UC Davis Health System04.26.16
As part of a multicenter clinical trial, UC Davis Health System researchers are testing whether a novel stem cell treatment can reduce the pain and mobility issues caused by degenerative disc disease. UC Davis is one of 25 sites nationwide—and the only academic healthcare system in California—involved in the study.
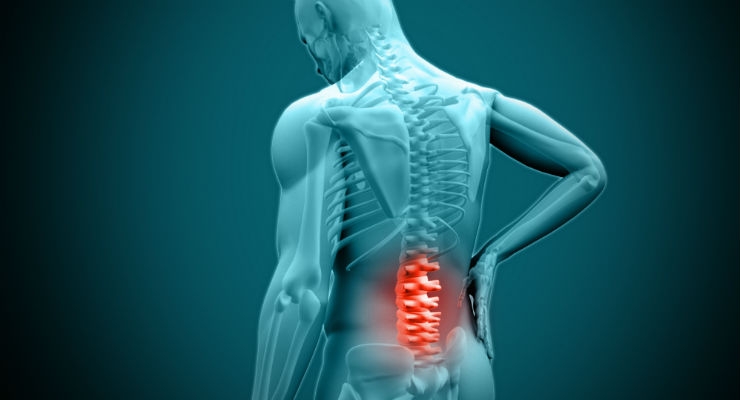
Disc degeneration occurs when the cushions between vertebrae wear down, a natural part of aging that for most causes no symptoms. Those with degenerative disc disease, however, can experience serious, chronic, and disabling low-back pain.
“Patients with this level of degeneration often try multiple treatments for relief, including pain medication, massage, physical therapy, chiropractic adjustments, and acupuncture,” said study principal investigator Kee Kim, professor of neurological surgery and co-director of the UC Davis Spine Center. “For some of them, nothing seems to help, and we end up operating to remove the degenerated disc and fuse the spine to eliminate motion that may cause increased pain. We want to know if a single dose of this investigational therapy can offer relief without the need for surgery.”
Kim and co-principal investigator David Copenhaver, assistant professor of pain medicine, are recruiting patients with lower back degenerative disc disease for the study. Participants will receive a single injection to the site of their pain with one of three treatments: mesenchymal precursor cells (MPCs), MPCs combined with a carrier material (hyaluronic acid), or a placebo. The goal of the trial is to assess the safety and efficacy of the therapy.
Research has shown that MPCs can target damaged tissue and induce healing by organizing cells to form new tissue. The MPCs used in this study are isolated from the bone marrow of healthy donors, and then expanded and amplified to generate readily available therapeutic doses for use in patients without the need for tissue matching.
Following treatment, participants will receive six evaluations at the UC Davis Spine Center in Sacramento over the course of a year. They also will be given the option to participate in an extension of the study to track their progress for three years after the initial injection.
This phase III study follows up on a successful phase II trial, also conducted at UC Davis, which involved fewer patients. The phase II results were encouraging and support the current phase III program, according to Kim.
If the current trial has positive outcomes, it will support the clinical program with a goal to seek approval from the U.S. Food and Drug Administration, and if successful, would make the therapy more widely available. Still, even if the trial succeeds, MPC injections will not be the answer for all patients.
“Many patients with back pain will not benefit from this stem cell therapy and may still require surgery,” Kim said. “For some patients, however, it could offer improvement. For these patients it is worth exploring this alternative.”
Disc degeneration occurs when the cushions between vertebrae wear down, a natural part of aging that for most causes no symptoms. Those with degenerative disc disease, however, can experience serious, chronic, and disabling low-back pain.
“Patients with this level of degeneration often try multiple treatments for relief, including pain medication, massage, physical therapy, chiropractic adjustments, and acupuncture,” said study principal investigator Kee Kim, professor of neurological surgery and co-director of the UC Davis Spine Center. “For some of them, nothing seems to help, and we end up operating to remove the degenerated disc and fuse the spine to eliminate motion that may cause increased pain. We want to know if a single dose of this investigational therapy can offer relief without the need for surgery.”
Kim and co-principal investigator David Copenhaver, assistant professor of pain medicine, are recruiting patients with lower back degenerative disc disease for the study. Participants will receive a single injection to the site of their pain with one of three treatments: mesenchymal precursor cells (MPCs), MPCs combined with a carrier material (hyaluronic acid), or a placebo. The goal of the trial is to assess the safety and efficacy of the therapy.
Research has shown that MPCs can target damaged tissue and induce healing by organizing cells to form new tissue. The MPCs used in this study are isolated from the bone marrow of healthy donors, and then expanded and amplified to generate readily available therapeutic doses for use in patients without the need for tissue matching.
Following treatment, participants will receive six evaluations at the UC Davis Spine Center in Sacramento over the course of a year. They also will be given the option to participate in an extension of the study to track their progress for three years after the initial injection.
This phase III study follows up on a successful phase II trial, also conducted at UC Davis, which involved fewer patients. The phase II results were encouraging and support the current phase III program, according to Kim.
If the current trial has positive outcomes, it will support the clinical program with a goal to seek approval from the U.S. Food and Drug Administration, and if successful, would make the therapy more widely available. Still, even if the trial succeeds, MPC injections will not be the answer for all patients.
“Many patients with back pain will not benefit from this stem cell therapy and may still require surgery,” Kim said. “For some patients, however, it could offer improvement. For these patients it is worth exploring this alternative.”