Maria Shepherd, President and Founder, Medi-Vantage05.23.19
While total 2017 U.S. healthcare spending grew by 3.9 percent to $3.5 trillion,1 it was at a lower rate than the 4.8 percent increase reported by the U.S. Department of Health and Human Services in 2016. The 2017 growth rate correlates to the lower increases seen between 2008 and 2013, which preceded the more rapid spike during 2014 to 2015 (Table 1). This two-year segment of faster growth may be due to factors such as significant increases in prescription drug spending and insurance coverage patterns.
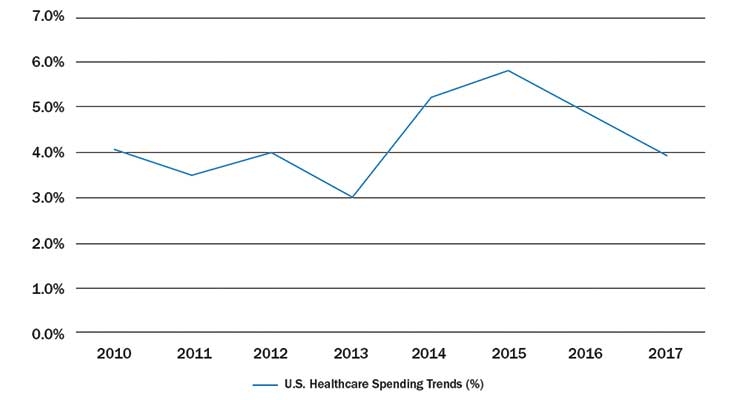
Table 1: Percentage change in recent U.S. healthcare spending trends2
Growth in healthcare spending declined slightly in 2017. The decrease was mainly attributed to a reduction in the consumption of goods and services, mainly in hospital care, clinician services, and prescription drugs. This has impacted almost all major insurers and other sponsors of healthcare, such as the federal government. Spending on healthcare grew by 3.9 percent on a per capita basis, reaching $10,739 in 2017.1 Gross domestic product (GDP) spent on healthcare remained at 17.9 percent in 2017, approximately the same as the share of GDP in 2016.1
Why This Is Important
According to the Kaiser Family Foundation (KFF), in 2017, Americans spent, on average, $10,224 on healthcare. While this source places the number at a slightly lower figure than the earlier reference, it still reflects almost two times as much as spent by most nations of equivalent economic status to the U.S. Per capita spending was $8,009 in Switzerland, $5,728 in Germany, $5,511 in Sweden, $5,440 in Austria, and $5,386 in the Netherlands, according to the KFF.3 The average per capita spend in this report, which focused on “comparable” countries, was $5,280, with France, Canada, Belgium, Japan, and Australia all registering below the Comparable Country Average (Table 2). The U.K. was last in this study with a per capita spend of $4,246.3
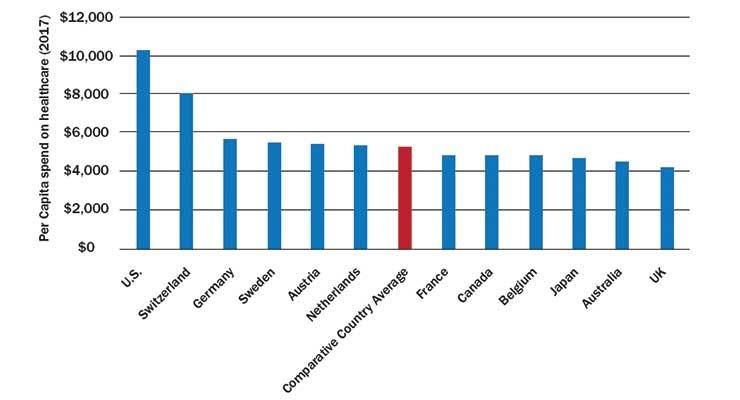
Table 2: Per capita spend on healthcare, by country (2017)3
What Part Does Orthopedics Play in the U.S. Healthcare Spend?
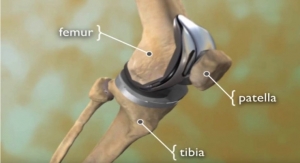
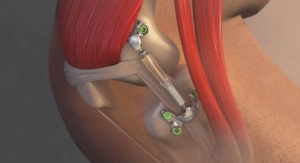
According to a report by Blue Cross Blue Shield4 (BCBS), planned hip and knee replacement surgeries are increasing in the U.S. The report identifies trends in cost and quality of care from 2010 through 2017 for elective hip replacements and total and partial knee replacements using an analysis performed on medical claims of BCBS commercially insured members.
In 2017, elective orthopedic procedures for BCBS commercially insured adult members cost the organization about $25 billion. Elective orthopedic procedures are estimated to be 47 percent of total spend for orthopedic treatments. Since 2010, this amount has grown approximately 44 percent.
Between 2010 to 2017, the greatest expensive increase has been the number of knee and hip procedures across all age segments of the BCBS insured population. For example, in 2017, 242,000 adult BCBS members below the age of 65 had a knee or hip implant.
Over this time frame, BCBS states procedures increased by 17 percent for knee replacements and 33 percent for hip replacements. Also, between 2010 to 2017, the average price for hip procedures grew by 5 percent and the average price for knee procedures grew by 6 percent. The inpatient costs for a knee replacement average $30,249. Hip replacements performed on an inpatient basis have an average price tag of $30,685 (Table 3).
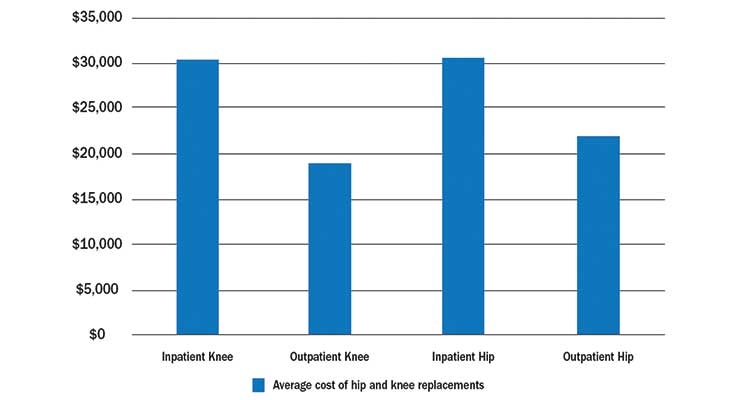
Table 3: Average cost of hip and knee replacements in the impatient and outpatient setting4
Largely ignored are the enormous savings for hip and knee procedures in the outpatient setting—a steep discount when compared to the inpatient setting. BCBS reported that a miniscule 11 percent of knees and 8 percent of hips were performed on an outpatient basis in 2017, at rates of $19,002 and $22,078, respectively.4 This isn’t due to complication rates in the outpatient setting. Rather, BCBS reports hip and knee complication rates for procedures performed in the outpatient setting between 2013 to 2017 have improved by 36 percent for hips and 23 percent for knees, and are superior to complication rates in the inpatient setting. These savings reach 30 percent to 40 percent over inpatient complication rates.
In this report, it is clear BCBS hasn’t been able to follow the lead of the Comprehensive Care for Joint Replacement Model (CJR) from the Center for Medicare & Medicaid Services, which claims to have had approximately 465 hospitals in 67 metropolitan statistical areas in the U.S. participating in the program as of Feb. 1, 20185. CJR holds participant hospitals financially responsible for a CJR episode of care and rewards improved care coordination between physicians, hospitals, and post-procedure care providers. Data reported6 for the cost of a procedure for MS-DRG 470—a major joint replacement or reattachment of lower extremity without fracture involvement and without major complications or comorbidities—averages $21,203. Granted, this is a best case scenario cost that averages the charges for hip and knee replacements, but it also represents a reduction in the overall cost of a procedure.
The Medi-Vantage Perspective
The data show hip and knee replacement costs can be managed, but many hospitals (at least for private payers) are not actively managing these costs. Perhaps the medical device industry could employ a strategy of vertically integrating by buying outpatient orthopedic facilities and negotiating with payers to have their members’ hip and knee replacement procedures performed there. It would certainly be an effective way to grow or maintain market share and it would also serve as a disruptive strategy in the orthopedic device industry.
References
Maria Shepherd has more than 20 years of leadership experience in medical device/life science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical, where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing, business strategy, and innovation research for the medical device, diagnostic, and digital health industries. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.aligo.com). She can be reached at 855-343-3100. Visit her website at www.medi-vantage.com.

Table 1: Percentage change in recent U.S. healthcare spending trends2
Growth in healthcare spending declined slightly in 2017. The decrease was mainly attributed to a reduction in the consumption of goods and services, mainly in hospital care, clinician services, and prescription drugs. This has impacted almost all major insurers and other sponsors of healthcare, such as the federal government. Spending on healthcare grew by 3.9 percent on a per capita basis, reaching $10,739 in 2017.1 Gross domestic product (GDP) spent on healthcare remained at 17.9 percent in 2017, approximately the same as the share of GDP in 2016.1
Why This Is Important
According to the Kaiser Family Foundation (KFF), in 2017, Americans spent, on average, $10,224 on healthcare. While this source places the number at a slightly lower figure than the earlier reference, it still reflects almost two times as much as spent by most nations of equivalent economic status to the U.S. Per capita spending was $8,009 in Switzerland, $5,728 in Germany, $5,511 in Sweden, $5,440 in Austria, and $5,386 in the Netherlands, according to the KFF.3 The average per capita spend in this report, which focused on “comparable” countries, was $5,280, with France, Canada, Belgium, Japan, and Australia all registering below the Comparable Country Average (Table 2). The U.K. was last in this study with a per capita spend of $4,246.3

Table 2: Per capita spend on healthcare, by country (2017)3
What Part Does Orthopedics Play in the U.S. Healthcare Spend?
According to a report by Blue Cross Blue Shield4 (BCBS), planned hip and knee replacement surgeries are increasing in the U.S. The report identifies trends in cost and quality of care from 2010 through 2017 for elective hip replacements and total and partial knee replacements using an analysis performed on medical claims of BCBS commercially insured members.
In 2017, elective orthopedic procedures for BCBS commercially insured adult members cost the organization about $25 billion. Elective orthopedic procedures are estimated to be 47 percent of total spend for orthopedic treatments. Since 2010, this amount has grown approximately 44 percent.
Between 2010 to 2017, the greatest expensive increase has been the number of knee and hip procedures across all age segments of the BCBS insured population. For example, in 2017, 242,000 adult BCBS members below the age of 65 had a knee or hip implant.
Over this time frame, BCBS states procedures increased by 17 percent for knee replacements and 33 percent for hip replacements. Also, between 2010 to 2017, the average price for hip procedures grew by 5 percent and the average price for knee procedures grew by 6 percent. The inpatient costs for a knee replacement average $30,249. Hip replacements performed on an inpatient basis have an average price tag of $30,685 (Table 3).

Table 3: Average cost of hip and knee replacements in the impatient and outpatient setting4
Largely ignored are the enormous savings for hip and knee procedures in the outpatient setting—a steep discount when compared to the inpatient setting. BCBS reported that a miniscule 11 percent of knees and 8 percent of hips were performed on an outpatient basis in 2017, at rates of $19,002 and $22,078, respectively.4 This isn’t due to complication rates in the outpatient setting. Rather, BCBS reports hip and knee complication rates for procedures performed in the outpatient setting between 2013 to 2017 have improved by 36 percent for hips and 23 percent for knees, and are superior to complication rates in the inpatient setting. These savings reach 30 percent to 40 percent over inpatient complication rates.
In this report, it is clear BCBS hasn’t been able to follow the lead of the Comprehensive Care for Joint Replacement Model (CJR) from the Center for Medicare & Medicaid Services, which claims to have had approximately 465 hospitals in 67 metropolitan statistical areas in the U.S. participating in the program as of Feb. 1, 20185. CJR holds participant hospitals financially responsible for a CJR episode of care and rewards improved care coordination between physicians, hospitals, and post-procedure care providers. Data reported6 for the cost of a procedure for MS-DRG 470—a major joint replacement or reattachment of lower extremity without fracture involvement and without major complications or comorbidities—averages $21,203. Granted, this is a best case scenario cost that averages the charges for hip and knee replacements, but it also represents a reduction in the overall cost of a procedure.
The Medi-Vantage Perspective
The data show hip and knee replacement costs can be managed, but many hospitals (at least for private payers) are not actively managing these costs. Perhaps the medical device industry could employ a strategy of vertically integrating by buying outpatient orthopedic facilities and negotiating with payers to have their members’ hip and knee replacement procedures performed there. It would certainly be an effective way to grow or maintain market share and it would also serve as a disruptive strategy in the orthopedic device industry.
References
- http://bit.ly/odt190601
- http://bit.ly/odt190602
- http://bit.ly/odt190603
- http://bit.ly/odt190604
- http://bit.ly/odt190605
- http://bit.ly/odt190606
Maria Shepherd has more than 20 years of leadership experience in medical device/life science marketing in small startups and top-tier companies. After her industry career, including her role as vice president of marketing for Oridion Medical, where she boosted the company valuation prior to its acquisition by Covidien/Medtronic, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing, business strategy, and innovation research for the medical device, diagnostic, and digital health industries. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.aligo.com). She can be reached at 855-343-3100. Visit her website at www.medi-vantage.com.