Sam Brusco, Associate Editor04.02.19
As of 2018, according to the Rheumatoid Arthritis Support Network, rheumatoid arthritis (RA) plagued over 1.3 million Americans, and up to one percent of the global population. Though the disease mainly attacks the joints’ synovial tissues, RA can affect the entire body and attack organs like the heart and lungs, or tissues like muscles, cartilage, and ligaments. RA causes chronic swelling and pain that can be severe and cause permanent damage.
RA patients’ pain manifests differently than neuropathic pain, requiring different treatment options. Usually, biologic therapies are used to treat RA’s underlying chronic inflammation and reduce the pain. Unfortunately, these therapies can suppress the immune system and may not always be effective, leading to refractory disease. There is, therefore, a huge need for treatments that are more effective, less immunosuppressive, and more cost-effective than current options.
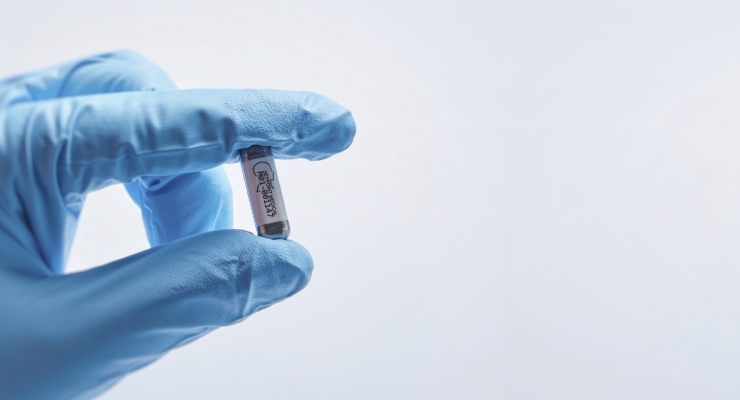
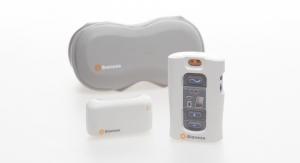
SetPoint Medical, a Valencia, Calif.-based bioelectronic medicine company dedicated to treating patients with chronic autoimmune diseases, is currently developing an implantable bioelectronic medicine platform to help treat RA and other inflammatory autoimmune diseases. Consisting of a small implantable MicroRegulator, a wireless charging collar or band, and an iPad-based prescription application, the less than one-inch long device recently completed its U.S. Pilot IDE study in patients with multi-drug refractory RA.
To gain more insight into how technology can help to curb or eliminate opioid use, I recently spoke with Murthy Simhambhatla, Ph.D., SetPoint Medical’s CEO. Some of his input is included in the pain management-focused cover story for the March/April issue of ODT, entitled “Pain, Pain, Go Away.” The full extent of Murthy’s comments are featured here.
Sam Brusco: Why is it important for medical technology to be part of a pain management regimen?
Murthy Simhambhatla: Pain management is a complex and highly variable condition that is largely individual for each patient, thus requiring unique and various treatment options. Patients with autoimmune diseases like RA often experience pain, but its manifestation is different from neuropathic pain, and thus may require different treatment options. Diseases like RA are often treated with biologic therapies to address the underlying inflammatory process. Improving this chronic inflammation has an impact on patients’ overall disease activity improvement, which could include reduction in their pain. However, biologic therapies can be immunosuppressive and are not always effective at treating RA patients, leading to refractory disease.
RA is an autoimmune and inflammatory disease in which a patient’s immune system, which normally attacks foreign bodies like viruses and bacteria, mistakenly attacks healthy cells in the body, causing inflammation (painful swelling) in the affected parts of the body, mainly the joints.
There is a major unmet need for novel treatment options for autoimmune diseases that are more efficacious, less immune-suppressive, and more cost-effective than current therapies.
Medical technology, including our unique bioelectronic medicine approach, has the opportunity to activate innate pathways in the body to better manage diseases like RA and the resulting pain, rather than subjecting patients to traditional drug therapies.
Brusco: What are the current problems with existing RA treatment?
Simhambhatla: Despite significant progress with pharmacological therapy, 30-50 percent of RA patients either don’t adequately respond to or are intolerant of biologic therapies. These therapies can have serious side effects and impose a significant cost burden on the healthcare system. In fact, some of the highest revenue grossing drugs in history are indicated for patients with RA and other inflammatory autoimmune diseases, and these drugs come with FDA black box warnings regarding serious side effects. Furthermore, patient compliance is a major issue as these drugs typically are injectable therapies.
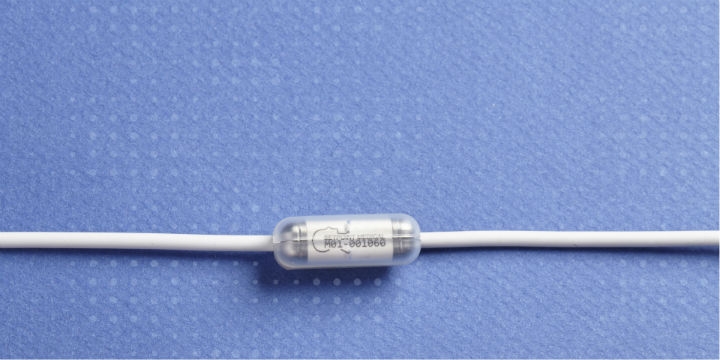
The technology shows promise as an alternative, efficient treatment option for RA, Crohn’s disease, and other chronic autoimmune diseases—that may reduce risk, lower cost, and improve patient adherence to therapy.
Brusco: How does SetPoint’s bioelectronic therapy technology work? How is it an improvement on existing treatment methods for RA?
Simhambhatla: We are pioneering the use of bioelectric medicine to fundamentally alter the treatment paradigm for autoimmune diseases. Bioelectronic medicine activates a natural physiologic pathway through vagus nerve stimulation to restore immunological homeostasis—or, return the body to its natural “set point.”
Compared to targeted biologics which aim to eliminate the bioavailability of a single pro-inflammatory cytokine, our approach has been shown to suppress a range of inflammatory cytokines by 30-70 percent without eliminating the bioavailability of any single cytokine. In doing so, we expect to reduce inflammation without causing significant immunosuppression, which is a major risk factor of almost all currently available therapies that aim to deplete the bioavailability of these cytokines.
SetPoint’s miniature (less than one inch long) bioelectronic medicine device is implanted on the left vagus nerve via a small incision in the neck. It delivers electrical impulses designed to activate the innate inflammatory reflex to produce a systemic anti-inflammatory effect and to help restore balance and regulate the immune system.
Brusco: Are you finding that clinicians, patients, and payors are embracing medical technology as a solution to managing RA?
Simhambhatla: We are still fairly early in the development of our therapy as we have just recently concluded the first pilot study for our device. We will need additional, larger studies to better define the safety and effectiveness of our therapy.
Brusco: What plans are in the future for SetPoint’s bioelectronic therapy system?
Simhambhatla: Most recently, we successfully completed our U.S. Pilot IDE Study in patients with multi-drug refractory RA. Overall, the results provide further validation of the mechanism of our novel device. The study indicated the device is safe and well-tolerated, and results were similar to the results from our prior European studies.
We anticipate initiating a larger clinical study to evaluate the safety and efficacy of our proprietary device in RA patients in the second half of 2019.
RA patients’ pain manifests differently than neuropathic pain, requiring different treatment options. Usually, biologic therapies are used to treat RA’s underlying chronic inflammation and reduce the pain. Unfortunately, these therapies can suppress the immune system and may not always be effective, leading to refractory disease. There is, therefore, a huge need for treatments that are more effective, less immunosuppressive, and more cost-effective than current options.
SetPoint Medical, a Valencia, Calif.-based bioelectronic medicine company dedicated to treating patients with chronic autoimmune diseases, is currently developing an implantable bioelectronic medicine platform to help treat RA and other inflammatory autoimmune diseases. Consisting of a small implantable MicroRegulator, a wireless charging collar or band, and an iPad-based prescription application, the less than one-inch long device recently completed its U.S. Pilot IDE study in patients with multi-drug refractory RA.
To gain more insight into how technology can help to curb or eliminate opioid use, I recently spoke with Murthy Simhambhatla, Ph.D., SetPoint Medical’s CEO. Some of his input is included in the pain management-focused cover story for the March/April issue of ODT, entitled “Pain, Pain, Go Away.” The full extent of Murthy’s comments are featured here.
Sam Brusco: Why is it important for medical technology to be part of a pain management regimen?
Murthy Simhambhatla: Pain management is a complex and highly variable condition that is largely individual for each patient, thus requiring unique and various treatment options. Patients with autoimmune diseases like RA often experience pain, but its manifestation is different from neuropathic pain, and thus may require different treatment options. Diseases like RA are often treated with biologic therapies to address the underlying inflammatory process. Improving this chronic inflammation has an impact on patients’ overall disease activity improvement, which could include reduction in their pain. However, biologic therapies can be immunosuppressive and are not always effective at treating RA patients, leading to refractory disease.
RA is an autoimmune and inflammatory disease in which a patient’s immune system, which normally attacks foreign bodies like viruses and bacteria, mistakenly attacks healthy cells in the body, causing inflammation (painful swelling) in the affected parts of the body, mainly the joints.
There is a major unmet need for novel treatment options for autoimmune diseases that are more efficacious, less immune-suppressive, and more cost-effective than current therapies.
Medical technology, including our unique bioelectronic medicine approach, has the opportunity to activate innate pathways in the body to better manage diseases like RA and the resulting pain, rather than subjecting patients to traditional drug therapies.
Brusco: What are the current problems with existing RA treatment?
Simhambhatla: Despite significant progress with pharmacological therapy, 30-50 percent of RA patients either don’t adequately respond to or are intolerant of biologic therapies. These therapies can have serious side effects and impose a significant cost burden on the healthcare system. In fact, some of the highest revenue grossing drugs in history are indicated for patients with RA and other inflammatory autoimmune diseases, and these drugs come with FDA black box warnings regarding serious side effects. Furthermore, patient compliance is a major issue as these drugs typically are injectable therapies.

The technology shows promise as an alternative, efficient treatment option for RA, Crohn’s disease, and other chronic autoimmune diseases—that may reduce risk, lower cost, and improve patient adherence to therapy.
Brusco: How does SetPoint’s bioelectronic therapy technology work? How is it an improvement on existing treatment methods for RA?
Simhambhatla: We are pioneering the use of bioelectric medicine to fundamentally alter the treatment paradigm for autoimmune diseases. Bioelectronic medicine activates a natural physiologic pathway through vagus nerve stimulation to restore immunological homeostasis—or, return the body to its natural “set point.”
Compared to targeted biologics which aim to eliminate the bioavailability of a single pro-inflammatory cytokine, our approach has been shown to suppress a range of inflammatory cytokines by 30-70 percent without eliminating the bioavailability of any single cytokine. In doing so, we expect to reduce inflammation without causing significant immunosuppression, which is a major risk factor of almost all currently available therapies that aim to deplete the bioavailability of these cytokines.
SetPoint’s miniature (less than one inch long) bioelectronic medicine device is implanted on the left vagus nerve via a small incision in the neck. It delivers electrical impulses designed to activate the innate inflammatory reflex to produce a systemic anti-inflammatory effect and to help restore balance and regulate the immune system.
Brusco: Are you finding that clinicians, patients, and payors are embracing medical technology as a solution to managing RA?
Simhambhatla: We are still fairly early in the development of our therapy as we have just recently concluded the first pilot study for our device. We will need additional, larger studies to better define the safety and effectiveness of our therapy.
Brusco: What plans are in the future for SetPoint’s bioelectronic therapy system?
Simhambhatla: Most recently, we successfully completed our U.S. Pilot IDE Study in patients with multi-drug refractory RA. Overall, the results provide further validation of the mechanism of our novel device. The study indicated the device is safe and well-tolerated, and results were similar to the results from our prior European studies.
We anticipate initiating a larger clinical study to evaluate the safety and efficacy of our proprietary device in RA patients in the second half of 2019.