implants.”
Several academic institutions are also designing and printing their own surgical guides for various orthopedic osteotomy applications, or for CMF reconstruction. This is mostly occurring in Japan and Europe, and to a lesser extent, in the U.S. “For example, in-house 3D planning and printing of splints for orthognathic surgery is common in larger health centers, especially in Europe and Japan,” noted De Boodt.
POC AM technologies can also address supply chain gaps by enabling the production of medical supplies at the hospital when they are running low. In the regulatory realm, regulatory agencies are better-defining the compliance pathways that will ensure safe and effective medical devices are being created at the point of care, which will further accelerate investment in POC AM by healthcare facilities.
“Device manufacturers are devising programs to enable on-site printing of models and guides, thereby creating a competitive advantage by supporting healthcare providers’ demand for quicker, cost-effective access to patient-specific solutions,” said Ben Johnson, vice president of portfolio and regulatory for healthcare for 3D Systems, a Rock Hill, S.C.-based provider of additive manufacturing solutions for the medical device industry. “These manufacturers, in turn, partner with additive companies to provide expertise, technologies, and support services at the point of care.”
There is growing interest in patient-specific prosthetics manufactured with POC AM/3DP. Making custom prosthetics with AM in this setting eliminates the limitations of traditional manufacturing processes and is less expensive. Depending on the AM method, finely detailed features can be achieved in more complex designs. For parts with larger tolerances, such as prosthetic cups, such a level of detail/tolerance may not be required. Either way, a customized prosthetic is a more comfortable device for a patient and leads to an improved quality of life.
One of the biggest challenges to the advancement of POC AM/3DP is that there is no standard method to earn funding, noted De Boodt. Most labs earn initial funding through research and development grants and then leverage return-on-investment data to obtain internal hospital funding. In an effort to further support POC AM/3DP as a sustainable practice, “there are now several initiatives designed to help hospitals to get reimbursed,” he said. “For example, the Radiological Society of North America Special Interest Group for 3D Printing is building a registry of clinical data, which will help serve as a basis to obtain reimbursement. Similar initiatives are emerging throughout the world, including in Europe.”
Another advantage is having the radiology department, which is typically responsible for creating the anatomic models, available in the same location as the 3D printing lab to optimize communication directly with the surgeon about the anatomy of interest. “This eliminates the need for back-and-forth conversation through a third party that the surgeon does not have a working relationship with,” said Coughlin. “Also, communication can get lost in translation when discussing complex anatomy over the phone or via Webex.”
The cost of outsourcing also adds up, especially if there is high demand at the hospital. Institutions that set up a 3D-printing lab are successfully reaping the economic benefits. For example, Mayo Clinic was one of the first medical centers to invest in a state-of-the-art 3D printing lab and has made significant strides in exploring the innovative use of the technology. Almost all Mayo surgical departments, from pediatrics to neurosurgery to orthopedics, now routinely use their 3D printing service. “The widespread acceptance of the technology has significantly increased the case volume and helped to justify the cost,” said Coughlin. “It is now one of a few go-to institutions for educating clinicians and 3D-printing industries about medical 3D printing, which acts as additional revenue stream.”
POC AM/3DP also offers a big advantage in reducing lead times and increasing flexibility. The personalized AM-based devices offered by OEMs almost exclusively target elective procedures, which can be planned weeks or even months in advance. By manufacturing at the point of care, medical facilities can reduce lead times to days, giving hospitals the opportunity to use AM for non-elective procedures as well—for example, a patient who needs surgery immediately. At 3D LifePrints, a Liverpool, U.K.- and Houston, Texas-based provider of digital surgical planning services and the design and manufacture of patient-specific medical devices, “we have been able to supply patient-specific cutting guides for on-site surgeons within three days of receipt of scans,” stated CEO Henry Pinchbeck.
Offering POC AM/3DP on-site requires 1) engineering expertise to understand the possibilities and limitations of AM, and 2) clinical expertise to interpret medical images and understand what the treatment options are. By having the engineers and 3D printers on site, physicians and engineers can work together to create high-quality, clinically relevant models. “For surgical procedures that require multiple clinical specialties, the advantage of having engineers on-site is even bigger,” said De Boodt. “Some procedures require collaboration between many different specialists, where each might need a different model to visualize different structures. When 3D printing is done in-house, specialists can have their own models that leads to better collaboration throughout the team.”
In addition to saving time and cost, POC AM technologies have the benefit of driving not only training and education, but also innovation by immersing technologists, engineers, and clinicians in a collaborative environment. Having the engineer and physician in the same room discussing patient cases together makes it easier to generate new and better ways to solve problems. Advanced visualization tools also help explain procedures to patients and improve communication.
“3D printing is also a tool for advancing patient education—holding your own skull in your hand can be a powerful moment,” said Manchanda. “Rather than explaining difficult surgeries to patients, doctors can guide them through the procedure using a printed model of the patient’s own anatomy.”
Although such enthusiasm is exciting, it must be tempered by the many factors involved and the steep learning curve.
Pinchbeck noted a recurring issue is when hospitals purchase a 3D printer without knowing the many additional requirements related to the design and manufacture of medical devices. “Much of my time is spent educating hospitals that the staffing and software elements are just as important as the 3D printing itself,” he said. “There is a belief, even in the medical community, that the CT [computed tomography] or MRI [magnetic resonance imaging] scanner will spit out all the relevant data in a useable format and that is simply plugged in a 3D printer. This is far from the truth.”
Hospitals and clinics are becoming more aware of the quality issues and complex regulatory challenges posed by adopting POC AM and complying with the necessary standards. The amount of requirements is daunting. For example, there is often confusion in the healthcare market about what is legally required to manufacture medical devices at the point of care. Pinchbeck advises not to solely rely upon third-party testing or results. “Just because a 3D printer manufacturer or software provider has done a series of tests on their own materials/algorithms does not mean that a hospital or other provider can forego doing their own tests in order to legally manufacture and use the devices.”
To reduce complexity, hospitals seek a more streamlined workflow to keep things as simple as possible. There are many steps involved with creating traditional anatomic models and many hospitals do not have the resources to be completely involved in the POC AM process. “The more simplified and streamlined manufacturers can make their technologies, the happier the already resource-constrained hospital personnel will be,” said Coughlin.
For example, anatomy segmentation, in which a 2D scan is turned into a 3D virtual model of a part of the anatomy, is often still a time-consuming process, with difficult manual steps completed by highly specialized personnel. Hospitals are seeking an easier, preferably automated segmentation software approach to scale their operations more easily. Also, as regulations become increasingly stringent and complex, hospitals are looking for software vendors that can ensure their tools and methods comply with evolving regulations.
Segmentation software companies are developing more automated/artificial intelligence (AI)-enabled solutions that can segment DICOM (Digital Imaging and Communications in Medicine) images much faster than just a few years ago, saving hours of processing time. Also, 3D printers can now provide anatomical models that have similar biomechanical properties as native tissue and bone, allowing surgeons to operate on the model by cutting, suturing, drilling, and inserting devices just as they would in a real surgery.
Many POC centers are also exploring augmented reality (AR) as a technology to complement their AM applications. AR would be helpful for better visualization of 3D models and could also provide shorter lead times and lower costs. “3D printing will always play an important role because physical models can be helpful to surgeons, but some use cases might shift towards AR or warrant an AR model as well as a 3D-printed model,” said De Boodt.
Printers continue to improve and become more affordable. While there are many different AM technologies that are available (with a variety of price points to match), there is no single 3D printer that can meet all the needs of a POC facility. “For bony anatomical models, for example, a cheaper FDM [fused deposition modeling] printer is sensible to keep the price of the materials down, while surgical guides require sterilizable materials and high precision,” said Pinchbeck. “Similarly for software, there are some excellent, FDA-approved/CE marked suites of software; however, I strongly advise against using free software because it will not be adequately tested or maintained for the creation of medical devices.”
Currently, converting 2D medical scans into 3D-printable files, a process called segmentation, is a highly manual and slow process, requiring skilled engineers and specialty software. Therefore, one of the biggest challenges for delivering 3D models requests is speed. To expedite this process, Axial3D has created its “segmentation-as-a-service” solution that can deliver the 2D to 3D segmentation process within just a few hours, instead of days or weeks.
“Our order platform is hosted on the AWS [Amazon Web Services] cloud, which means that it can be accessed anywhere in the world; surgeons only need an Internet connection,” said Johnston. “The segmentation process is significantly reduced to just a few hours, or even minutes in less complex cases. The printable file then can be output into the hospital’s print lab or shipped the next day—making 3D modeling available for even the most time-sensitive cases.”
3D Systems recently acquired Kumovis and its R1 FDM printer, which enables extrusion printing in biocompatible polyetheretherketone [PEEK] and polyphenylsulfone [PPSU] materials. “Until now, these highly desired healthcare materials were only available through traditional manufacturing and patient-specific applications were expensive and time-consuming to produce,” said Johnson. “With the addition of this technology to our portfolio, hospitals will soon be able to manufacture patient-specific PEEK implants at the point of care.”
“The discussion paper provides insight into our perspective of the benefits and challenges of 3D printing at hospitals and other points of care and presents a potential approach for regulatory oversight under various scenarios to inform future policy development,” stated William Maisel, director of the Office of Product Evaluation and Quality for the FDA’s Center for Devices and Radiological Health.
The FDA proposed three different scenarios for adopting POC AM:
“AM solution providers can help augment AM capabilities at the POC, based on these proposed scenarios,” Johnson noted. “We understand the regulatory bodies and guidance with oversight on additive manufacturing and can help healthcare providers stay compliant by:
There is no doubt that POC AM is gaining momentum throughout the healthcare environment. According to a survey commissioned by Axial3D, 52% of the surgeons interviewed indicated they had changed their plan for a complex surgery after using a 3D model during planning; 47% reported the models helped them confirm the optimal plan much faster and with more certainty, compared to relying solely on 2D patient scans. “Planning procedures, aided by 3D models, lead to an average reduction of 62 minutes per case, and an average reduction of stay in hospital for the patient of 16%,” indicated Johnston.
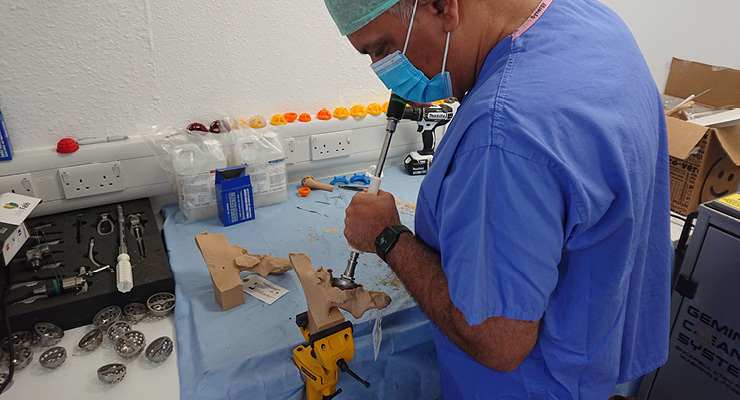
Pinchbeck added that some orthopedic surgeons prefer to practice their surgical procedures by going through the steps on anatomical models. “At several of our facilities, we have set up a simulation bench with a range of surgical tools and implants,” he said. “We then manufacture a model in appropriate materials and the surgeons can carry out test runs of the surgery on the models. This is hugely beneficial for implant sizing and also determining whether a custom-made implant is, or is not, required in a particular case. The simulation is even better when it is conducted in collaboration with the implant supplier, so that a full range of tools and implants are available at the onset of the simulation.”
Formlabs continues to see groundbreaking 3D printing applications as a next step toward wide-scale adoption. For example, it recently partnered with Vizient, one of the largest member-driven healthcare group purchasing organizations (GPO) in the nation, making it the first 3D printing company to be listed in a major GPO catalog.2 “This partnership reflects the increasing demand for 3D-printed surgical tools, medical supplies, and other solutions in hospitals and ambulatory surgical centers,” said Manchanda.
Even though the benefits of integrating POC AM/3DP into healthcare systems are clear, successful adoption of these technologies and services is dependent upon addressing a number of quality and compliance concerns, which remain the biggest challenges that POC AM/3DP faces today. In response, over the longer term, 3D Systems’ ultimate goal is to establish FDA-compliant medical device manufacturing centers of excellence at the point of care. Johnson indicated that overcoming facility, staffing, usage, and regulatory challenges at POC can be achieved through the aforementioned methods (i.e., establishing workflows, building quality management programs, and setting up control processes), plus:
“I believe we will see more hospitals that will be able to implement end-to-end solutions for patient-specific surgical planning and medical device manufacturing,” said Johnson. “This will disrupt existing healthcare models, reduce overall costs, and crucially, improve the quality of care.”
The roles and responsibilities for hospitals versus industry for POC AM/3DP will continue to evolve in the coming years, especially as regulations, logistics, and business models change.
“As devices and technology become more advanced, we will see a shift toward more collaborative intelligence between physicians and engineers,” said De Boodt. “Bringing some personalization aspects closer to the point of care makes it easier for physicians to understand 3D printing’s benefits and limitations. Even now they continue to see new opportunities all the time and will continue to collaborate with engineers on new and better ways to personalize treatment for improved patient outcomes.”
References
Mark Crawford is a full-time freelance business and marketing/communications writer based in Madison, Wis. His clients range from startups to global manufacturing leaders. He also writes a variety of feature articles for regional and national publications and is the author of five books.
3D printing (3DP) is used in surgical settings to help improve patient care across the spectrum of investigation, planning, procedural, and post-operative processes.
“For prosthetics, the ability to create custom fittings allows for maximum comfort, while geometrical freedom allowed by 3D printing means new design structures can be created for lighter, stronger prostheses,” said Jessica Coughlin, director of market access for healthcare for Stratasys, an Eden Prairie, Minn.- and Rehovot, Israel-based manufacturer of 3D printers, polymer materials, software, and 3D-printed parts on demand. “For medical devices, the reduction in production lead time and availability of biocompatible materials means more personalized solutions are getting to patients more quickly.”
3D printing is also emerging as a new diagnostic tool for pre-surgical planning. 3D-printed models are extremely advantageous to surgeons—"for example, handling accurate physical replicas engages active spatial perception skills, enabling a more comprehensive understanding of the presented information in an inherently intuitive manner that cannot be achieved with conventional methods of imaging review that use screen-based 2D or volume-rendered representations,” Coughlin added.
The primary use case for POC AM/3DP (point of care additive manufacturing/3D printing) today is creating physical anatomical patient models, especially for patients with complex or rare conditions. Physicians analyze these models to determine the best treatment options, prepare for surgery, or explain procedures to patients—allowing them to make better-informed decisions that lead to improved patient outcomes.
Even with these advantages, “point-of-care manufacturing of implants is very rare and usually happens in close collaboration with a company or with a company as the legal manufacturer using AM equipment located at the hospital,” said Sebastian De Boodt, market manager of research and engineering for Materialise, a Belgium-based provider of certified medical software solutions for image-based planning and medical 3D printing, including personalized implants and surgical guides. “In these cases, AM is most often used for complex orthopedic revisions or for craniomaxillofacial [CMF] implants.”
Several academic institutions are also designing and printing their own surgical guides for various orthopedic osteotomy applications, or for CMF reconstruction. This is mostly occurring in Japan and Europe, and to a lesser extent, in the U.S. “For example, in-house 3D planning and printing of splints for orthognathic surgery is common in larger health centers, especially in Europe and Japan,” noted De Boodt.
POC AM technologies can also address supply chain gaps by enabling the production of medical supplies at the hospital when they are running low. In the regulatory realm, regulatory agencies are better-defining the compliance pathways that will ensure safe and effective medical devices are being created at the point of care, which will further accelerate investment in POC AM by healthcare facilities.
Latest Trends
Hospitals are increasing the volume and diversity of their POC AM use cases, drawing on a greater variety of AM technologies and materials. They are looking for flexible solutions that can leverage the different technologies and methods to effectively manage the increasing complexity of their operations.“Device manufacturers are devising programs to enable on-site printing of models and guides, thereby creating a competitive advantage by supporting healthcare providers’ demand for quicker, cost-effective access to patient-specific solutions,” said Ben Johnson, vice president of portfolio and regulatory for healthcare for 3D Systems, a Rock Hill, S.C.-based provider of additive manufacturing solutions for the medical device industry. “These manufacturers, in turn, partner with additive companies to provide expertise, technologies, and support services at the point of care.”
There is growing interest in patient-specific prosthetics manufactured with POC AM/3DP. Making custom prosthetics with AM in this setting eliminates the limitations of traditional manufacturing processes and is less expensive. Depending on the AM method, finely detailed features can be achieved in more complex designs. For parts with larger tolerances, such as prosthetic cups, such a level of detail/tolerance may not be required. Either way, a customized prosthetic is a more comfortable device for a patient and leads to an improved quality of life.
One of the biggest challenges to the advancement of POC AM/3DP is that there is no standard method to earn funding, noted De Boodt. Most labs earn initial funding through research and development grants and then leverage return-on-investment data to obtain internal hospital funding. In an effort to further support POC AM/3DP as a sustainable practice, “there are now several initiatives designed to help hospitals to get reimbursed,” he said. “For example, the Radiological Society of North America Special Interest Group for 3D Printing is building a registry of clinical data, which will help serve as a basis to obtain reimbursement. Similar initiatives are emerging throughout the world, including in Europe.”
Advantages of POC AM
Surgeons use patient-specific 3D anatomical models to improve pre-operative planning, intra-team communications, and patient education. By using them for pre-operative planning, surgeons can tailor their treatment plan for individual patients, which shortens time in the OR, resulting in reduced complications and ultimately improved patient outcomes. “Having a 3D model as an additional visual aid improves the patient consent process and discussions with the surgical team,” said Roger Johnston, CEO for Axial3D, a Belfast, Ireland-based provider of additive manufacturing platforms that enable customized 3D-printed implants through its “segmentation as a service” platform.Another advantage is having the radiology department, which is typically responsible for creating the anatomic models, available in the same location as the 3D printing lab to optimize communication directly with the surgeon about the anatomy of interest. “This eliminates the need for back-and-forth conversation through a third party that the surgeon does not have a working relationship with,” said Coughlin. “Also, communication can get lost in translation when discussing complex anatomy over the phone or via Webex.”
The cost of outsourcing also adds up, especially if there is high demand at the hospital. Institutions that set up a 3D-printing lab are successfully reaping the economic benefits. For example, Mayo Clinic was one of the first medical centers to invest in a state-of-the-art 3D printing lab and has made significant strides in exploring the innovative use of the technology. Almost all Mayo surgical departments, from pediatrics to neurosurgery to orthopedics, now routinely use their 3D printing service. “The widespread acceptance of the technology has significantly increased the case volume and helped to justify the cost,” said Coughlin. “It is now one of a few go-to institutions for educating clinicians and 3D-printing industries about medical 3D printing, which acts as additional revenue stream.”
POC AM/3DP also offers a big advantage in reducing lead times and increasing flexibility. The personalized AM-based devices offered by OEMs almost exclusively target elective procedures, which can be planned weeks or even months in advance. By manufacturing at the point of care, medical facilities can reduce lead times to days, giving hospitals the opportunity to use AM for non-elective procedures as well—for example, a patient who needs surgery immediately. At 3D LifePrints, a Liverpool, U.K.- and Houston, Texas-based provider of digital surgical planning services and the design and manufacture of patient-specific medical devices, “we have been able to supply patient-specific cutting guides for on-site surgeons within three days of receipt of scans,” stated CEO Henry Pinchbeck.
Offering POC AM/3DP on-site requires 1) engineering expertise to understand the possibilities and limitations of AM, and 2) clinical expertise to interpret medical images and understand what the treatment options are. By having the engineers and 3D printers on site, physicians and engineers can work together to create high-quality, clinically relevant models. “For surgical procedures that require multiple clinical specialties, the advantage of having engineers on-site is even bigger,” said De Boodt. “Some procedures require collaboration between many different specialists, where each might need a different model to visualize different structures. When 3D printing is done in-house, specialists can have their own models that leads to better collaboration throughout the team.”
In addition to saving time and cost, POC AM technologies have the benefit of driving not only training and education, but also innovation by immersing technologists, engineers, and clinicians in a collaborative environment. Having the engineer and physician in the same room discussing patient cases together makes it easier to generate new and better ways to solve problems. Advanced visualization tools also help explain procedures to patients and improve communication.
“3D printing is also a tool for advancing patient education—holding your own skull in your hand can be a powerful moment,” said Manchanda. “Rather than explaining difficult surgeries to patients, doctors can guide them through the procedure using a printed model of the patient’s own anatomy.”
What Hospitals Want
The POC needs for a hospital depends on the size of the institution and its vision for POC AM. “We are seeing large chain hospitals and health systems wanting to be independent manufacturers of patient-specific devices at their facilities to reduce costs and drive innovation, essentially becoming manufacturers themselves,” said Johnson.Although such enthusiasm is exciting, it must be tempered by the many factors involved and the steep learning curve.
Pinchbeck noted a recurring issue is when hospitals purchase a 3D printer without knowing the many additional requirements related to the design and manufacture of medical devices. “Much of my time is spent educating hospitals that the staffing and software elements are just as important as the 3D printing itself,” he said. “There is a belief, even in the medical community, that the CT [computed tomography] or MRI [magnetic resonance imaging] scanner will spit out all the relevant data in a useable format and that is simply plugged in a 3D printer. This is far from the truth.”
Hospitals and clinics are becoming more aware of the quality issues and complex regulatory challenges posed by adopting POC AM and complying with the necessary standards. The amount of requirements is daunting. For example, there is often confusion in the healthcare market about what is legally required to manufacture medical devices at the point of care. Pinchbeck advises not to solely rely upon third-party testing or results. “Just because a 3D printer manufacturer or software provider has done a series of tests on their own materials/algorithms does not mean that a hospital or other provider can forego doing their own tests in order to legally manufacture and use the devices.”
To reduce complexity, hospitals seek a more streamlined workflow to keep things as simple as possible. There are many steps involved with creating traditional anatomic models and many hospitals do not have the resources to be completely involved in the POC AM process. “The more simplified and streamlined manufacturers can make their technologies, the happier the already resource-constrained hospital personnel will be,” said Coughlin.
For example, anatomy segmentation, in which a 2D scan is turned into a 3D virtual model of a part of the anatomy, is often still a time-consuming process, with difficult manual steps completed by highly specialized personnel. Hospitals are seeking an easier, preferably automated segmentation software approach to scale their operations more easily. Also, as regulations become increasingly stringent and complex, hospitals are looking for software vendors that can ensure their tools and methods comply with evolving regulations.
Technology Advances for POC AM
3D printing and advanced 3D planning can give physicians a deeper understanding of each patient’s individual anatomy and pathology, leading to better and more accurate planning and ideally more predictable patient outcomes. Physicians are eager to move beyond using POC AM for just visualizing anatomy of the patient to modeling different treatment options pre-surgery, using 3D printing for creating splints and guides. “For those benefits to scale to more routine clinical applications, there is a need for easier use and streamlined planning and printing tools, likely dedicated to specific clinical applications,” said De Boodt. “This reduces dependency on engineers.”Segmentation software companies are developing more automated/artificial intelligence (AI)-enabled solutions that can segment DICOM (Digital Imaging and Communications in Medicine) images much faster than just a few years ago, saving hours of processing time. Also, 3D printers can now provide anatomical models that have similar biomechanical properties as native tissue and bone, allowing surgeons to operate on the model by cutting, suturing, drilling, and inserting devices just as they would in a real surgery.
Many POC centers are also exploring augmented reality (AR) as a technology to complement their AM applications. AR would be helpful for better visualization of 3D models and could also provide shorter lead times and lower costs. “3D printing will always play an important role because physical models can be helpful to surgeons, but some use cases might shift towards AR or warrant an AR model as well as a 3D-printed model,” said De Boodt.
Printers continue to improve and become more affordable. While there are many different AM technologies that are available (with a variety of price points to match), there is no single 3D printer that can meet all the needs of a POC facility. “For bony anatomical models, for example, a cheaper FDM [fused deposition modeling] printer is sensible to keep the price of the materials down, while surgical guides require sterilizable materials and high precision,” said Pinchbeck. “Similarly for software, there are some excellent, FDA-approved/CE marked suites of software; however, I strongly advise against using free software because it will not be adequately tested or maintained for the creation of medical devices.”
Currently, converting 2D medical scans into 3D-printable files, a process called segmentation, is a highly manual and slow process, requiring skilled engineers and specialty software. Therefore, one of the biggest challenges for delivering 3D models requests is speed. To expedite this process, Axial3D has created its “segmentation-as-a-service” solution that can deliver the 2D to 3D segmentation process within just a few hours, instead of days or weeks.
“Our order platform is hosted on the AWS [Amazon Web Services] cloud, which means that it can be accessed anywhere in the world; surgeons only need an Internet connection,” said Johnston. “The segmentation process is significantly reduced to just a few hours, or even minutes in less complex cases. The printable file then can be output into the hospital’s print lab or shipped the next day—making 3D modeling available for even the most time-sensitive cases.”
3D Systems recently acquired Kumovis and its R1 FDM printer, which enables extrusion printing in biocompatible polyetheretherketone [PEEK] and polyphenylsulfone [PPSU] materials. “Until now, these highly desired healthcare materials were only available through traditional manufacturing and patient-specific applications were expensive and time-consuming to produce,” said Johnson. “With the addition of this technology to our portfolio, hospitals will soon be able to manufacture patient-specific PEEK implants at the point of care.”
Regulatory Challenges Abound
Regulatory oversight of POC AM/3DP is a hot topic and poses some unique challenges. For example, regulatory bodies are familiar with regulating medical device companies but not hospitals. As more hospitals began to manufacture their own medical devices in-house, regulators became concerned about how to do this and maintain patient safety. Over the last 10 years, regulatory bodies have been collaborating with industry and hospital experts to define how to best regulate the POC manufacturing of medical devices. To stimulate discussion and receive feedback from different stakeholders, in December 2021 the FDA published a discussion paper on 3D printing at the point of care.1 The paper does not constitute guidance; rather, its purpose is to gather input from the public to inform future policy development.“The discussion paper provides insight into our perspective of the benefits and challenges of 3D printing at hospitals and other points of care and presents a potential approach for regulatory oversight under various scenarios to inform future policy development,” stated William Maisel, director of the Office of Product Evaluation and Quality for the FDA’s Center for Devices and Radiological Health.
The FDA proposed three different scenarios for adopting POC AM:
- The POC uses a medical device production system (MDPS), which is a validated and approved turn-key solution that can be used at the POC to manufacture specific medical devices.
- The medical device manufacturer co-locates at the POC as one of its satellite sites and registers it with the FDA to manufacture approved devices.
- The POC chooses to be a legal manufacturer itself by getting approval from the FDA to manufacture its own devices at the POC.
“AM solution providers can help augment AM capabilities at the POC, based on these proposed scenarios,” Johnson noted. “We understand the regulatory bodies and guidance with oversight on additive manufacturing and can help healthcare providers stay compliant by:
- Establishing workflows and protocols for device design and manufacturing
- Building quality management programs to meet regulatory and safety requirements
- Setting up control processes to ensure auditable traceability and documentation.”
Moving Forward
POC AM/3DP has the potential to disrupt traditional medical device manufacturing and supply chain ecosystems. Hospitals and health systems becoming medical device manufacturers (MDMs) and manufacturing their own FDA-approved medical devices such as instruments, guides, and even implants is very likely in the near future. Increasingly, MDMs and healthcare systems collaborate to develop innovative new processes and business models that are focused on advancing POC manufacturing.There is no doubt that POC AM is gaining momentum throughout the healthcare environment. According to a survey commissioned by Axial3D, 52% of the surgeons interviewed indicated they had changed their plan for a complex surgery after using a 3D model during planning; 47% reported the models helped them confirm the optimal plan much faster and with more certainty, compared to relying solely on 2D patient scans. “Planning procedures, aided by 3D models, lead to an average reduction of 62 minutes per case, and an average reduction of stay in hospital for the patient of 16%,” indicated Johnston.
Pinchbeck added that some orthopedic surgeons prefer to practice their surgical procedures by going through the steps on anatomical models. “At several of our facilities, we have set up a simulation bench with a range of surgical tools and implants,” he said. “We then manufacture a model in appropriate materials and the surgeons can carry out test runs of the surgery on the models. This is hugely beneficial for implant sizing and also determining whether a custom-made implant is, or is not, required in a particular case. The simulation is even better when it is conducted in collaboration with the implant supplier, so that a full range of tools and implants are available at the onset of the simulation.”
Formlabs continues to see groundbreaking 3D printing applications as a next step toward wide-scale adoption. For example, it recently partnered with Vizient, one of the largest member-driven healthcare group purchasing organizations (GPO) in the nation, making it the first 3D printing company to be listed in a major GPO catalog.2 “This partnership reflects the increasing demand for 3D-printed surgical tools, medical supplies, and other solutions in hospitals and ambulatory surgical centers,” said Manchanda.
Even though the benefits of integrating POC AM/3DP into healthcare systems are clear, successful adoption of these technologies and services is dependent upon addressing a number of quality and compliance concerns, which remain the biggest challenges that POC AM/3DP faces today. In response, over the longer term, 3D Systems’ ultimate goal is to establish FDA-compliant medical device manufacturing centers of excellence at the point of care. Johnson indicated that overcoming facility, staffing, usage, and regulatory challenges at POC can be achieved through the aforementioned methods (i.e., establishing workflows, building quality management programs, and setting up control processes), plus:
- Deploying the right combination of technologies
- Providing ongoing staff education and procedural planning support
- Monitoring operational, production, and resource expenses to accurately assess expected impact on outcomes and cost savings
“I believe we will see more hospitals that will be able to implement end-to-end solutions for patient-specific surgical planning and medical device manufacturing,” said Johnson. “This will disrupt existing healthcare models, reduce overall costs, and crucially, improve the quality of care.”
The roles and responsibilities for hospitals versus industry for POC AM/3DP will continue to evolve in the coming years, especially as regulations, logistics, and business models change.
“As devices and technology become more advanced, we will see a shift toward more collaborative intelligence between physicians and engineers,” said De Boodt. “Bringing some personalization aspects closer to the point of care makes it easier for physicians to understand 3D printing’s benefits and limitations. Even now they continue to see new opportunities all the time and will continue to collaborate with engineers on new and better ways to personalize treatment for improved patient outcomes.”
References
Mark Crawford is a full-time freelance business and marketing/communications writer based in Madison, Wis. His clients range from startups to global manufacturing leaders. He also writes a variety of feature articles for regional and national publications and is the author of five books.